- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Dermoscopy of primary cutaneous amyloidosis: A retrospective analysis
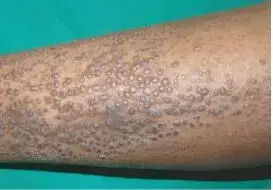
Source- Behera B, Kumari R, Mohan Thappa D, Gochhait D, Hanuman Srinivas B, Ayyanar P. Dermoscopic features of primary cutaneous amyloidosis in skin of colour: A retrospective analysis of 48 patients from South India. Australas J Dermatol. 2021 Jul 6. doi: 10.1111/ajd.13662. Epub ahead of print. PMID: 34227687.
Dermoscopy of primary cutaneous amyloidosis : AJD study
Primary cutaneous amyloidosis (PCA) are a group of benign dermatoses characterized extracellular deposition of amyloid fibrils locally in the skin. It has 3 classical clinical variants papular amyloidosis (PA) or lichen amyloidosis (LA), macular amyloidosis (MA) and the rare nodular amyloidosis. These are very pruritic and diagnosis is usually clinical. They can be confused for various dermatoses like LA for lichen simplex chronicus, prurigo nodularis etc and MA can mimic lichen planus pigmentosus, pigmented contact dermatitis etc. Dermoscopy has recently been used for its diagnosis but literature on its features in skin of colour are sparse. A study describing dermoscopic features of PCA was published recently in the Australasian Journal of Dermatology.
This was a retrospective study conducted from April 2014 to December 2016 at a tertiary care hospital of South India including all the biopsy-proven PCA cases. Dermoscopic pictures were taken using a HEINE DELTA20 dermatoscope attached to a Nikon SLR camera under nonpolarised contact mode. A total of 48 patients (26 females and 22 males) 30 patients with LA and 18 with MA, all belonging to the skin phototypes IV and V were included. Pruritus (66.7%) was the most frequent complaint followed by cosmetic concerns (47.9%).
A two zone pattern comprising a central structureless white area of variable shade and a peripheral ridge and groove area and/ or structureless pigmented area, was the most common dermoscopic pattern observed in LA (83.3%). The colour of the structureless white area varied from brownish-white, grey-white to blue-grey-white.
In MA, a jigsaw puzzle pattern, comprising pigment dots, globules, and/ or peppering arranged parallelly with or surrounded by structureless white area, was the dominant dermoscopic pattern (94.5%). The colour of the pigment dots, globules and peppering ranged from black, brown, brown-grey, grey and blue-grey. Two different hubs and spoke patterns were observed. One had a central white clod surrounded by pigment structures; the second had central brown dots, globules or peppering surrounded by grey to blue-grey radial structures (18.7%).
Pigment dots, globules or peppering were noted in all the cases and were arranged in the following configurations: clustered, discrete, starburst or radial, and corymbose. Around 20% of cases had a preferential perieccrine distribution of brown dots and peppering.
Pathologically, PCA is characterised by amyloid in the papillary dermis, increased epidermal pigmentation and pigment incontinence and marked epidermal changes like hyperkeratosis, hypergranulosis and acanthosis in LA. The white structureless area corresponds to the hyperkeratosis and/ or acanthosis. Acanthosis with increased epidermal melanin and/ or dermal pigment incontinence are responsible for the brownish-white, grey-white to blue-grey-white colour. Melanin in the stratum corneum corresponds to black dots, globules and peppering based on their concentration and aggregation. In both LA and MA, the ridge and groove area corresponds to the acanthotic and papillomatous epidermis and intervening epidermal invagination. The white hub in the spoke and wheel pattern corresponds to the eccrine duct opening.
The differences in dermoscopic features between LA and MA are due to their differences in epidermal growth patterns. In MA, the relative absence of hyperkeratosis and acanthosis results in predominance of pigment structures in various arrangements.
In conclusion this is a study of dermoscopic features of PCA in skin of colour and describes new dermoscopic patterns and features associated with primary cutaneous amyloidosis (PCA) which dermatologists should be aware of to differentiate PCA from its mimics.
Source-
Behera B, Kumari R, Mohan Thappa D, Gochhait D, Hanuman Srinivas B, Ayyanar P. Dermoscopic features of primary cutaneous amyloidosis in skin of colour: A retrospective analysis of 48 patients from South India. Australas J Dermatol. 2021 Jul 6. doi: 10.1111/ajd.13662. Epub ahead of print. PMID: 34227687.
MBBS
Dr Manoj Kumar Nayak has completed his M.B.B.S. from the prestigious institute Bangalore medical college and research institute, Bengaluru. He completed his M.D. Dermatology from AIIMS Rishikesh. He is actively involved in the field of dermatology with special interests in vitiligo, immunobullous disorders, psoriasis and procedural dermatology. His continued interest in academics and recent developments serves as an inspiration to work with medical dialogues.He can be contacted at editorial@medicaldialogues.in.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


