- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Rare case of Progressive Worsening of Unilateral Ptosis in Woman- A report
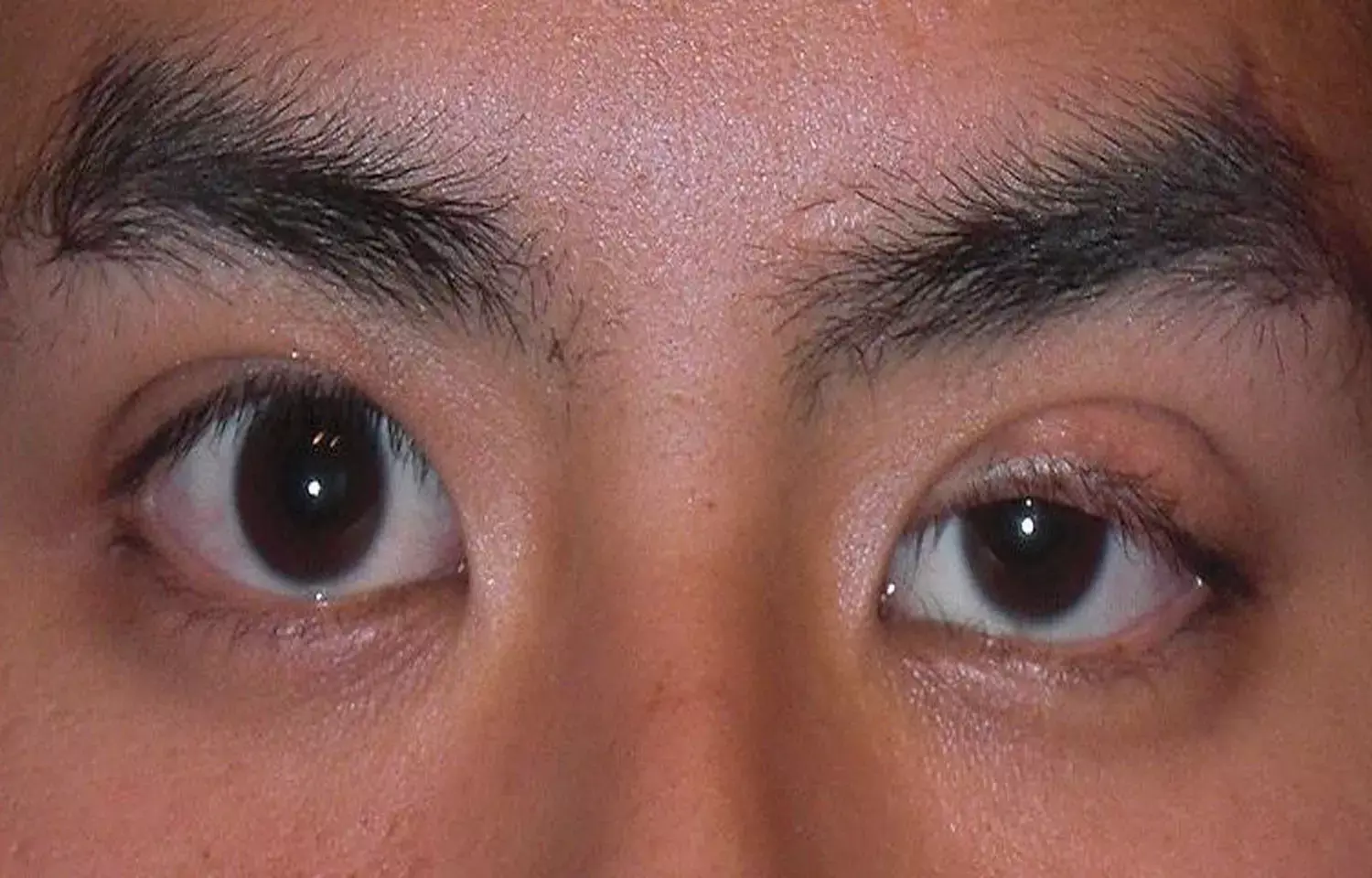
Researchers have reported a rare case of Progressive Worsening of Unilateral Ptosis in Woman and has been published in JAMA case reports.
According to history, a woman in her 60s with a history of hyperlipidemia, hypothyroidism, and chronic migraines presented with 9 months of progressively worsening left-sided ptosis, which was more notable at night and with fatigue. She denied experiencing pain, diplopia, muscle weakness, dysarthria, dysphagia, difficulty breathing, or other neurologic deficits.
