- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Sedation may not improve survival in ventilated ICU patients: NON-SEDA trial
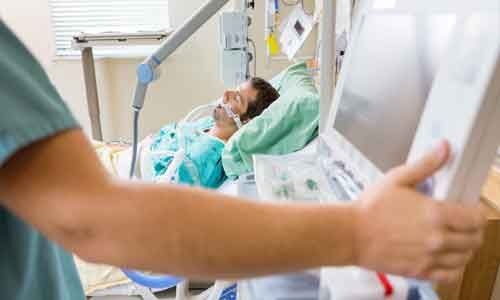
Denmark: Mechanically ventilated patients in the ICU who received no sedation had similar 90-day mortality compared to the patients who were assigned to a plan of light sedation with daily interruption, according to findings from the NON-SEDA trial published in the NEJM journal.
Daily interruption of sedation in critically ill, mechanically ventilated patients has been shown to reduce the ventilation time and length of stay in the ICU. However, there is a lack of data on whether a plan of no sedation, as compared with a plan of light sedation, has an effect on mortality.
To determine the same, Palle Toft, Odense University Hospital, Denmark, and colleagues conducted this multicenter, randomized, controlled trial. A total of 710 mechanically ventilated ICU patients underwent randomization. They were assigned in the ratio 1:1 to a plan of no sedation (nonsedation group) or to a plan of light sedation (sedation group). In the sedatuion group, the patients were sedated to a level at which the patient was arousable, defined as a score of −2 to −3 on the Richmond Agitation and Sedation Scale [RASS], on which scores range from −5 [unresponsive] to +4 [combative]) with daily interruption.
The primary outcome was mortality at 90 days. Secondary outcomes were the number of major thromboembolic events, the number of days free from coma or delirium, acute kidney injury according to severity, the number of ICU-free days, and the number of ventilator-free days. Between-group differences were calculated as the value in the nonsedation group minus the value in the sedation group.
Key findings of the study include:
- The characteristics of the patients at baseline were similar in the two trial groups, except for the score on the Acute Physiology and Chronic Health Evaluation (APACHE) II, which was 1 point higher in the nonsedation group than in the sedation group, indicating a greater chance of in-hospital death.
- The mean RASS score in the nonsedation group increased from −1.3 on day 1 to −0.8 on day 7 and, in the sedation group, from −2.3 on day 1 to −1.8 on day 7.
- Mortality at 90 days was 42.4% in the nonsedation group and 37.0% in the sedated group (difference, 5.4 percentage points).
- The number of ICU-free days and of ventilator-free days did not differ significantly between the trial groups.
- The patients in the nonsedation group had a median of 27 days free from coma or delirium, and those in the sedation group had a median of 26 days free from coma or delirium.
- A major thromboembolic event occurred in 1 patient (0.3%) in the nonsedation group and in 10 patients (2.8%) in the sedation group (difference, −2.5 percentage points).
According to the authors, the findings are important as they arouse concern about omitting sedation in mechanically ventilated patients and reinforce the need to monitor sedation clinically with the aim of discontinuing it as early as possible or at least interrupting it daily.
"Such monitoring should be performed continuously (24 hours per day, every day) on the basis of standardized criteria that can be applied uniformly in an ICU," they concluded.
The study, "Nonsedation or Light Sedation in Critically Ill, Mechanically Ventilated Patients," is published in The New England Journal of Medicine.
MSc. Biotechnology
Medha Baranwal holds a Bachelor’s degree in Biomedical Sciences from the University of Delhi and a Master’s degree in Biotechnology from Amity University. Since May 2018, she has been contributing to Medical Dialogues, writing and editing medical news articles that translate complex research into clear, accessible information for healthcare professionals.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


