- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Brazilian Guidelines for Early Mobilization in Intensive Care Unit
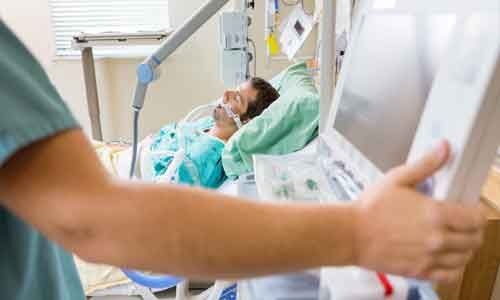
Associação Médica Brasileira has released Brazilian guidance on early mobilisation in the Intensive Care Unit. The objective of this guideline was to produce a document that would provide evidence-based recommendations and suggestions regarding the early mobilization of critically ill adult patients, with the aim of improving understanding of the topic and making a positive impact on patient care.
In the last decade, there has been an increase in evidence regarding the functional benefit of early physical therapy for critically ill patients starting in the first 48 hours after the institution of mechanical ventilation (MV); however, patient mobilization as a usual practice is still infrequent. Immobility can cause several complications, including skeletal muscle atrophy and weakness, that influence the recovery of critically ill patients. This effect can be mitigated by early mobilization. Early mobilization is safe and should be the goal of the entire multidisciplinary team.
Following are the major recommendations:
- Early mobilization is safe. Adverse events are mainly related to hemodynamic and/or respiratory changes, are low-frequency and are reversible with the interruption of the intervention. Adverse events are not frequent or severe, and early mobilization is considered safe (A).
- Early mobilization is indicated for adults in the ICU, preferably those under spontaneous breathing, who cooperate and who do not have intracranial hypertension (A). Mechanical ventilation and noncooperation may be considered limitations for early mobilizations, but not contraindications.
- Early mobilization is contraindicated for terminal patients with systolic hypertension (systolic blood pressure > 170mmHg) or intracranial hypertension, unstable fractures, recent acute myocardial infarction and open abdominal wounds (A).
- The appropriate dose of early mobilization is defined by clinical efficacy and individual tolerance (B).
The doses are as follows:
- Passive mobilization: approximately 10 to 20 mobilizations per selected joint, up to two times/day.
- Active exercises: 1 hour per day, up to two 30-minute sessions.
The following constitute positioning and progression:
- Assisted verticalization with an orthostatic board: up to 1 hour per day, up to twice a day.
- Passive ergometer cycling: 20 minutes, 20 cycles/minute.
- Active ergometer cycling: two 10-minute sessions per day (A).
- The care and safety criteria for early mobilization do not require specific monitoring, and hemodynamic and respiratory stability characterize a safe intervention model (A).
- The prognostic indicators include an assessment of the risk of functional decline, weight, functional range, muscle strength, hemodynamic instability, respiratory dysfunction, recent extubation, protective factors, sedation, length of stay in the ICU and duration of mechanical ventilation (B).
For more details click on the link: doi: 10.5935/0103-507X.20190084
Hina Zahid Joined Medical Dialogue in 2017 with a passion to work as a Reporter. She coordinates with various national and international journals and association and covers all the stories related to Medical guidelines, Medical Journals, rare medical surgeries as well as all the updates in the medical field. Email: editorial@medicaldialogues.in. Contact no. 011-43720751
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


