- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Atypical Presentation of Juvenile Hyaline Fibromatosis of Hands- A report
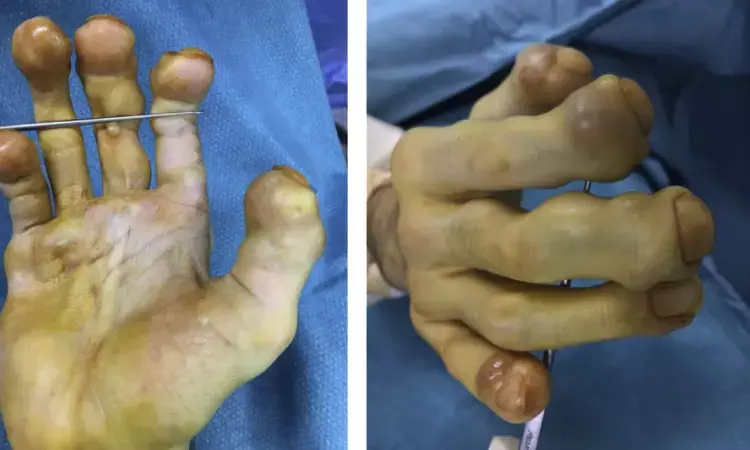
Juvenile hyaline fibromatosis is a rare disorder characterized by an extracellular accumulation of hyaline deposit. In the extremities, lesions may remain quiescent or gradually increase in size, eventually resulting in skin ulceration. There is no curative treatment. Surgery may allow some recovery of function, but recurrence is possible. Ruben Dukan et al report a case of juvenile hyaline fibromatosis in both hands of a 25-year-old man who required multiple surgical procedures to address problems with function, pain, and appearance.
According to history, the patient was a 25-year-old man, the first of 3 children, born of unrelated parents in France. He was right-handed and a non-smoker. There was no family history of fibrous disorders. Juvenile hyaline fibromatosis was diagnosed at age 4 years. He gradually lost the ability to walk because of bilateral knee deformity and clubfoot. At age 17 years, lower-limb corrective surgeries involving distal femoral extension osteotomy and percutaneous Achilles tenotomy were performed to improve ambulation.
The first skin lesions appeared on the face and back in childhood. Papular and nodular skin lesions, appeared progressively in the extremities, causing substantial aesthetic and functional disability. Evolution of the various skin lesion was variable, with some progressing more quickly than others. Difficulty fitting footwear and plantar pain required resection of the nodules from the feet at age 18 years. In the hands, multiple excisions were performed at ages 18, 22, and 23 years. At each procedure, careful dissection of the neurovascular structures was performed to assess their integrity and release them from compression.
Histologic examination of the excised specimen revealed JHF each time. The tumor was composed of abundant hyaline extracellular matrix embedding spindle or oval cells, which were isolated or organized in sheets. The density of the cells was heterogeneous, from scanty to moderate. No atypia, necrosis, or mitosis was observed. Successive radiographic assessment of the hands showed osteopenia and revealed both erosive and sclerotic lesions, predominantly at the distal interphalangeal joints.
At the last follow-up (2 years after the last procedure), there was no recurrence at the site of the previously resected nodules. The evolution of the other lesions and masses did not result in a loss of functional capacity, and thus did not require surgery. Despite the contractures of different hand joints related to JHF, the patient maintained functional grip and pinch capacity. He was able to continue work as a consultant. Juvenile hyaline fibromatosis had progressed in the lower extremities and the patient was confined to a wheelchair. Nevertheless, the satisfactory evolution of the hands allowed him to perform upper-limb muscular-strengthening activities, enabling him to maintain a social life and some ambulation.
Further reading:
Atypical Presentation of Juvenile Hyaline Fibromatosis of Hands.
Ruben Dukan, Gautier Petroni, Patrick Bruneval, Stephanie Pannier, Emmanuel H. Masmejean.
J Hand Surg Am. r Vol. 47, February 2022
https://doi.org/10.1016/j.jhsa.2020.12.013
MBBS, Dip. Ortho, DNB ortho, MNAMS
Dr Supreeth D R (MBBS, Dip. Ortho, DNB ortho, MNAMS) is a practicing orthopedician with interest in medical research and publishing articles. He completed MBBS from mysore medical college, dip ortho from Trivandrum medical college and sec. DNB from Manipal Hospital, Bengaluru. He has expirence of 7years in the field of orthopedics. He has presented scientific papers & posters in various state, national and international conferences. His interest in writing articles lead the way to join medical dialogues. He can be contacted at editorial@medicaldialogues.in.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


