- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Hidden breast cancer after breast augmentation diagnosed by colour Doppler: BMJ case report
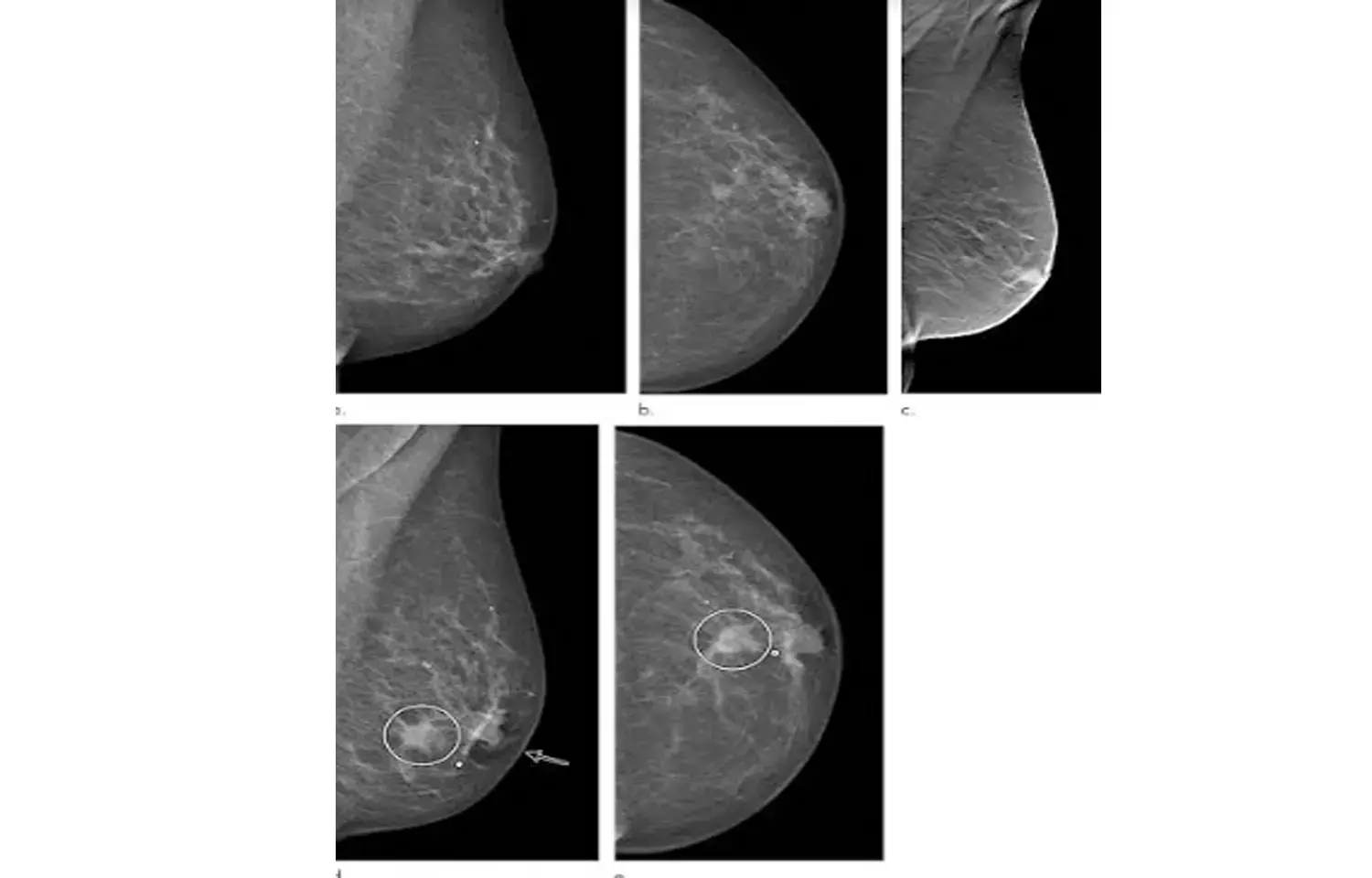
Breast augmentation with silicone injection is currently prohibited due to safety concerns. However, there are still a certain number of elderly people who underwent breast augmentation with silicone injection.
Some reports show that breast cancer arises after breast augmentation with silicone injection. Common screening methods, including palpation, mammography (MMG) and ultrasonography (US), are ineffective for detecting breast cancer due to the influence of silicone granulomas, which makes diagnosis challenging.
US findings for breast cancer with mass lesions are usually visualised as hypoechoic masses. The presence of hypervascular areas on colour Doppler ultrasound (CD) suggests malignant tumours.
In this case reported by Akihiro Fujimoto and team, a lesion showing 18F-fluorodeoxyglucose (FDG) uptake was incidentally identified by FDG-positron emission tomography/CT (PET/CT) after breast augmentation with silicone injection; however, the tumour was not palpable and US did not show any mass lesion. A slightly hypoechoic area showing hypervascularity was observed on CD; thus, core needle biopsy was performed and early stage breast cancer was diagnosed.
