- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Prone Position Improves Oxygenation In Non intubated ICU Patients of COVID-19
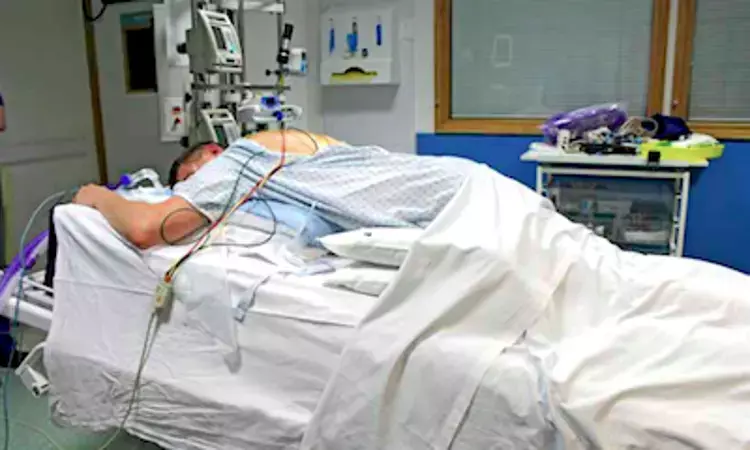
New information, recommendations and treatment guidelines are emerging often for the management of COVID 19. In the treatment for severe acute respiratory distress syndrome (ARDS) from coronavirus disease 2019 (COVID-19), the World Health Organization (WHO) recommends prone positioning (PP) during mechanical ventilation for periods of 12–16 h/d to potentially improve oxygenation and survival. In a recent study published in the ANESTHESIA & ANALGESIA, researchers have found supporting evidence for this recommendation. They reported prone positioning improved oxygenation in all patients with COVID 19 and moderate or severe ARDS.
Since the emergence of the novel severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection in December 2019, the coronavirus disease 2019 (COVID-19) has rapidly spread across the globe. The clinical spectrum of patients with COVID-19 ranges from asymptomatic or mild symptoms to critical disease with a high risk of mortality. In particular, the incidence of acute respiratory distress syndrome (ARDS) in patients hospitalized with COVID-19 can range from 17% to 30% who may later develop respiratory failure. Based on the WHO's recommendation on Prone position researchers of Clinical University Hospital of Santiago, Spain conducted a study to evaluate the effectiveness of the PP sessions to improve oxygenation and assess the incidence of tracheal intubation and mechanical ventilation in patients with moderate or severe ARDS by COVID-19.
It was a prospective observational study in seven awake patients with moderate or severe ARDS by COVID-19 admitted to the ICU at University Hospital of Santiago from March 21 to April 5, 2020. All patients received at least 1 PP session and were advised to remain in PP as long as possible until the patient felt too tired to maintain that position. A total of 16 PP sessions were performed in the 7 patients during the period study. They administered light sedation with dexmedetomidine and evaluated the following information: number and duration of PP sessions; tissue O2 saturation (Sto2) and blood gases before, during, and following a PP session; the need of mechanical ventilation; duration of ICU admission; and ICU outcome.
Key findings of the study were:
♦The median duration of PP sessions was 10 hours.
♦Researchers found that Oxygenation was increased in all 16 sessions performed in the 7 patients.
♦They also found that the ratio of arterial oxygen partial pressure to fractional inspired oxygen (Pao2/Fio2) significantly increased during PP (change from baseline 110) without significant changes after PP in the supine position.
♦They also observed small improvement in tissue oxygenation during PP (change from baseline 2.6%) without significant changes after PP.
♦They reported that two patients required intubation and all patients had well-tolerated PP sessions and discharged from ICU.
The authors concluded, "We found that PP improved oxygenation in ICU patients with COVID-19 and moderate or severe ARDS. PP was relatively well tolerated in our patients and maybe a simple strategy to improve oxygenation trying to reduce the number of patients in mechanical ventilation and the length of stay in the ICU, especially in COVID-19 pandemic".
For further information:
Medical Dialogues Bureau consists of a team of passionate medical/scientific writers, led by doctors and healthcare researchers. Our team efforts to bring you updated and timely news about the important happenings of the medical and healthcare sector. Our editorial team can be reached at editorial@medicaldialogues.in.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


