- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
CT/Ultrasound Fusion, a novel sampling technique of ovarian biopsy
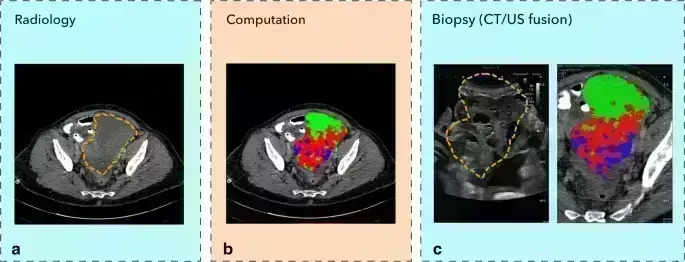
Improving patient stratification is a major challenge in high-grade serous ovarian cancer (HGSOC) where both genomic and tumour microenvironment heterogeneity is found within and between patients. High genomic heterogeneity is associated with reduced progression-free survival. In a recent study, researchers have developed a novel precision tissue sampling technique that co-registers CT-based radiomics–based tumour habitats with Ultrasound (US) images in the clinical routine for patients with HGSOC. The research has been published in the journal European Radiology on December 14, 2020.
MRI or CT/US fusion biopsies are an emerging technique to selectively target areas of interest. MRI/US fusion biopsies improve the accuracy to detect especially clinically significant prostate cancer while decreasing the detection of low-grade cancers. MRI or CT/US fusion systems are increasingly used to target hepatic lesions as they increase the accuracy to target tumours that are undetectable with US alone. So far no studies have applied imaging-guided US fusion biopsies in patients with HGSOC. Therefore researchers of the Cancer Research UK Cambridge Centre, University of Cambridge, conducted a study to develop a precision tissue sampling technique that uses computed tomography (CT)–based radiomic tumour habitats for ultrasound (US)-guided targeted biopsies that can be integrated with the clinical workflow of patients with high-grade serous ovarian cancer (HGSOC).
It was a prospective study in Six patients with suspected HGSOC scheduled for US-guided biopsy before starting neoadjuvant chemotherapy from September 2019 to February 2020. Researchers performed the tumour segmentation manually on the pre-biopsy contrast-enhanced CT scan. They used spatial radiomic maps to identify tumour areas with similar or distinct radiomic patterns, and tumour habitats were identified using the Gaussian mixture modelling. CT images with superimposed tumour habitat maps were then co-registered with ultrasound data using Smart Fusion software. They used the dice similarity coefficient (DSC) to assess the tumour-specific CT/US fusion accuracy.
A gynecological radiologist utilized the fused images to perform an ultrasound-guided biopsy on all six participants using an ultrasound scanner with a 3.5-MHz convex transducer. Up to six biopsies -- two per tumour habitat -- were collected for each patient, according to the researchers. They noted that the median time between CT scan and biopsy was 21 days (range 7–30 days) and the median DSC for tumour-specific CT/US fusion accuracy was 0.53. They found that CT/US fusion accuracy was high for the larger pelvic tumours (DSC: 0.76–0.79) while it was lower for the smaller omental metastases.
The authors concluded, "We developed a precision tissue sampling technique that uses radiomic habitats to guide in vivo biopsies using CT/US fusion and that can be seamlessly integrated in the clinical routine for patients with HGSOC".
For further information:
Medical Dialogues Bureau consists of a team of passionate medical/scientific writers, led by doctors and healthcare researchers. Our team efforts to bring you updated and timely news about the important happenings of the medical and healthcare sector. Our editorial team can be reached at editorial@medicaldialogues.in.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