On examination, corrected visual acuity was 20/20 bilaterally, with normal color vision, visual fields, intraocular pressure, extraocular movements, alignment, and pupils.
External examination was notable for left upper eyelid ptosis, with a margin-to reflex distance 1 of 3.5 mm on the right and 0.5 mm on the left, intact levator function, and no fatiguability on sustained upgaze. There was no evidence of eyelid edema, erythema, or tenderness to palpation. There were no palpable adnexal masses or orbital rim deformities, but there was mild fullness in the left superior sulcus and mildly increased left-sided resistance to retropulsion. However, Hertel exophthalmometry did not reveal any relative proptosis. No lacrimal gland abnormalities or conjunctival masses were seen with upper eyelid eversion. There was no palpable preauricular or cervical lymphadenopathy. Slit lamp and fundus examination findings were normal. Serological testing results for antiacetylcholine receptor antibody were negative.
The patient was diagnosed having Unilateral ptosis secondary to mantle cell lymphoma of the left lacrimal gland.
The etiologies for unilateral ptosis in adults include involutional, traumatic, myogenic (eg, muscular dystrophy), neurogenic (eg, myasthenia gravis), and mechanical (eg, eyelid or orbital mass). While the most common cause of ptosis in adults is involutional ptosis related to levator dehiscence, other diagnoses should be considered in patients with abnormal clinical findings in addition to ptosis.
Although ptosis that is more notable at night and with fatigue is classically seen with myasthenia gravis, patients with ptosis of other etiologies may report similar symptoms owing to reduced compensatory frontalis action by the end of the day. This patient did not have any neurologic signs or fatiguability on examination, and antiacetylcholine receptor serology findings were negative, making myasthenia gravis less likely. Similarly, the patient had normal levator function and extraocular motility, making myogenic ptosis less likely. However, unilateral findings of superior sulcus fullness and increased resistance to retropulsion were concerning for an orbital process. In this case, orbital imaging revealed a well-demarcated tumor involving the left lacrimal gland, with mass effect on the superior rectus-levator complex. Subsequent biopsy and workup demonstrated mantle cell lymphoma without systemic involvement.
Lacrimal gland tumors typically present with progressive proptosis and upper eyelid swelling over the course of 12 months or longer but can present with a shorter duration of symptoms, including ptosis. On magnetic resonance imaging, lacrimal gland lymphomas classically appear as well-defined masses that conform to the globe and adjacent orbital bones, are mildly hypointense to isointense on T1- and T2-weighted images, and enhance with contrast. Once a lacrimal gland biopsy confirms the diagnosis, systemic evaluation is performed for staging and treatment planning.
Mantle cell lymphoma is a rare form of non-Hodgkin lymphoma, representing 2% to 7% of ocular adnexal lymphomas, and is characterized by widespread disease on presentation, an aggressive clinical course, frequent recurrences, and poor survival. Current therapeutic options include radiation, chemotherapy, and immunotherapy but systemic therapy may be advantageous even in stage I and II disease because of high risk of relapse. Although the prognosis for most ocular adnexal lymphomas is generally good, with a 5-year diseases pecific survival of 81%, 5-year disease-specific survival for ocular adnexal mantle cell lymphomas can be as low as 38%. Regardless of the initial treatment response, all patients require long-term surveillance for disease recurrence. This case illustrates how lacrimal gland lymphomas can present as unilateral ptosis and underscores the importance of performing a thorough clinical examination (eg, palpation of periocular soft tissues and resistance to retropulsion) followed by an appropriate workup, which can lead to early detection and treatment of potentially life-threatening conditions.
Patient Outcome: This patient received 24 Gy of radiation to the left lacrimal gland for localized disease. Three months after treatment, repeated magnetic resonance imaging showed significant reduction in left lacrimal gland size. Positron emission tomography at 6months posttreatment showed resolution of tracer uptake in the left lacrimal gland.
Source: Jane S. Kim, MD; Jonathan D. Trobe, MD; Shannon S. Joseph, MD, MSc; JAMA Ophthalmology Clinical Challenge
doi:10.1001/jamaophthalmol.2021.5716
Dr Ishan Kataria has done his MBBS from Medical College Bijapur and MS in Ophthalmology from Dr Vasant Rao Pawar Medical College, Nasik. Post completing MD, he pursuid Anterior Segment Fellowship from Sankara Eye Hospital and worked as a competent phaco and anterior segment consultant surgeon in a trust hospital in Bathinda for 2 years.He is currently pursuing Fellowship in Vitreo-Retina at Dr Sohan Singh Eye hospital Amritsar and is actively involved in various research activities under the guidance of the faculty.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


