- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Rare case of cerebral infarction in Congenital Adrenal Hyperplasia: A report
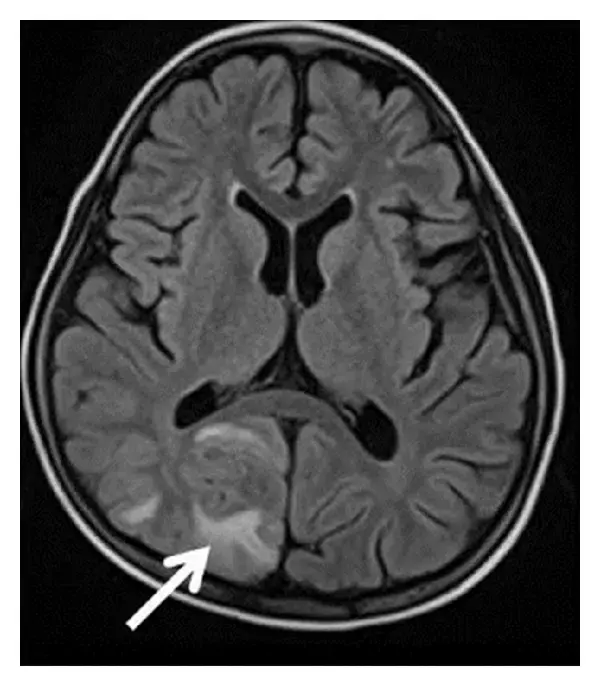
Dr Saugata Acharyya et al from Calcutta Medical Research Institute report a rare case of extensive cerebral infarction in a child with diagnosed Congenital Adrenal Hyperplasia.
A 5‑year‑old boy born out of non-consaguinity presented to the emergency room with acute onset fever (36 h), altered sensorium, and new‑onset refractory generalized tonic‑clonic seizures. His past history was notable for congenital adrenal hyperplasia(CAH) diagnosed on day 10 of life as child presented with significant weight loss and shock with supportive investigations of 21-hydroxylase deficiency. He was put on a regular maintenance dose of glucocorticoid (15 mg/m2/day) and mineralocorticoid (0.1 mg) supplementation since then. Growth and immunization was appropriate till date. He did not have any other major illness and blood pressure recodrings were always normal.
At the time of admission child was febrile(temperature-101) with a recurring seizure and recorded hypoglycemia(RBS-38mg/dl).He was given two doses of IV midazolam and a bolus of fosphenytoin for seizure termination and 10% dextrose bolus for hypoglycemia. Fundus examination showed no signs of rased ICT and neurological examination revealed a GCS of 7/15 ,extensor plantars with brisk deep‑tendon jerks in the lower limbs, and the pupils were sluggishly reacting bilaterally. He was started on supportive therapy-IV fluids and IV antibiotics(Ceftriaxone,vancomycin and acyclovir) with a maintenance dose of IV fosphenytoin and levetiracetam. ABG was suggestive of metabolic acidosis and with a poor GCS he was put on mechanical ventilator.
Rotine blood tests were suggestive of anemia with normal total count and platelets. LFT ,RFT,serum electrolytes and serum CRP levels were all normal. Malaria parasites and dual antigen, Dengue NS1 and IgM, blood and urine culture, as well as scrub typhus and Mycoplasma IgM, were all negative. The serum aldosterone level was 16 ng/dl (normal <40) and the ratio of serum aldosterone and plasma renin activity was normal (<20). The early morning serum cortisol level was 18 μg/dl (normal 3–20).Initial CT scan of the brain revealed multiple acute hematoma in the right cerebral hemisphere along with sulcal bleed and extensive infarction in the right cerebral hemisphere and left frontal region. CSF analysis was within normal limits with negative virological screening.The EEG was suggestive of diffuse encephalopathy and echocardiography was normal.
Child improved with above measures with no further seizures and ventilation was weaned off on day 5 , phenytoin was tapered and levetiracetam was continued. The sensorium was improved gradually, but there was mild residual weakness of the left side, for which regular physiotherapy was advised. A magnetic resonance imaging (MRI) of the brain performed on day 7 revealed large subacute infarcts along with multiple hematomas in right cerebral hemisphere.
The results of investigations to delineate any underlying cause of cerebral infarction were all normal(protein C,protein S, antithrombin 3, homocysteine levels, Serum C3 & C4,pANCA, antinuclear and antiphospholipid antibodies).MR angiogram and Doppler of carotid vessels were normal. The child was discharged on day 14 after putting him back to his normal maintenance doses of glucocorticoids and mineralocorticoids.
From previous evidence it has been suggested that CAH in itself or its treatment with glucocorticoid and/or mineralocorticoid or an inadequate treatment under stressful conditions may be the cause of cerebral infarction. This may be related to the potential inhibitory role of cortisol in the process of neuronal maturation and myelination by inhibiting the differentiation of oligodendrocyte precursors.
Authors conclude-"inadequate dose‑escalation along with the possible cerebral effect of CAH itself might be responsible for the cause of cerebral infarction in this child, which had led to the acute neurologic emergency".
Source: Acharyya, Saugata, et al. "Cerebral infarction in a child with congenital adrenal hyperplasia presenting as acute encephalitis syndrome." Journal of Pediatric Critical Care, vol. 8.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


