- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Tirbanibulin ointment effective in actinic keratosis of face, scalp for short period: NEJM
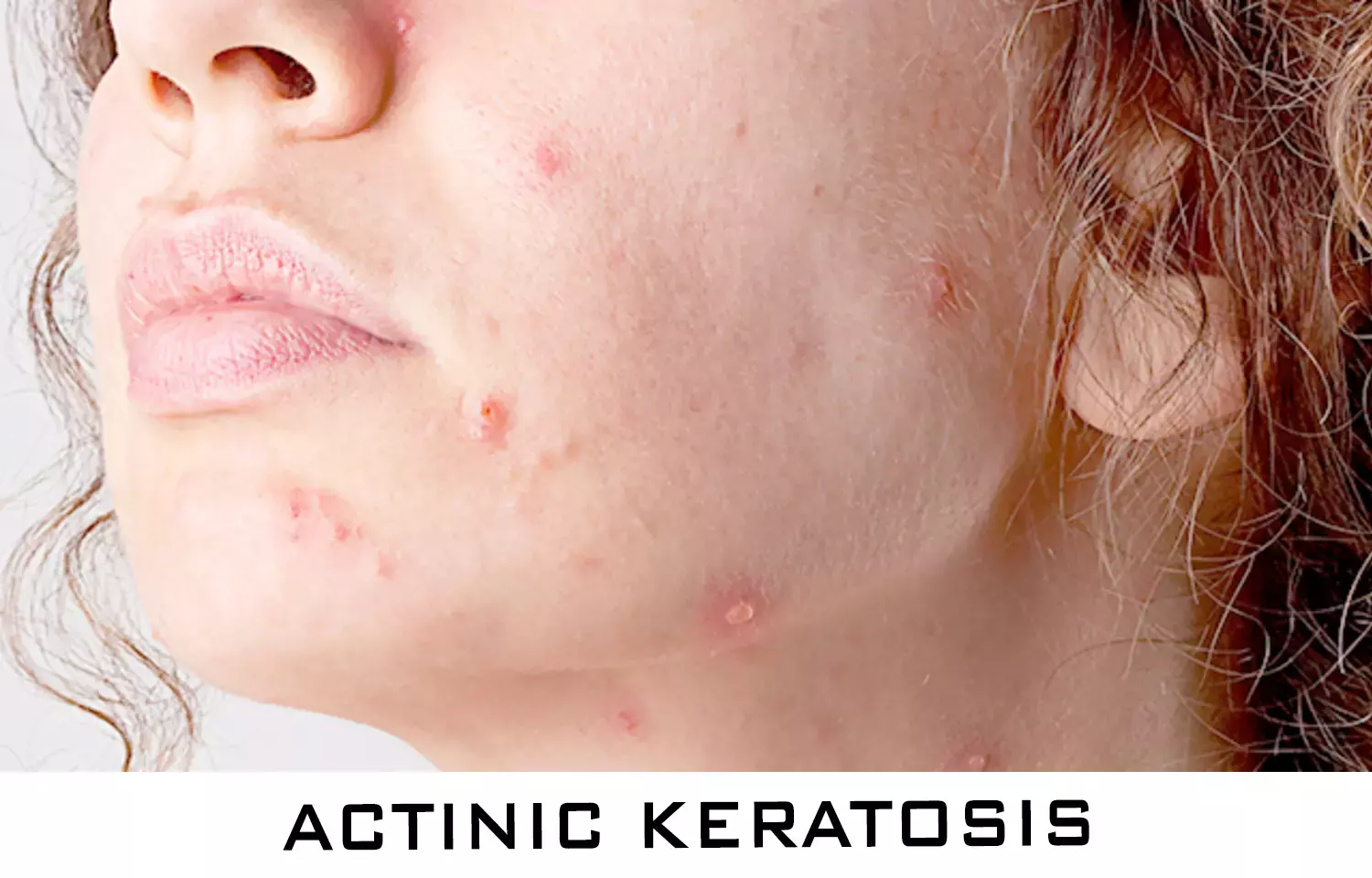
USA: Once daily application of tirbanibulin 1% ointment for 5 days was superior to vehicle (placebo) ointment for the treatment of actinic keratosis on the scalp and face for 2 months, finds a recent study in the New England Journal of Medicine. But tirbanibulin use was associated with a recurrence of lesions at 1 year and transient local reactions
Actinic keratosis is a common precancerous condition caused by years of sun exposure. It occurs particularly on the face, scalp, arms, and legs. The condition commonly affects men, people with fair skin, older people, and people with a history of prolonged exposure to ultraviolet light. If left untreated, the condition may progress to invasive cutaneous squamous-cell carcinoma. The reported risk of progression ranges from 0.025 to 16% per lesion per year. Given its unpredictable nature of progression, it has been recommended to treat all actinic keratoses.
The tubulin polymerization and Src kinase signaling inhibitor tirbanibulin is being investigated as a topical treatment for actinic keratosis, a precursor of squamous-cell carcinoma.
Andrew Blauvelt, Austin Institute for Clinical Research, Pflugerville, Texas, and colleagues present in this study, the results of two identically designed phase 3 trials that evaluated the safety and efficacy of tirbanibulin ointment, as compared with vehicle ointment, applied for 5 days in adults with actinic keratoses on the face or scalp.
The two trials included adults (n=702; 351 patients per trial) with actinic keratoses on the face or scalp. They were randomly assigned in the ratio 1:1 to receive either topical tirbanibulin or vehicle (placebo) ointment. The ointment was applied by the patients to a 25-cm2 contiguous area containing four to eight lesions once daily for 5 consecutive days.
The primary outcome was the percentage of patients with a complete (100%) reduction in the number of lesions in the application area at day 57. The secondary outcome was the percentage of patients with a partial (≥75%) reduction in the number of lesions within the application area at day 57. The incidence of recurrence was evaluated at 1 year. Local reactions were scored with the use of 4-point scale (ranging from 0 [absent] to 3 [severe]).
Key findings of the study include:
- Complete clearance in trial 1 occurred in 44% of the patients (77 of 175) in the tirbanibulin group and in 5% of those (8 of 176) in the vehicle group; in trial 2, the percentages were 54% (97 of 178 patients) and 13% (22 of 173), respectively.
- The percentages of patients with partial clearance were significantly higher in the tirbanibulin groups than in the vehicle groups.
- At 1 year, the estimated percentage of patients with recurrent lesions was 47% among patients who had had a complete response to tirbanibulin.
- The most common local reactions to tirbanibulin were erythema in 91% of the patients and flaking or scaling in 82%.
- Adverse events with tirbanibulin were application-site pain in 10% of the patients and pruritus in 9%, all of which resolved.
"In two identically designed trials, tirbanibulin 1% ointment applied once daily for 5 days was superior to vehicle for the treatment of actinic keratosis at 2 months but was associated with transient local reactions and recurrence of lesions at 1 year," wrote the authors.
"Larger and longer trials are necessary to determine the effects and risks of tirbanibulin therapy among patients with actinic keratosis," they concluded.
Reference:
The study titled, "Phase 3 Trials of Tirbanibulin Ointment for Actinic Keratosis," is published in the New England Journal of Medicine.
DOI: https://www.nejm.org/doi/full/10.1056/NEJMoa2024040
MSc. Biotechnology
Medha Baranwal holds a Bachelor’s degree in Biomedical Sciences from the University of Delhi and a Master’s degree in Biotechnology from Amity University. Since May 2018, she has been contributing to Medical Dialogues, writing and editing medical news articles that translate complex research into clear, accessible information for healthcare professionals.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


