- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Stress worsens prognosis of non-surgical treatment of chronic periodontitis: Study
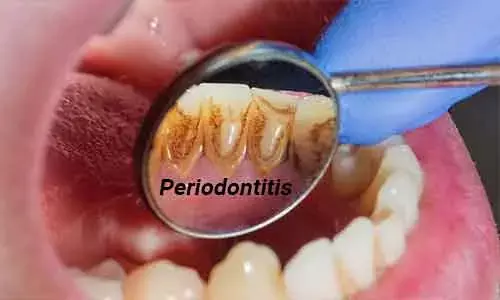
Recent research published in the Journal of Periodontology has found out that patients with increased stress, anxiety, and depression scores as well as those exhibiting negative coping strategies demonstrate worsened non‐surgical periodontal treatment (SRP) outcomes in severe chronic periodontitis cases.
Catherine Petit and colleagues from the Department of Periodontology, University of Strasbourg, Dental Faculty, Strasbourg, France conducted the study to evaluate the influence of psychological stress on non‐surgical periodontal treatment (SRP) outcomes in patients with severe chronic periodontitis (stage 3/4 generalized periodontitis) at 6 months in the French population.
Patients diagnosed with severe generalized chronic periodontitis (periodontitis stage 3/4) were included in this study. At baseline, psychological status was evaluated by self‐administered questionnaire (Depression Anxiety Stress Scale 42 [DASS‐42] and Toulouse coping scale [TCS]). Plasma levels of cortisol and chromogranin‐A were determined. Patients were then managed by oral hygiene instructions, scaling and root planing of sites with PD >3 mm and followed at 3 and 6 months. Quantitative and qualitative variables were described and interactions were determined by linear and logistic regressions.
The following results were seen-
a. Seventy‐one patients were included in this study and 54 were followed up to 6 months.
b. An average probing depth (PD) reduction of 0.73 ± 0.11 mm and decrease of diseased sites (PD >3 mm) were measured at 6 months illustrating SRP efficacy.
c. Multivariable analysis showed that increased DASS‐stress score was associated to worsened SRP outcomes in terms of bleeding on probing (BOP) (OR = 1.02, P <0.05) and mean PD (P <0.05) reduction.
d. An increase of DASS‐depression score negatively influenced PD >5 mm (OR = 1.06, P
7 mm (OR = 1.17, P
5 mm (OR = 1.03, P
7 mm (OR = 1.07, P <0.05) reduction.
e. Negative coping strategies were also associated with worsened SRP outcomes.
Hence, the authors concluded that "Patients with increased stress, anxiety, and depression scores as well as those exhibiting negative coping strategies demonstrate worsened SRP outcomes. DASS‐42 and TCS were useful to determine psychological status and their use could be incorporated to assess treatment prognosis."
Dr. Nandita Mohan is a practicing pediatric dentist with more than 5 years of clinical work experience. Along with this, she is equally interested in keeping herself up to date about the latest developments in the field of medicine and dentistry which is the driving force for her to be in association with Medical Dialogues. She also has her name attached with many publications; both national and international. She has pursued her BDS from Rajiv Gandhi University of Health Sciences, Bangalore and later went to enter her dream specialty (MDS) in the Department of Pedodontics and Preventive Dentistry from Pt. B.D. Sharma University of Health Sciences. Through all the years of experience, her core interest in learning something new has never stopped. She can be contacted at editorial@medicaldialogues.in. Contact no. 011-43720751
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


