- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Rare case of Stargardt Juvenile Macular Degeneration reported in NEJM
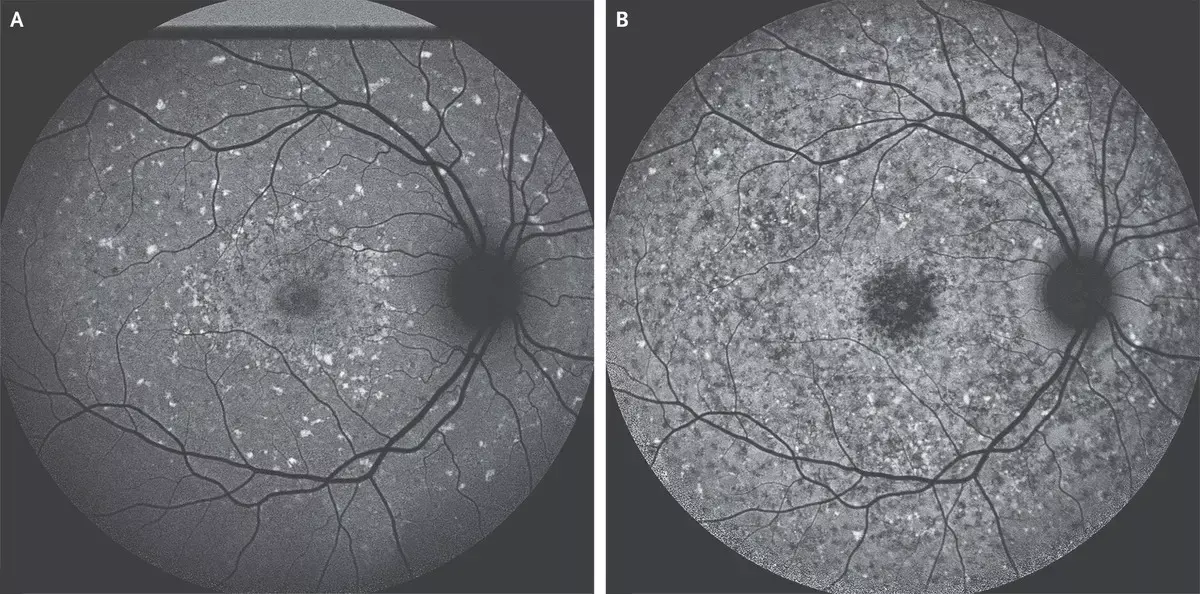 Courtesy New England journal of Medicine
Courtesy New England journal of MedicineDr Stephen H. Tsang and colleagues at Columbia University Irving Medical Center, New York have reported a rare case of Stargardt Juvenile Macular Degeneration that has been published in the New England journal of Medicine.
Juvenile Macular Degeneration refers collectively to a group of rare and inherited eye diseases that affect the vision of children and young adults. Juvenile Macular Degeneration primarily targets the vision of children, teens and young adults.
Stargardt's disease, Best Disease and Juvenile Retinoschisis are the major eye diseases constituting juvenile macular degeneration. AMD and JMD not only seem synonymous, they work the same way as well, i.e. AMD affects the macula in adults, while JMD affects the macula in children, teens and young adults.
Juvenile macular degeneration is an inherited genetic disorder and different types of the disease have different inheritance patterns.
According to the history a 13-year-old boy was referred to the ophthalmology clinic with enlarging blind spots in the central vision in both eyes. He had no family history of eye problems. At presentation, the visual acuity was 20/40 in the right eye and 20/50 in the left eye. Fundus examination of both eyes showed widespread, yellow, pisciform flecks. Short-wavelength autofluorescence imaging showed diffuse hyperautofluorescent lesions suggestive of bisretinoid accumulation and patchy central areas of atrophy of the retinal pigment epithelium with peripapillary sparing (Panel A). These findings are consistent with a diagnosis of Stargardt juvenile macular degeneration (also called Stargardt's disease), an autosomal recessive disorder caused by mutations in the gene encoding ATP-binding cassette subfamily A member 4 (ABCA4). Dysfunction of the ABCA4 transporter leads to the accumulation of toxic bisretinoids with consequent degeneration of the retinal pigment epithelium and photoreceptors. Vision loss typically begins during childhood and progresses. The diagnosis was confirmed with sequencing of ABCA4. The patient was advised to avoid vitamin A supplementation, which may accelerate bisretinoid accumulation. At 6-year follow-up, visual acuity was 20/70 in the right eye and 20/50 in the left eye, with worsening central scotomata. Autofluorescence imaging showed progressive atrophy in the previously identified areas of pisciform flecks with the maintenance of peripapillary sparing (Panel B)
For further reference log on to:
N Engl J Med 2020; 382:2353
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