CASE PRESENTATION
The patient was an 83-year-old postmenopausal woman with a paternal family history of gastric cancer. The patient had a history of colon cancer and Hashimoto's disease. She underwent breast augmentation with silicone injection approximately 60 years ago and underwent surgery for colon cancer approximately 1 year ago.
A PET/CT was done to detect colon cancer recurrence. During this time, a lesion showing FDG uptake was incidentally detected in her right breast and was suspected to be breast cancer.
Diffuse undulations were palpated on both sides of the breast, which is consistent with the influence of breast augmentation with silicone injection; however, no apparent mass was palpated near the FDG uptake area. MMG was not performed considering breast augmentation surgery.
US did not show a clear hypoechoic mass lesion at the site corresponding to the FDG uptake site, but careful observation using CD revealed a slight hypoechoic area with hypervascularity.
An US-guided core needle biopsy was performed and invasive ductal carcinoma (IDC) was diagnosed based on the histological findings.
Immunohistochemical staining revealed positive expressions of oestrogen receptor and progesterone receptor. The human epidermal growth factor receptor-2 (HER-2) expression score was 2+, but in situ hybridisation showed no amplification of the HER2 gene. US also revealed multiple hypoechoic masses with no vascularity in her right breast, near the FDG uptake site based on PET/CT images.
Silicone granulomas were suspected; thus, additional core needle biopsies were performed on one of the mass lesions to rule out breast cancer. As expected, the diagnosis was silicone granuloma.
PET/CT revealed the absence of axillary metastasis and distant metastasis, and revealed the maximum lesion diameter to be 25mm. Thus, the diagnosis was classified as stage IIA IDC (cT2N0M0) based on the eighth edition of the Union for International Cancer Control tumour–node–metastasis classification of malignant tumours.
Right mastectomy and sentinel lymph node biopsy were performed. Postoperative pathological findings confirmed that the tumour was IDC with an infiltration diameter of 29mm. Therefore, the final diagnosis was stage IIA IDC (pT2N0M0). Macroscopic findings of the resected specimen revealed multiple silicone granulomas on the dorsal side of breast cancer mass.
Histological findings showed that extensive granulomas were present in the mammary tissue surrounding or within the tumour, consistent with postsilicone injection findings. No axillary lymph node metastases were observed, but macrophage aggregation was prominent; this may have been due to the silicone injection.
Outcome and Follow-up: Approximately 2 months had passed since the operation. The patient is currently undergoing adjuvant endocrine therapy with no apparent recurrence.
This case highlights two important clinical issues:
- First, in cases in which US does not show any mass after breast augmentation with silicone injection, CD should be used to detect hypervascularised areas.
- Second, to prevent false-negative biopsy results, it is important to perform CD to identify hypervascularisation that suggests cancer at suspected sites.
US usually shows breast cancer with mass lesions as hypoechoic masses. In this case, plain CT and macroscopic findings of the resected specimen revealed that the breast cancer had a usual mass lesion. Therefore, if it were not for the silicone injection, the lesion was more likely to be palpable and appear as a hypoechoic mass.
In contrast, the FDG uptake site on PET/CT, that is, the site where the lesion was considered to be present, was carefully checked using CD to identify hypervascularisation. The extent of vascularisation in and around lesions is helpful in distinguishing between benign and malignant tumours. Although in this case, the site of FDG uptake was a non-mass lesion, a slightly hypoechoic area compared with the surrounding area, suggesting that a biopsy was required.
Stereotactic-guided biopsy was reported to be useful for breast cancer diagnosis after breast augmentation with silicone injection when lesions are unidentifiable via US. It is common to not perform MMG after breast augmentation surgery due to quality control issues in screening for breast cancer and possible damage to the insertion. MMG findings are less likely to indicate mammographic abnormalities in the absence of any physical findings. In addition, contrast-enhanced MMG may also have been effective for assessing breast vascularity in this case.
Contrast-enhanced magnetic resonance imaging (MRI) may also be effective in detecting breast cancer after breast augmentation. However, even though the MRI findings strongly indicate the presence of cancer, a biopsy should be performed to confirm the diagnosis of cancer. Breast biopsy, most commonly performed under US guidance, is important to identify breast lesions on US.
In conclusion, CD should be actively used to detect hypervascularised areas to prevent false-negative biopsy results, especially when no lesions are detected on US. While CD was helpful in this case and is increasingly suggested as a relatively straightforward adjunct in complex and challenging cases, it may not be applicable to all cases; further research on its value is required.
Breast augmentation with silicone injections is no longer performed and only the elderly has undergone this method in the past, however similar problems are expected to arise in case of silicone breast implant (SBI) injury. SBI is widely used for breast augmentation and breast reconstruction.
In this case, breast cancer was incidentally found by PET/CT, but the lesion was initially non-palpable and asymptomatic, thus, making it difficult to detect breast cancer by US screening alone. Breast cancer screening using MMG may be required even after breast augmentation, but due care must be taken during the examination. Furthermore, PET/CT and MRI are not commonly used in screening for breast cancer, but these methods may be considered after breast augmentation, especially when lesions are not palpable or easily visible on US.
Source: Fujimoto A, Kosaka Y, Hasebe T, et al. BMJ Case Rep 2021;14:e242742.
doi:10.1136/bcr-2021- 242742
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


