- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Microvascular Reconstruction of Osteonecrosis associated with good return of function and QOL: AAOHN
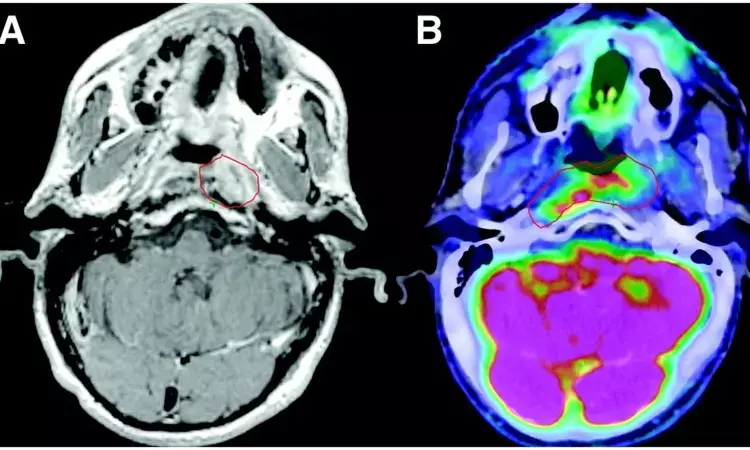
Osteonecrosis of the head and neck region is often a debilitating condition with negative impacts on quality of life (QOL). Advanced osteonecrosis of the head and neck is often associated with uncontrolled pain, chronic draining fistulas, impaired mastication, diet limitations, dissatisfaction with cosmesis, and pathologic fractures. When compared with patients who did not develop osteonecrosis following treatment, those with osteonecrosis reported greater pain, dissatisfaction with appearance, and reduction in activity. In addition, patients with osteonecrosis reported worse swallowing and chewing function.
The majority of osteonecrosis in the head and neck region is due to previous radiation therapy, referred to as osteoradionecrosis (ORN), while a small subset of head and neck osteonecrosis occurs following prolonged bisphosphonate therapy (bisphosphonate-related osteonecrosis of the jaw [BRONJ]). ORN has been defined as persistent bone exposure following radiation therapy that fails to heal after 3 months and is without evidence of recurrent malignancy.
Conservative treatment is often offered initially to patients who present with osteonecrosis of the head and neck region, with resection of involved bone and microvascular free flap reconstruction reserved for advanced disease that has failed to resolve with more conservative therapy. Currently there are limited publications assessing long-term outcomes and QOL for patients following microvascular reconstruction for advanced osteonecrosis of the head and neck region. Sweeny et al conducted a multi-institutional Retrospective review of a large cohort of patients at tertiary care centers to evaluate long-term outcomes and QOL.
Patients included those undergoing free flap reconstructions for osteonecrosis of the head and neck (N = 232). Data included demographics, defect, donor site, radiation history, perioperative management, diet status, recurrence rates, and long-term quality-of-life outcomes. Quality of-life outcomes were measured using the University of Washington Quality of Life (UW-QOL) survey.
- Overall flap success rate was 91% (n = 212). Relative to preoperative diet, 15% reported improved diet function at 3 months following reconstruction and 26% at 5 years.
- Osteonecrosis recurred in 14% of patients (32/232); median time to onset was 11 months.
- Cancer recurrence occurred in 13% of patients (29/232); median time to onset was 34 months.
- Results from the UW-QOL questionnaire were as follows: no pain (45%), minor or no change in appearance (69%), return to baseline endurance level (37%), no limitations in recreation (40%), no changes in swallowing following reconstruction (28%), minor or no limitations in mastication (29%), minor or no speech difficulties (93%), no changes in shoulder function (84%), normal taste function (19%), normal saliva production (27%), generally excellent mood (44%), and no or minimal anxiety about cancer (94%).
Osteonecrosis has significant QOL implications, including pain, infection, draining fistula, and/or pathologic fracture, which must be factored into the decision-making process. While some patients with osteonecrosis can be treated conservatively (antibiotics, local tissue debridement), a subset does not improve and requires more aggressive therapy. This typically results in the need for surgical resection of the affected bone and soft tissues, followed by reconstruction with a microvascular free flap.
The intent of surgical intervention is to improve patient QOL via reduction or elimination of pain, resolution of a salivary fistula, and/or improved function. The decision to proceed with resection of the involved bone and microvascular free flap for osteonecrosis involves careful consideration of a multitude of challenging factors. These factors include comorbid conditions, history of radiation therapy to the operating field, previous operation at the surgical site, economic burden, and patient expectations. These procedures are demanding not only for the performing surgeon and patient but also on the health care system with significant resource utilization and cost. Subsequently, there is a growing need for objective outcome measures quantifying longterm outcomes and impacts on QOL.
Osteonecrosis pain is thought to be the result of exposed nerve endings within a nonhealing wound to infection and inflammation. Vascular free flaps improve blood flow to the area and provide coverage for exposed nerve ending.
"To our knowledge, the series reported here is the largest to date on long-term outcomes and QOL in patients with osteonecrosis of the head and neck requiring free flap reconstruction. The majority of patients in this study had advancement or maintenance of diet function following reconstruction, with low rates of osteonecrosis or cancer recurrence and above-average scores on the UW-QOL survey suggesting good return of function and QOL. We found that UW-QOL domain scores following free flap reconstructions were higher for those who received dental implants, did not have a history of head and neck surgery, and did not develop a cancer recurrence. Outcomes data for patients undergoing microvascular reconstruction for osteonecrosis of the head and neck are essential for management, counseling, and the assessment of quality. The results of studies such as this one contribute to the basis of informed discussions with patients regarding expectations and anticipated outcomes."
Source: Sweeny et al; Otolaryngology– Head and Neck Surgery
DOI: 10.1177/0194599821990682
Dr Ishan Kataria has done his MBBS from Medical College Bijapur and MS in Ophthalmology from Dr Vasant Rao Pawar Medical College, Nasik. Post completing MD, he pursuid Anterior Segment Fellowship from Sankara Eye Hospital and worked as a competent phaco and anterior segment consultant surgeon in a trust hospital in Bathinda for 2 years.He is currently pursuing Fellowship in Vitreo-Retina at Dr Sohan Singh Eye hospital Amritsar and is actively involved in various research activities under the guidance of the faculty.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


