- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Maniere's disease - AAO-HNSF practice Guidelines
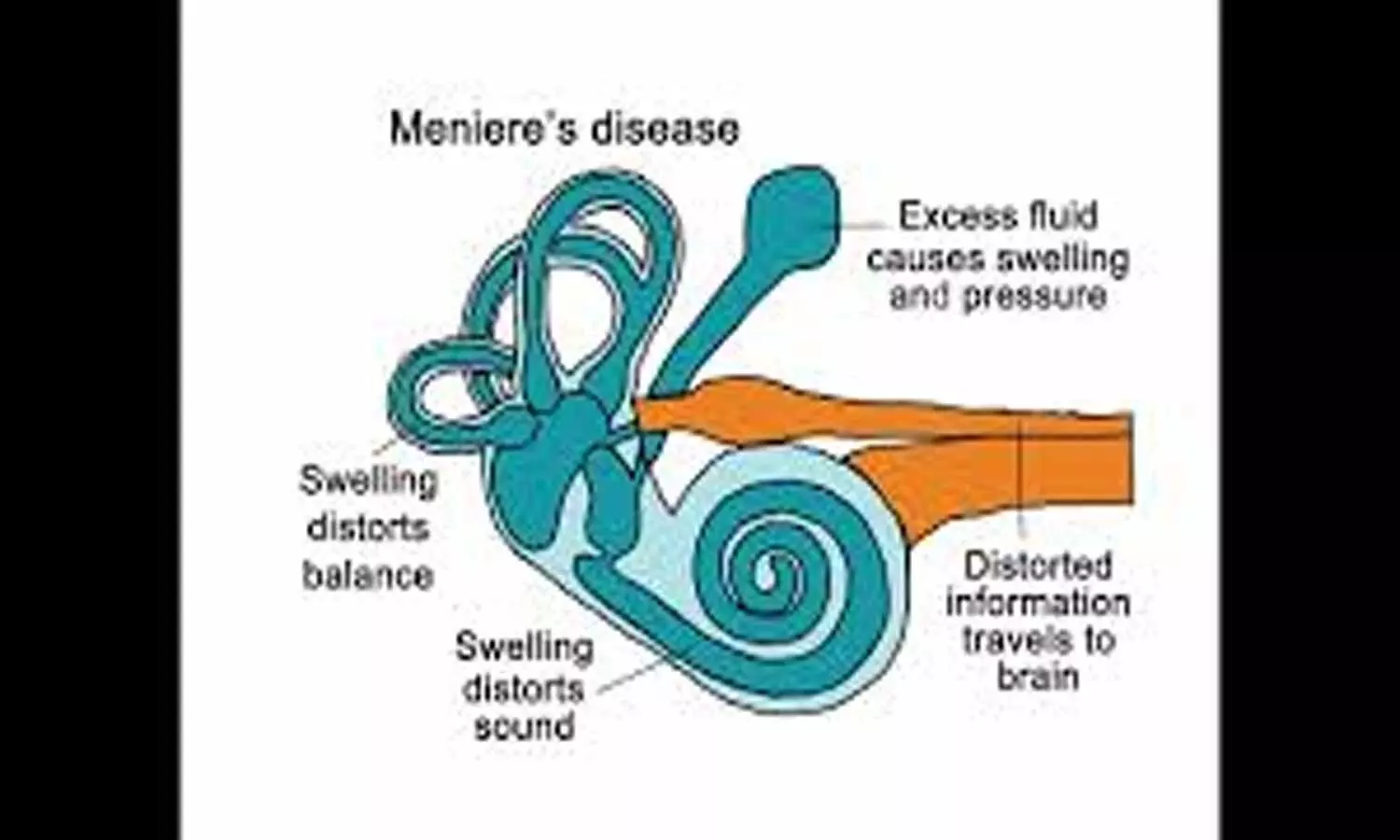
The American Academy of Otolaryngology-Head and Neck Surgery Foundation has released the Clinical Practice Guideline: Ménière's Disease . The guidelines have been published in Otolaryngology-Head and Neck Surgery.
Ménière's disease is a disorder of the inner ear that includes episodes of vertigo with possible hearing loss, ringing or buzzing in the ear, or ear pressure.
Ménière's disease is defined by spontaneous vertigo attacks, each lasting 20 minutes to 12 hours, with low- to mid-frequency sensorineural hearing loss in the affected ear before, during, or after one of the episodes of vertigo.
The clinical practice guideline (CPG) defines vertigo as the feeling of spinning or moving when one is not moving. This is different from dizziness, which can mean feeling lightheaded or feeling like passing out.
