- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Rare case of calcification around catheter tip of a central venous access port: a report
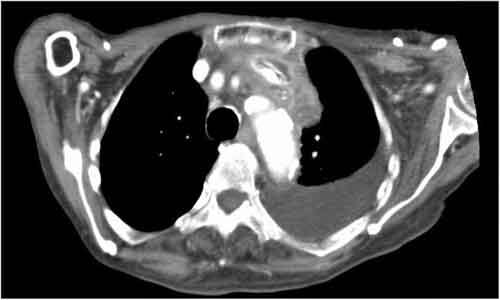
Dr Tomoya Takami at the Department of General Surgery, Cardiology, Kishiwada Tokushukai Hospital, Kishiwada-shi, Osaka-fu, Japan and colleagues have reported a rare case of calcification around catheter tip of a central venous access port. The case has been published in the Journal of Medical Case Reports.
Thrombosis of the internal jugular vein is a relatively rare form of deep vein thrombosis, but this condition has been reported in association with the long-term placement of a central venous catheter (CVC). However, it is extremely rare for such complications to involve calcification in the blood vessels.
The etiology of intravascular calcification is considered to be related to the infusion content and the infusion rate of high caloric infusions and blood products.
The patient an 84-year-old Asian woman presented with persistent anorexia since being treated for acute myocardial infarction about 1 year prior to the current presentation. Her anorexia was thought to be related to aging. Because it was difficult to secure a peripheral venous infusion route, a CVC was placed about 5 months before the current presentation to ensure the provision of adequate nutrition. After CVC placement, the patient's condition remained stable, but she developed a persistent fever. Infection around the CVC was suspected, so she was referred to our hospital. Her medical history included hypertension and dementia. Her regular medications were antiplatelet drugs, proton pump inhibitors, laxatives, and diuretics.
On physical examination, the patient had a temperature of 37 °C, blood pressure of 142/91 mmHg, heart rate of 93 beats/minute, and respiratory rate of 18 breaths/minute. No redness or warmth was noted around the CVC port. Blood tests revealed a marked inflammatory response. The patient's white blood cell count was 16,600/μl, C-reactive protein concentration was 9.42 mg/dl, hemoglobin concentration was 11.2 g/dl, platelet count was 139,000/μl, blood urea nitrogen concentration was 23 mg/dl, and creatinine concentration was 0.69 mg/dl. Chest computed tomography (CT) showed a CVC port located subcutaneously in the left anterior chest, but there were no signs of infection such as a subcutaneous abscess around the port or increased fat deposition. The catheter tip was located within the lumen of the left brachiocephalic vein, but there was a high absorption area around it with some air density; thus, venous wall calcification and abscess formation were suspected. Chest CT showed bilateral pleural effusion that was worse on the left. Based on the blood test and CT findings, the diagnosis was abscess formation with venous wall calcification following long-term CVC placement.
The patient was hospitalized and started on antibiotics (cefmetazole 1 g every 8 hours). Bacterial culture of a blood sample collected on the day of hospitalization revealed multidrug-resistant Serratia marcescens, so the antibiotic was changed to meropenem (1 g every 8 hours) for a total of 15 days. The patient's clinical course was uneventful, her fever subsided, and the inflammatory response improved. Chest CT performed 20 days after hospital admission showed that the abscess cavity had shrunk and that there was no infection recurrence. The patient was subsequently followed up at our hospital for about 1 month.
In general, cases of catheter-associated infection warrant early removal of the catheter. However, in the present case, the catheter tip was fixed to the calcified venous wall, and forcible removal would have damaged the catheter and left parts of it in the blood vessel. Therefore, surgical removal was recommended, but the family declined surgery because of the patient's advanced age, so only antibiotic treatment was administered. Although the patient's family was advised that the infection could recur around the CVC, they elected to avoid surgical CVC removal for the same reason.
For further reference log on to: https://doi.org/10.1186/s13256-019-2333-z
Hina Zahid Joined Medical Dialogue in 2017 with a passion to work as a Reporter. She coordinates with various national and international journals and association and covers all the stories related to Medical guidelines, Medical Journals, rare medical surgeries as well as all the updates in the medical field. Email: editorial@medicaldialogues.in. Contact no. 011-43720751
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


