- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
First case of COVID-19 presenting as Gullian- Barre syndrome
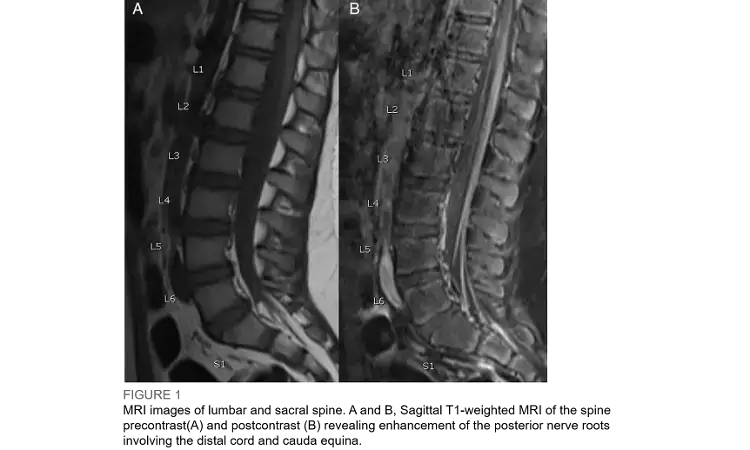
Guillain-Barré syndrome (GBS)is typically a postinfectious autoimmune process characterized by a monophasic, ascending, and symmetrical paralysis with areflexia that progresses over days to weeks. In the latest issue of Journal of AAP, Dr Molly Cutis et al illustrate an interesting first ever case of COVID-19 presenting as GBS in children.
The patient presented to emergency department with history of back pain and progressive weakness since past week. Illness started as bilateral lower extremity weakness that progressed to paralysis and inability to walk for which he was evaluated at local emergency department and reassured to be normal after X-ray of lumbar spine.
Over the next few days, his weakness worsened as he began to develop upper extremity weakness and dyspnea, hence he was referred to a tertiary care centre.
At the time of admission to pediatric floor, the patient was afebrile with blood pressure of 139/97 mmHg, heart rate of 135 beats per minute, respiratory rate of 35 breaths per minute, and oxygen saturation of 95% on room air. He was dyspneic, only able to speak 2 to 3 words at a time.
Cranial nerves were intact except for intermittent left esotropia and dysconjugate gaze. Overall muscle strength was diminished with 3/5 in the upper extremities and 2/5 in the lower extremities. Deep tendon reflexes were absent in upper and lower extremities bilaterally. Sensation was intact to light touch, but proprioception of the distal lower extremities was abnormal.
Baseline negative inspiratory force was 60 mmHg. He denied any recent illness within past 2 months including fever, cough, upper respiratory tract infection, diarrhea and emesis.
The patient rapidly developed increased secretions with poor clearance and cough, requiring intubation. An MRI of the spine revealed abnormal enhancement of the posterior nerve roots from the T11 level through the cauda equina and CSF analysis showed albuminocytologic dissociation. Results for the Gram-stain, culture, and rapid meningitis-encephalitis multiplex panel were negative. Electro diagnostic testing revealed prolonged distal latencies and low amplitude responses in the upper and lower extremities. These findings were compatible with a sensorimotor demyelinating polyneuropathy.
The result of the patient's SARS-CoV- 2 nucleic acid amplification was positive on 2 separate samples on hospital days 1 and 5. SARS-CoV-2 immunoglobulin G antibody was detected in his serum. Hence a diagnosis of BBS, AIDP form as a presentation of COVID-19 infection was confirmed.
Further workup was notable for elevated CRP, IL-6, D-dimer and neutrophilia with leukocytosis, however the patient did not meet CDC criteria for MIS-C.
Treatment was initiated with intravenous immunoglobulin (IVIg) - 2 g/kg IVIg over 48 hours. His examination revealed improvement over the next several days after IVIg with 4+/5 upper extremity strength and 3/5 lower extremities bilaterally. The patient was extubated on hospital day 5 following which intensive physical,
occupational, and speech therapy were initiated. Serial testing for SARS-CoV2 was negative at the time of discharge.
With this case, the authors illustrate the ever widening scope of presentations of
COVID-19 and associated complications. Clinicians need to constantly have a high level of suspicion for COVID-19 in all patients admitted to the hospital, especially in patients with unexplained symptoms.
Authors conclude-"Children with an unexplained neurologic process should be tested for SARS-CoV-2."
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