The guideline discusses the background on possible causes of Ménière's disease, disorders that present similarly to it, and the ways in which the disease can progress. "The guideline aims to reduce the subjectivity of diagnosis and treatment for Ménière's disease and to provide some objective standards based on the literature available today," said Dr. Basura. "This new CPG gives providers some optimal tools with which to make their clinical decisions."
Key recommendations are-
STATEMENT 1. DIAGNOSIS OF MENIÈRE'S DISEASE: Clinicians should diagnose definite or probable Ménière's disease in patients presenting with 2 or more episodes of vertigo lasting 20 minutes to 12 hours (definite) or up to 24 hours (probable) and fluctuating or nonfluctuating sensorineural hearing loss, tinnitus, or pressure in the affected ear, when these symptoms are not better accounted for by another disorder.
STATEMENT 2. ASSESSING FOR VESTIBULAR MIGRAINE: Clinicians should determine if patients meet diagnostic criteria for vestibular migraine when assessing for Ménière's disease.
STATEMENT 3. AUDIOMETRIC TESTING: Clinicians should obtain an audiogram when assessing a patient for the diagnosis of Ménière's disease.
STATEMENT 4. UTILITY OF IMAGING: Clinicians may offer magnetic resonance imaging (MRI) of the internal auditory canal and posterior fossa in patients with possible Ménière's disease and audiometrically verified asymmetric sensorineural hearing loss.
STATEMENT 5. VESTIBULAR OR ELECTROPHYSIOLOGIC TESTING: Clinicians should not routinely order vestibular function testing or electrocochleography to establish the diagnosis of Ménière's disease.
STATEMENT 6. PATIENT EDUCATION: Clinicians should educate patients with Ménière's disease about the natural history, measures for symptom control, treatment options, and outcomes.
STATEMENT 7. SYMPTOMATIC MANAGEMENT OF VERTIGO: Clinicians should offer a limited course of vestibular suppressants to patients with Ménière's disease for management of vertigo only during Ménière's disease attacks.
STATEMENT 8. SYMPTOM REDUCTION AND PREVENTION: Clinicians should educate patients with Ménière's disease on dietary and lifestyle modifications that may reduce or prevent symptoms.
STATEMENT 9. ORAL PHARMACOTHERAPY FOR MAINTENANCE: Clinicians may offer diuretics and/or betahistine for maintenance therapy to reduce symptoms or prevent Ménière's disease attacks.
STATEMENT 10. POSITIVE PRESSURE THERAPY: Clinicians should not prescribe positive pressure therapy to patients with Ménière's disease.
STATEMENT 11. INTRATYMPANIC STEROID THERAPY: Clinicians may offer, or refer to a clinician who can offer, intratympanic steroids to patients with active Ménière's disease not responsive to noninvasive treatment.
STATEMENT 12. INTRATYMPANIC GENTAMICIN THERAPY: Clinicians should offer, or refer to a clinician who can offer, intratympanic gentamicin to patients with active Ménière's disease not responsive to nonablative therapy.
STATEMENT 13. SURGICAL ABLATIVE THERAPY: Clinicians may offer, or refer to a clinician who may offer, labyrinthectomy in patients with active Ménière's disease who have failed less definitive therapy and have nonusable hearing.
STATEMENT 14a. ROLE OF VESTIBULAR THERAPY FOR CHRONIC IMBALANCE: Interictal instability and following ablative therapy: Clinicians should offer vestibular rehabilitation/physical therapy for Ménière's disease patients with chronic imbalance.
STATEMENT 14b. ROLE OF VESTIBULAR THERAPY FOR ACUTE VERTIGO: Clinicians should not recommend vestibular rehabilitation/physical therapy for managing acute vertigo attacks in patients with Ménière's disease.
STATEMENT 15. COUNSELING FOR AMPLIFICATION AND HEARING ASSISTIVE TECHNOLOGY: Clinicians should counsel patients, or refer to a clinician who can counsel patients, with Ménière's disease and hearing loss on the use of amplification and hearing assistive technology.
STATEMENT 16. PATIENT OUTCOMES: Clinicians should document resolution, improvement, or worsening of vertigo, tinnitus, and hearing loss and any change in quality of life in patients with Ménière's disease after treatment.
The CPG is intended for all healthcare providers in any setting who are likely to encounter, diagnose, treat, and/or monitor patients with suspected Ménière's disease. This includes emergency medicine, primary care, otolaryngology, neurology, audiology, and physical/vestibular therapy. The target patient for the guideline is anyone 18 years of age or older who has a suspected diagnosis of definite or probable Ménière's disease.
For further reference log on to:
https://doi.org/10.1177/0194599820909439
fluctuating aural symptoms, electrocochleography, endolymphatic hydrops, endolymphatic sac decompression, gentamicin, labyrinthectomy, Meniett device, sensorineural hearing loss, sodium-restricted diet, vestibular testing, quality of life
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


