- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Fortis Gurgaon surgeons repair fused jaw bones of a 21-year old
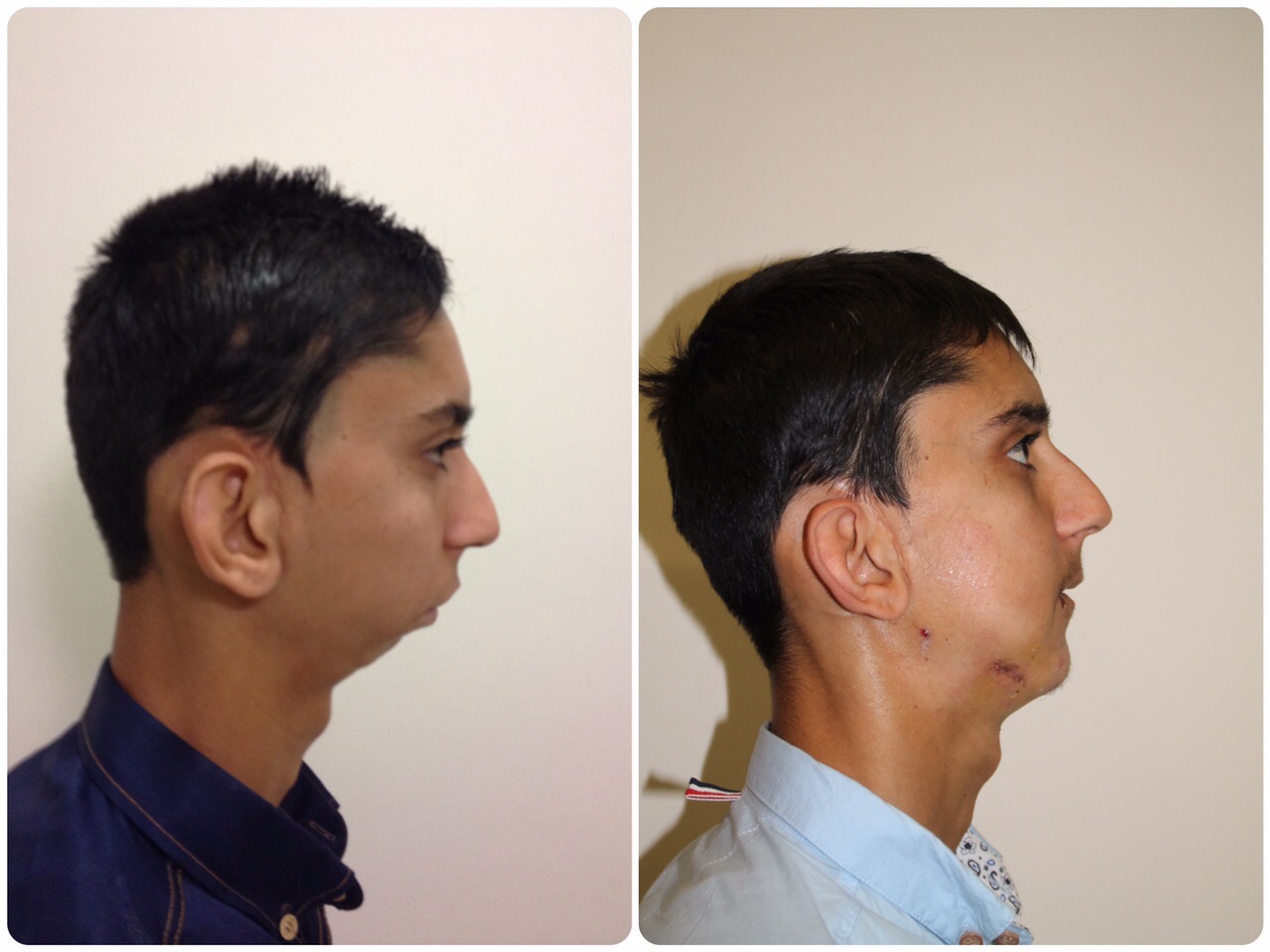
For all his life, 21-year-old Harman Abdullah had never tasted the delicacies like Yakhni pulao and Korma his mother cooked. This was not because he lived away from her, but because he could never open his mouth wider than a few millimeters to bite into them.
Abdullah (from Kabul) presented to Fortis Memorial Research Institute with Classical bird face deformity which restricted his mouth opening to barely 10 mm (against a normal 35-40 mm mouth opening).
