- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Rare Case of Congenital Smooth Muscle Hamartoma Obscuring the Cornea reported
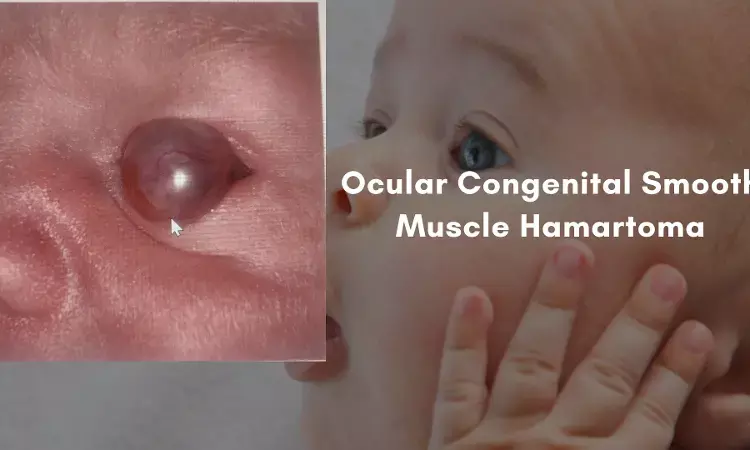
A congenital epibulbar mass raises suspicion for a variety of conditions ranging from benign to life-threatening. High on the differential is a limbal dermoid, which typically presents as a well-circumscribed yellow-white solid mass involving the conjunctiva, limbus, or cornea.
A more rare condition with similar presentation is congenital anterior staphyloma, consisting of an opaque corneal protrusion lined with uveal tissue. Histopathologic evaluation is often helpful in establishing the true etiology of these lesions.
Congenital smooth muscle hamartoma is a benign proliferation of smooth muscle that predominately occurs as a single lesion in the lumbosacral area and proximal extremities. These lesions are sporadic and occur in 1 in 2600 live births, with a slight male predominance.
Ocular involvement of congenital smooth muscle hamartoma, though exceedingly rare, has been reported in the eyelid, brow, and conjunctival fornix. The authors Andrew Bean and team are first to describe a patient with a congenital smooth muscle hamartoma in the bulbar conjunctival/limbal region published Hindawi Case Reports in Ophthalmological Medicine.
Case Report
A newborn male was seen in the hospital for a cyst on his left eye. The cyst had been visualized by prenatal ultrasound at 28 weeks of gestation.
The patient was born at 38 weeks and 2 days. There were no complications with delivery; vacuum assist or forceps were not required.
On ophthalmic examination:
The cyst was translucent and vascularized. It was 9 mm in size and protruded from the globe. It was attached to the limbus nasally and temporally and to the sclera inferiorly.
Magnetic resonance imaging of the brain and orbits with and without contrast reported a unilocular cyst arising from the left globe. No other abnormal findings were noted. The lesion was thought to be an atypical dermoid cyst. Erythromycin ointment was prescribed, and a close follow-up was arranged.
The cyst was noted to have regressed somewhat at the patient's two-month clinic visit, with less protrusion from the globe than initial presentation. It appeared as a firmly attached, pink infratemporal mass.
Some peripheral cornea was visible, but the pupil was occluded completely. Little if any potential for useful vision was possible with the lesion in place. After discussion with the patient's parents, the decision was made to proceed with excision of the cyst and cornea graft placement.
The cyst wall was incised superiorly, and dissection was carried inferiorly. The wall of the cyst was completely excised from the underlying deformity and sent for pathology. Removal of the cyst resulted in an evident defect in the cornea, with uvea protruding through. Once dissection of the trephination extended to the inferior temporal area, the iris had to be caught and peeled off the back of the adherent cornea. The lens did not appear to be involved and was retained.
The donor cornea was transferred into place and sutured with interrupted 10-0 nylon sutures. The patient tolerated the procedure well. On postoperative day 1, the graft was in good position and the closure was intact.
However, the graft had become diffusely cloudy by two months postoperatively and by 3 months had developed peripheral vascularization. The patient did not seem to have any pain or distress with his left eye.
Given the extensive nature of the original lesion and involvement of three fourths of the limbus, a repeat graft was thought to have a high likelihood of failure.
Pathologic evaluation of the specimen revealed conjunctival mucosa with benign smooth muscle proliferation, consistent with smooth muscle hamartoma.
Hematoxylin and Eosin staining revealed haphazardly arranged fascicles of smooth muscle with characteristic elongated, spindleshaped to blunt-ended nuclei.
Smooth muscle actin stain was diffusely positive. The lesion lacked dense fibrous tissue or dermal elements characteristic of dermoid.
Congenital smooth muscle hamartomas of the periorbita are thought to arise from the vascular smooth muscle or from the smooth muscle in the eyelid retractor complexes. Though rare, there are several cases of congenital smooth muscle hamartomas of ocular structures described in the literature.
To the knowledge of authors, this was the first reported case of a congenital smooth muscle hamartoma originating in the bulbar conjunctival/limbal tissue. It is possible that the patient's congenital smooth muscle hamartoma arose from the smooth muscle cells the limbal vascular endothelium. Congenital smooth muscle hamartoma should be added to the differential in a patient presenting with a cystic corneal or perilimbal lesion.
Source: Hindawi Case Reports in Ophthalmological Medicine Volume 2021
https://doi.org/10.1155/2021/6692229
Dr Ishan Kataria has done his MBBS from Medical College Bijapur and MS in Ophthalmology from Dr Vasant Rao Pawar Medical College, Nasik. Post completing MD, he pursuid Anterior Segment Fellowship from Sankara Eye Hospital and worked as a competent phaco and anterior segment consultant surgeon in a trust hospital in Bathinda for 2 years.He is currently pursuing Fellowship in Vitreo-Retina at Dr Sohan Singh Eye hospital Amritsar and is actively involved in various research activities under the guidance of the faculty.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


