- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Coronary stenting may not benefit patients of CAD with severe left ventricular dysfunction
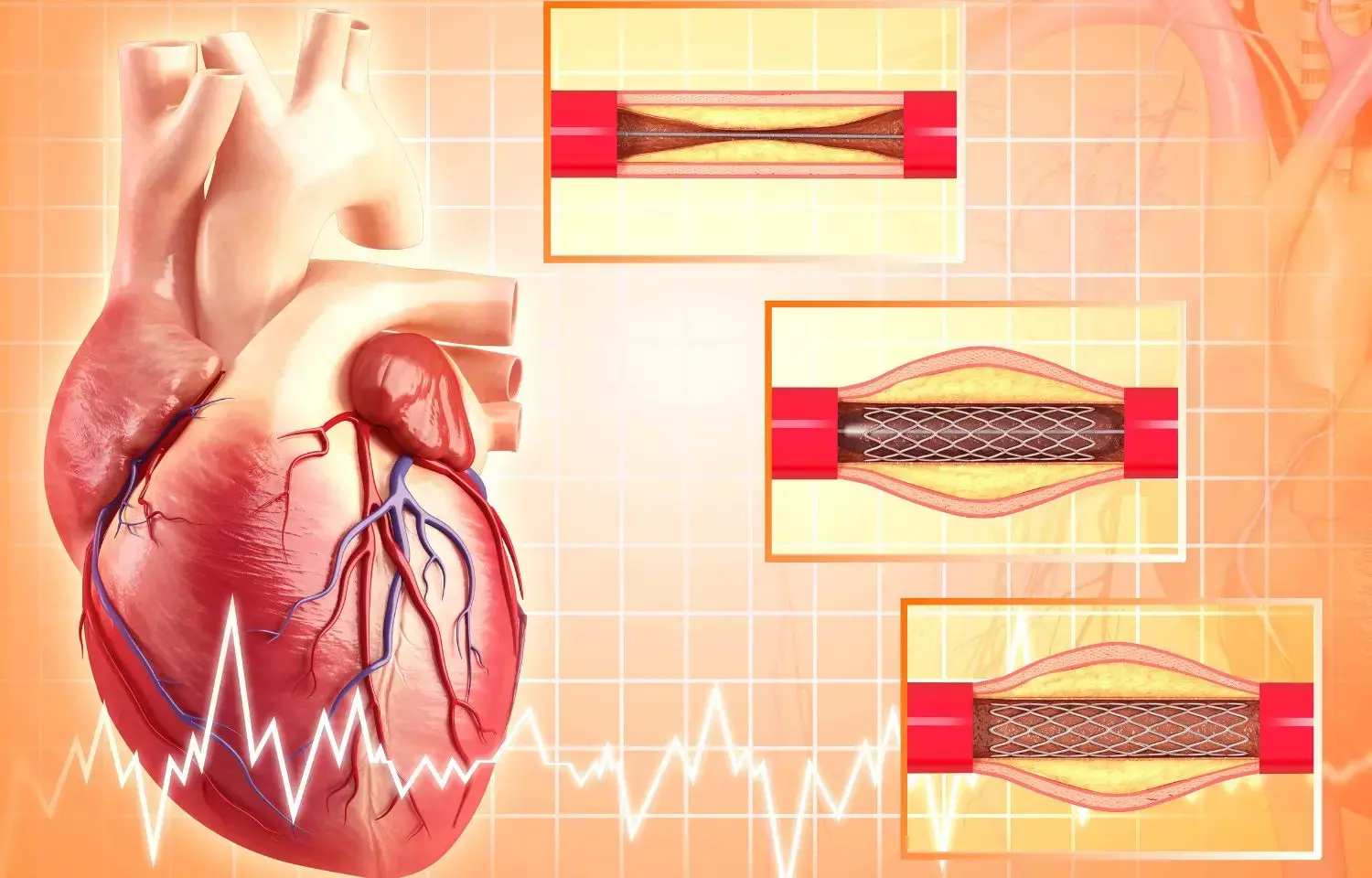
Researchers have found in a new study that among patients with severe left ventricular dysfunction and extensive coronary artery disease, Percutaneous coronary intervention (PCI) does not reduce all-cause mortality or heart failure hospitalisation.