Abdullah had a history of trauma to the temporo-madibular joint as a child (which fused his jaw into the skull and made it immobile), leading to progressive inability to open his mouth.
He had been operated twice as a child back home to improve his condition but not much to his avail. Abdullah also had a severely retruded chin as his bone had not grown as any other normal child affecting his physical appearance. As a result, Harman had not completed his schooling and had no peer. Due to his condition, he could not maintain proper oral hygiene and was malnourished and weak in his overall well-being.
During the two earlier surgeries – doctors had tried to separate the jaw from the skull but his condition only marginally improved.
A 3D CT scan showed fusion of the lower jaw bone to the skull, leading to the diagnosis of Bilateral Temporo- Mandibular joint ankylosis.
At Fortis Memorial Research Institute, his treatment, under Dr Gagan Sabharwal, Consultant, Maxillofacial Surgeon at was planned in two stages - improve mouth opening and improve esthetic.
The surgical phase was divided into 3 parts. In the first part Inter-positional arthroplasty where a wide bony gap is created at the jaw joint region, with interpose local flap, followed by aggressive mouth opening exercise and physiotherapy was carried out.
“Post this surgery, Harman was able to open his mouth to as wide as 35 mm much to his and his family’s disbelief. His mother wept,” recalled Dr Sabharwal.
The second stage was carried out 6 months after the first surgery. This was the distractor placement and distraction phase - where the bone was divided at the mandibular angle region and gradually moved apart 1cm a day using a mandibular distraction device.
“We achieved 20 mm of bone distraction by the end of a month,” explained Dr Sabarwal.
In the third and last stage which followed four months after the second surgery – called the consolidation phase- the distractor was removed and an advancement genioplasty was done to achieve results.
“The total treatment time took one-and-a-half years from start to end and the patient visited the hospital thrice with and average hospital stay period 4 days each time and 1months in India" said Dr Sabarwal
Harman has returned to India for a medical follow up and a much improved health and overall well-being.
Abdullah (from Kabul) presented to Fortis Memorial Research Institute with Classical bird face deformity which restricted his mouth opening to barely 10 mm (against a normal 35-40 mm mouth opening).
Abdullah had a history of trauma to the temporo-madibular joint as a child (which fused his jaw into the skull and made it immobile), leading to progressive inability to open his mouth.
He had been operated twice as a child back home to improve his condition but not much to his avail. Abdullah also had a severely retruded chin as his bone had not grown as any other normal child affecting his physical appearance. As a result, Harman had not completed his schooling and had no peer. Due to his condition, he could not maintain proper oral hygiene and was malnourished and weak in his overall well-being.
During the two earlier surgeries – doctors had tried to separate the jaw from the skull but his condition only marginally improved.
A 3D CT scan showed fusion of the lower jaw bone to the skull, leading to the diagnosis of Bilateral Temporo- Mandibular joint ankylosis.
At Fortis Memorial Research Institute, his treatment, under Dr Gagan Sabharwal, Consultant, Maxillofacial Surgeon at was planned in two stages - improve mouth opening and improve esthetic.
The surgical phase was divided into 3 parts. In the first part Inter-positional arthroplasty where a wide bony gap is created at the jaw joint region, with interpose local flap, followed by aggressive mouth opening exercise and physiotherapy was carried out.
“Post this surgery, Harman was able to open his mouth to as wide as 35 mm much to his and his family’s disbelief. His mother wept,” recalled Dr Sabharwal.
The second stage was carried out 6 months after the first surgery. This was the distractor placement and distraction phase - where the bone was divided at the mandibular angle region and gradually moved apart 1cm a day using a mandibular distraction device.
“We achieved 20 mm of bone distraction by the end of a month,” explained Dr Sabarwal.
In the third and last stage which followed four months after the second surgery – called the consolidation phase- the distractor was removed and an advancement genioplasty was done to achieve results.
“The total treatment time took one-and-a-half years from start to end and the patient visited the hospital thrice with and average hospital stay period 4 days each time and 1months in India" said Dr Sabarwal
Harman has returned to India for a medical follow up and a much improved health and overall well-being.
Meghna A Singhania is the founder and Editor-in-Chief at Medical Dialogues. An Economics graduate from Delhi University and a post graduate from London School of Economics and Political Science, her key research interest lies in health economics, and policy making in health and medical sector in the country. She is a member of the Association of Healthcare Journalists. She can be contacted at meghna@medicaldialogues.in. Contact no. 011-43720751
Next Story


