- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
COVID-19 Linked to Deadly Relapsing Toxic Epidermal Necrolysis: A Case Report
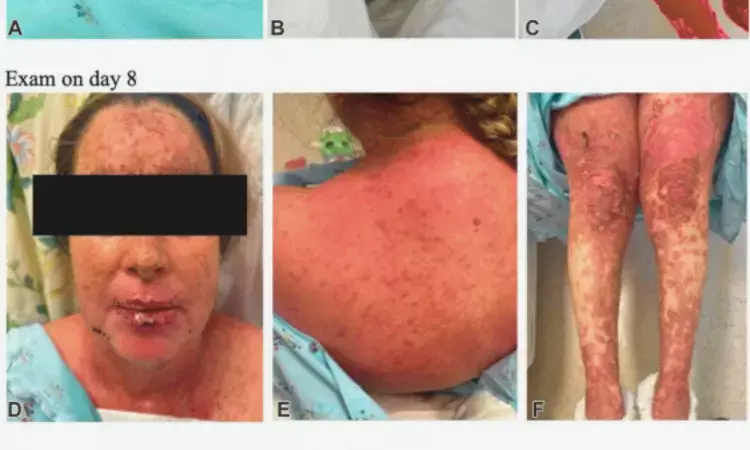
USA: A recent case report published in JAAD Case Reports has highlighted a concerning association between COVID-19 and the incidence of Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN), two severe dermatologic conditions typically triggered by medications. These conditions can lead to life-threatening skin reactions characterized by widespread erythema, painful blisters, and extensive skin peeling.
Kenneth G. Linden, Department of Dermatology, University of California, Irvine, Irvine, California, and colleagues present a complex case of refractory and relapsing TEN, with no identifiable causative medication, believed to be linked to immune sequelae following COVID-19.
COVID-19 has been linked to an increased incidence of Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN), with a reported sevenfold rise during the pandemic. While the exact mechanisms remain unclear, possible pathways include vaccine-induced reactions, virus-induced immune dysregulation, and increased drug hypersensitivity.
In the patient described in the case report, prior vaccination was unlikely the cause, but recent COVID-19 could have led to immune dysregulation and TEN. Notably, drugs like Paxlovid (nirmatrelvir/ritonavir) may contribute to hypersensitivity. Despite various treatments, including IVIG and cyclosporine, the patient’s condition worsened, ultimately resulting in her passing, suggesting COVID-19 might have triggered relapsing TEN.
The case concerns a 48-year-old woman with a history of unicentric Castleman disease, treated six months prior with rituximab, siltuximab, and radiation, and presented with a worsening pruritic rash covering approximately 20% of her body. Four weeks earlier, she had contracted COVID-19 and completed a 5-day course of nirmatrelvir/ritonavir (Paxlovid) three weeks before her hospital visit. On examination, a positive Nikolsky sign was noted, and two biopsies confirmed necrotic keratinocytes, indicating early-stage SJS or toxic epidermal necrolysis.
Her severity-of-illness score indicated a high mortality risk (>90%). The patient was treated with intravenous immunoglobulin (IVIG) and cyclosporine. However, by day three, her condition worsened, showing progression of the rash and oral erosions. A shave biopsy confirmed TEN.
Despite starting prednisone and topical corticosteroids, the patient continued to deteriorate. A second round of IVIG and cyclosporine was initiated, resulting in significant improvement, and she was discharged after 21 days.
However, six days post-discharge, she returned to the emergency department with severe skin pain and sloughing. Extensive testing, including various antibody panels, returned negative results, and a repeat biopsy again indicated TEN.
The patient underwent further rounds of IVIG and cyclosporine but failed to improve. Ultimately, she required intubation due to acute hypoxemic respiratory failure. Tragically, despite intensive care efforts, she passed away a month into her second hospitalization.
"Our case underscores the serious immunocutaneous complications that can arise from COVID-19, highlighting the urgent need for further research to elucidate the disease's pathophysiology and pave the way for more targeted treatment options," the researchers concluded.
Reference:
Messele F, Horton L, Sharma AN, Min MS, Rojek NW, Linden KG. Relapsing toxic epidermal necrolysis following COVID-19. JAAD Case Rep. 2024 Jul 31;53:23-26. doi: 10.1016/j.jdcr.2024.07.011. PMID: 39430626; PMCID: PMC11488411.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


