- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Poor maintenance of implant hygiene associated with peri-implant diseases: Study
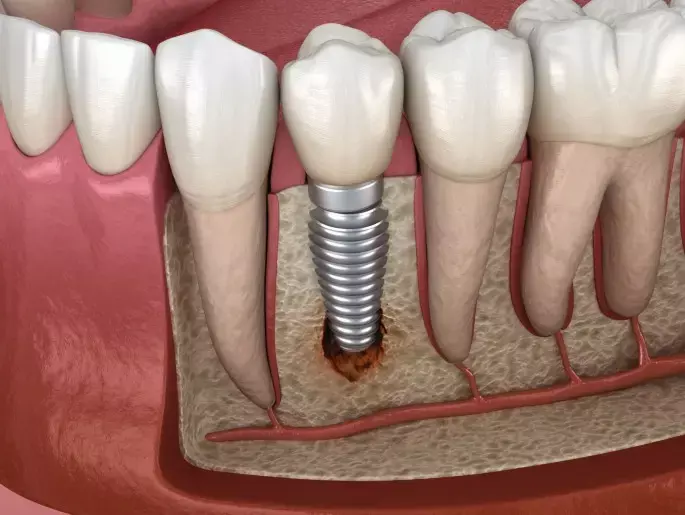
Peri-implant diseases are known as undesirable conditions that can occur after implant therapy. Although several risk indicators are becoming clear, the causes of peri-implant diseases have not been completely investigated.
Poor patient-performed implant hygiene associated with peri-implant diseases, according to a recent study published in the Australian Dental Journal.
Peri-implant diseases are inflammatory conditions affecting the soft and hard gum tissues around dental implants. Similar to a natural tooth, bacteria can build up on the base of the implant, below the gum line.
This study investigated the possible correlations between patient-performed implant hygiene and peri-implant success and disease, as well as patient-reported outcomes, in a community-based cohort.
Fifty-one patients (78 implants) from two private general practices were surveyed on their dental implant treatment history, oral hygiene instructions (OHI) received, home hygiene habits and current implant concerns. Their dentition, plaque/calculus scores and clinical implant parameters were examined. Correlations between hygiene habits, risk factors, implant success and peri-implant disease rates were assessed.
The Results of the study are as follows:
Implants had a patient-reported mean time in function of 6.7 years. Floss (74.4%), interdental brushes (IDB) (44.9%) and mouthwash (39.7%) were commonly used, while 7.7% of implants were only cleaned by brushing. Over half (56.4%) of implants fulfilled the success criteria, 61.5% had peri-implant health, 24.4% had mucositis and 7.7% had peri-implantitis. Only brushing (P < 0.001) and detectable plaque/calculus (P < 0.001) were significantly associated with more peri-implant disease. Local prosthetic factors affecting cleaning accessibility significantly reduced implant success (P < 0.001). Patients reported mixed recall of implant oral hygiene instructions (OHI), 7.7% of implants were aesthetically unsatisfactory and 9.0% had peri-implant symptoms.
Thus, the researchers concluded that the lack of interproximal cleaning and the presence of plaque/calculus were significantly associated with peri-implant disease in a community-based general practice setting, and patients reported mixed recall of oral hygiene instructions (OHI).
Reference:
Patient-reported oral hygiene and implant outcomes in general dental practice by Monique Charlene Cheung et al. published in the Australian Dental Journal.
https://doi.org/10.1111/adj.12806
Dr. Shravani Dali has completed her BDS from Pravara institute of medical sciences, loni. Following which she extensively worked in the healthcare sector for 2+ years. She has been actively involved in writing blogs in field of health and wellness. Currently she is pursuing her Masters of public health-health administration from Tata institute of social sciences. She can be contacted at editorial@medicaldialogues.in.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


