- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Children with T2D have a higher risk of developing retinopathy than those with T1D: JAMA
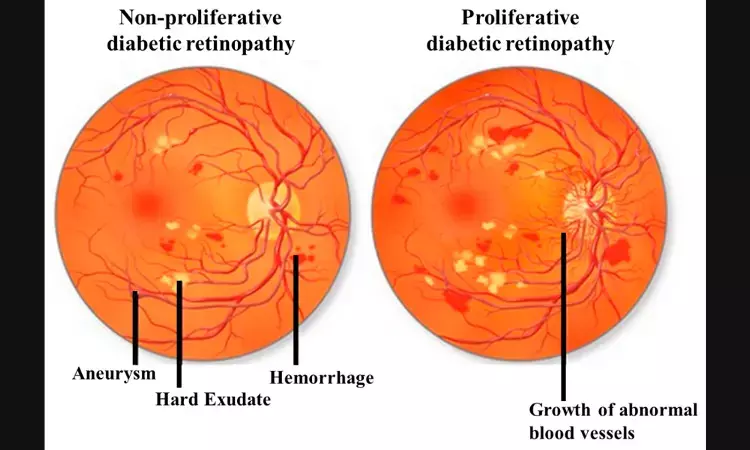
Diabetes is a common chronic disease of childhood characterized by chronic hyperglycemia with end-organ damage that often results in the microvascular triad of nephropathy, neuropathy, and retinopathy.
Although the ocular sequelae of type 1 diabetes (T1D) and adult onset type 2 diabetes (T2D) have been well described, little is known concerning the progression of diabetic retinopathy among children with T2D, despite its increasing prevalence in recent year.
Children with T2D have a higher risk of developing retinopathy than those with T1D, finds a new study.The study has appeared in JAMA ophthalmology.
The purpose of this study carried by Patricia Bai et al was to assess the risk of developing diabetes-associated ocular complications (DAOC) among a population-based cohort of children diagnosed with either T1D or T2D during a 50-year period.
This retrospective, population-based medical record review included all residents of Olmsted County, Minnesota, diagnosed with diabetes at younger than 22 years from January 1, 1970, through December 31, 2019. Main outcomes and measures included Risk of developing ocular complications over time.
Among 1362 individuals with a diagnostic code of diabetes, medical record reviews confirmed a diagnosis of T1D or T2D in 606 children, of whom 525 (86.6%) underwent at least 1 eye examination.
Diabetes-associated ocular complications occurred in 147 of the 461 children (31.2%) with T1D and in 17 of the 64 children (26.6%) with T2D. The hazard ratio illustrating the risk between T2D and T1D rates was 1.88 (P = .02) for developing any diabetic retinopathy (nonproliferative or greater), 2.33 (P = .048) for proliferative diabetic retinopathy, 1.49 (P = .50) for diabetic macular edema, 2.43 (P = .24) for a visually significant cataract, and 4.06 (P = .007) for requiring pars plana vitrectomy by 15 years after the diagnosis of diabetes.
In this 50-year population-based cohort, children diagnosed with T2D had a higher risk of developing diabetic retinopathy, developing PDR, and requiring PPV compared with those diagnosed with T1D. The duration between the diagnosis of diabetes and the development of diabetic retinopathy was shorter in the T2D cohort compared with the T1D cohort, and patients with T2D developed vision-threatening retinopathy at a higher rate than those with T1D. This suggests that the natural history of retinopathy development among youth diagnosed with T2D may differ from that in youth diagnosed with T1D, where patients with T2D may be more susceptible to developing retinopathy than those with T1D despite controlling for diabetes disease duration
In this population-based cohort of children diagnosed with diabetes during a 50-year period, patients with T2D developed vision-threatening retinopathy after a shorter diabetes duration and at a higher rate than children with T1D. These findings suggest that to prevent serious ocular complications, children with T2D may require ophthalmoscopic evaluations at least as frequently as or more frequently than children with T1D.
doi:10.1001/jamaophthalmol.2021.5052
Dr Ishan Kataria has done his MBBS from Medical College Bijapur and MS in Ophthalmology from Dr Vasant Rao Pawar Medical College, Nasik. Post completing MD, he pursuid Anterior Segment Fellowship from Sankara Eye Hospital and worked as a competent phaco and anterior segment consultant surgeon in a trust hospital in Bathinda for 2 years.He is currently pursuing Fellowship in Vitreo-Retina at Dr Sohan Singh Eye hospital Amritsar and is actively involved in various research activities under the guidance of the faculty.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


