- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
"Malignant hypertension unveiling as Bilateral exudative retinal detachment"- BMJ Case Report
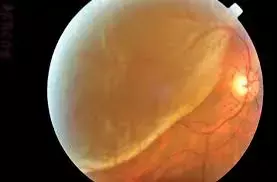
Acute massive elevation of blood pressure can cause hypertensive choroidopathy and exudative retinal detachment without underlying retinopathy changes.
Severe and acute elevation in BP can cause hypertensive choroidopathy as choroidal vessels are more prone to damage in such conditions. These vessels do not have a well-developed autoregulation mechanism, presence of adrenergic receptors and a short course with minimal branching. This causes downstream transmission of acute elevation in BP and causes fibrinoid necrosis of choroidal arterioles and occlusion of areas of choriocapillaris.
Dr. Anirudh Kapoor recently published a case study in BMJ case reports where a young patient presented with complaints of severe reduction in vision and headache of acute onset and was diagnosed to be a case of exudative retinal detachment with choroidopathy.
Presenting complaints-
24-year-old man presented with sudden-onset bilateral loss of vision with persistent headaches for 3 days. His visual acuity (VA) in the right eye was 20/1200 and in the left eye was finger counting close to face.
On examination-
Both pupils were equally reactive and anterior segment examination was normal bilaterally.
Dilated fundus evaluation revealed bilateral serous retinal detachment with macular involvement. Multiple white patches were noted lying deep to the retina in both eyes consistent with Elschnig spots.
His blood pressure (BP) was found to be 246/143mm Hg and he was referred to emergency medicine for further management.
A diagnosis of bilateral exudative retinal detachment with hypertensive choroidopathy in malignant hypertension was made.
The patient was admitted for management of hypertensive emergency. He was found to have acute renal failure requiring emergent dialysis. The aetiology of his renal failure was unclear at the time of discharge and he was started on outpatient intermittent haemodialysis. Three weeks after blood control was achieved, his VA improved to 20/80 and 20/63 in the right and left eye, respectively. The retinal detachments in both eyes resolved with few residual haemorrhages.
Differential diagnosis included Vogt-Koyanagi-Harada disease - young patient with complaints of headache and bilateral serous retinal detachments. Although, these patients also have accompanying signs of ocular inflammation involving the anterior and/or the posterior segment and often other integumentary and neurological signs and symptoms.
Also, cases of hypertensive choroidopathy due to choroidal ischaemia and associated exudative retinal detachment with minimal to no abnormalities in retinal circulation have been described in association with pre-eclampsia and eclampsia, renal failure, systemic lupus erythematosus, disseminated intravascular coagulation, thrombotic thrombocytopenic purpura and Castleman's disease.
"Most of the cases of acute hypertensive choroidopathy with serous retinal detachments resolve with control of BP. Hypertensive choroidopathy can present independent of retinopathy and this case demonstrates an extreme example of ocular manifestation of a life threatening hypertensive emergency."
Take home message-
- Patients with malignant hypertension may present first to an ophthalmologist with vision loss being their predominant complaint.
- Acute massive elevation of blood pressure can cause hypertensive choroidopathy and exudative retinal detachment without underlying retinopathy changes.
Source: Kapoor A, Kumar A, Chawla R. BMJ Case Rep 2021;14:e242413. doi:10.1136/bcr-2021- 242413
Dr Ishan Kataria has done his MBBS from Medical College Bijapur and MS in Ophthalmology from Dr Vasant Rao Pawar Medical College, Nasik. Post completing MD, he pursuid Anterior Segment Fellowship from Sankara Eye Hospital and worked as a competent phaco and anterior segment consultant surgeon in a trust hospital in Bathinda for 2 years.He is currently pursuing Fellowship in Vitreo-Retina at Dr Sohan Singh Eye hospital Amritsar and is actively involved in various research activities under the guidance of the faculty.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