The late breaking research was presented in a Hot Line session at ESC Congress 2022.
Coronary artery disease is the most common cause of heart failure and is associated with poor survival and low quality of life despite advances in medical therapy.2 Treating the coronary arteries to improve blood supply (revascularisation) has long been considered as a treatment option in this population.
In the STICH trial, coronary artery bypass surgery improved survival but only in highly selected, typically young, patients.3 However, the benefit took 10 years to emerge, largely due to the early harm of the operation. PCI was an attractive alternative to bypass surgery, as it might offer the benefits of revascularisation without the early hazard. However, there was no randomised evidence to support this and guidelines recommending the use of this treatment in some patients were based only on expert opinion.
REVIVED-BCIS2 is the first adequately powered randomised trial to examine the efficacy and safety of PCI in patients with left ventricular systolic dysfunction.5 The trial enrolled patients with severe left ventricular dysfunction (ejection fraction 35% or below), extensive coronary artery disease and demonstrable viability in at least four dysfunctional myocardial segments that could be revascularised by PCI.
Viability could be assessed by any modality, but cardiac magnetic resonance imaging was used most. Those with a myocardial infarction within four weeks, decompensated heart failure or sustained ventricular arrhythmias within 72 hours were excluded.
A total of 700 patients from 40 centres in the UK were randomly assigned in a 1:1 ratio to either PCI with optimal medical therapy or optimal medical therapy alone.
The median age of participants was 70 years, 88% were men and the mean left ventricular ejection fraction was 28%. The primary outcome was the composite of all-cause death or hospitalisation for heart failure. Secondary outcomes included left ventricular ejection fraction at six and 12 months and quality of life measures.
During a median follow up of 3.4 years, the primary outcome occurred in 129 (37.2%) patients in the PCI group and 134 (38.0%) patients in the medical therapy alone group for a hazard ratio of 0.99 (95% confidence interval 0.78–1.27, p=0.96).
Chief Investigator Professor Divaka Perera of King's College London, UK said: "PCI provided no incremental benefit over optimal medical therapy, in this high-risk population, where approximately one in three patients died or were hospitalised with heart failure during follow-up."
No significant difference was seen between groups in the major secondary outcome of the trial, left ventricular ejection fraction at six and 12 months. Given that only patients with demonstrable myocardial viability were enrolled, the latter finding challenges the concept of myocardial hibernation, which for decades has been considered an adaptation of the heart to cope with the effects of severe coronary disease, that can be reversed by treating the coronary disease.
Quality of life (the other major secondary outcome) favoured PCI at six and 12 months but there was no difference between groups at 24 months.
Professor Perera said: "We can conclude that PCI should not be offered to stable patients with ischaemic left ventricular dysfunction if the sole aim is to provide prognostic benefit. Our findings were consistent across all subgroups and for all prespecified outcome measures. These definitive results should help to rationalise guidelines on managing coronary disease in patients with very poor left ventricular function.
However, it is important to note that REVIVED-BCIS2 excluded patients with limiting angina or recent acute coronary syndromes, and PCI is still an option in these contexts."
Reference:
1. Ryan M, Morgan H, Petrie MC, Perera D. Coronary revascularisation in patients with ischaemic cardiomyopathy. Heart. 2021. doi:10.1136/heartjnl-2020-316856.
2. Velazquez EJ, Lee KL, Jones RH, et al. Coronary-artery bypass surgery in patients with ischemic cardiomyopathy. N Engl J Med. 2016;374:1511–1520.
3. Neumann FJ, Sousa-Uva M, Ahlsson A, et al. 2018 ESC/EACTS Guidelines on myocardial revascularization. Eur Heart J. 2019;40:87–165.
4. Perera D, Clayton T, Petrie MC, et al. Percutaneous revascularization for ischemic ventricular dysfunction: Rationale and design of the REVIVED-BCIS2 trial. J Am Coll Cardiol HF. 2018;6:517-526.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


