- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Myomectomy yields superior health-related quality of life to uterine artery embolization: FEMME trial
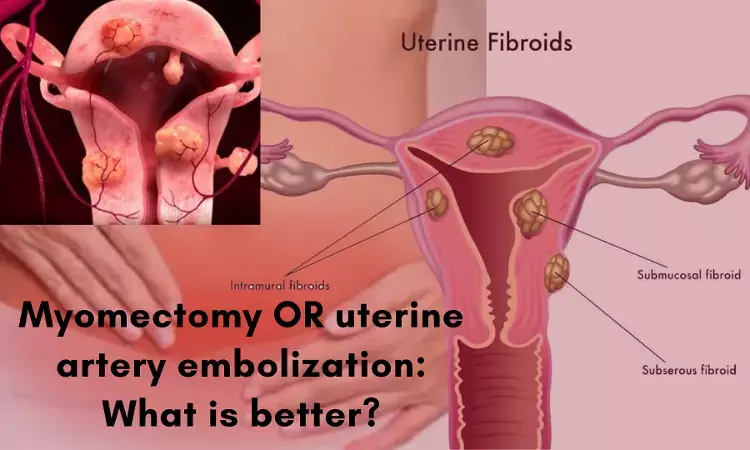
The prevalence of uterine fibroids, the most common type of tumor among women of reproductive age, increases with age. Approximately half of women with fibroids have bothersome symptoms, including heavy menstrual bleeding, abdominal pain, and pressure, that negatively affect quality of life. Submucosal fibroids and, to a lesser extent, intramural fibroids have been associated with subfertility and adverse pregnancy outcomes although data are inconsistent.
Surgery, either myomectomy or hysterectomy, has traditionally been the primary approach for the management of symptomatic fibroids; uterine artery embolization emerged as an alternative during the 1990s.
Myomectomy involves the surgical removal of the fibroid and preservation of the uterus. Although myomectomy substantially reduces heavy bleeding, it is associated with myometrial trauma, and whether it results in improved reproductive outcomes is not known.
Uterine-artery embolization, which is usually performed while the patient is under local anesthesia, involves temporary occlusion of the arteries supplying the uterus, with the use of biocompatible particles, to cause ischemic infarction of the fibroids.
As compared with myomectomy, uterine-artery embolization is associated with a shorter hospital stay and an earlier return to normal activities but also a higher likelihood of the need for additional intervention.
I. Manyonda et al conducted the FEMME trial (A Randomized Trial of Treating Fibroids with Either Embolisation or Myomectomy to Measure the Effect on Quality of Life Among Women Wishing to Avoid Hysterectomy), a multicenter, randomized trial to evaluate myomectomy, as compared with uterine-artery embolization, in women who had symptomatic uterine fibroids and did not want to undergo hysterectomy.
Procedural options included open abdominal, laparoscopic, or hysteroscopic myomectomy. The primary outcome was fibroid-related quality of life, as assessed by the score on the health related quality-of-life domain of the Uterine Fibroid Symptom and Quality of Life (UFS-QOL) questionnaire (scores range from 0 to 100, with higher scores indicating a better quality of life) at 2 years; adjustment was made for the baseline score.
The participants were recruited at 29 hospitals in the United Kingdom. Women were eligible for enrollment in the trial if they were older than 18 years of age, were premenopausal, were not pregnant, and had symptomatic fibroids that could be treated with myomectomy or uterine-artery embolization. Women were excluded if they had substantial adenomyosis, had a suspected or diagnosed cancer, had recent or ongoing pelvic inflammatory disease, or had undergone a previous open abdominal myomectomy or uterine-artery embolization.
Prespecified quality-of-life secondary outcomes were the following: the score on the health-related quality-of-life domain of the UFS-QOL questionnaire at 6 months and at 1 year, the score on the symptom severity domain of the UFS-QOL questionnaire (scores range from 0 to 100, with higher scores indicating increased severity), the score on the European Quality of Life 5-Dimension 3-Level (EQ-5D-3L) questionnaire (scores range from −0.59 to 1.00, with higher scores indicating a better quality of life), and the score on the EQ-5D visual analogue scale (scores range from 0 [indicating the worst possible health state] to 100 [indicating the best possible health state]).
Women estimated menstrual blood loss (the number of sanitary napkins or tampons used and the extent of soiling with blood) with the use of the pictorial blood-loss assessment chart and recorded their estimates in diary entries. Scores were then generated from the diary entries, with 0 as the lowest score (indicating no bleeding) and higher scores (no defined upper limit) indicating more bleeding.
Other secondary outcomes were the occurrence of pregnancy, a pregnancy outcome (live birth, miscarriage, stillbirth, or termination), participant satisfaction (determined on the basis of responses to "would you have your operation again?" and "would you recommend the operation to a friend?"), the length of hospital stay, and the occurrence of additional fibroid-related procedures.
Each participant-completed outcome assessment was collected at 6 months, 1 year, and 2 years after randomization. Ovarian reserve was determined on the basis of blood levels of follicle-stimulating hormone (FSH), antimüllerian hormone, and luteinizing hormone measured before myomectomy or uterine-artery embolization was performed and at 6 weeks, 6 months, and 1 year after the procedure.
A total of 254 women, recruited at 29 hospitals in the United Kingdom, were randomly assigned: 127 to the myomectomy group (of whom 105 underwent myomectomy) and 127 to the uterine-artery embolization group (of whom 98 underwent embolization).
In the intention-to-treat analysis, the mean (±SD) score on the health-related quality-of-life domain of the UFS-QOL questionnaire at 2 years was 84.6±21.5 in the myomectomy group and 80.0±22.0 in the uterine-artery embolization group (P=0.01).
The mean score on the health-related quality-of life domain was also higher after myomectomy than after uterine-artery embolization at both 6 months and 1 year.
The mean differences in the UFS-QOL symptom severity domain were −6.1 points favoring myomectomy at 6 months and −3.8 favoring myomectomy at 2 years, whereas menstrual bleeding scores appeared similar in the two groups.
At 2 years, the percentage of women who indicated that they would recommend a given procedure to a friend was 93% in the myomectomy group, as compared with 84% in the uterine artery embolization group, whereas the percentages of women who indicated that they would be willing to undergo the procedure again were 78% and 74%, respectively.
In total, 9 women (8%) in the uterine-artery embolization group and 5 women (4%) in the myomectomy group reported a pregnancy within 2 years after randomization; there were 6 live births in the uterine-artery embolization group and 4 live births in the myomectomy group. The hormonal levels did not appear to be materially different in the two groups at the majority of time points.
The incidence of intraoperative complications was low, with only one conversion of a myomectomy to a hysterectomy and one conversion of a laparoscopic myomectomy to an open abdominal myomectomy.
Although improvement in participant-reported health-related quality-of-life scores was observed after both myomectomy and uterine-artery embolization at 2 years, the scores indicated a higher health-related quality of life among women assigned to undergo myomectomy. Menstrual bleeding scores appeared similar in the two groups.
The overall incidence of complications associated with both procedures was low. Additional procedures were performed in 7% of the women in the myomectomy group, as compared with 16% in the uterine-artery embolization group; the median length of hospital stay was 4 days with myomectomy and 2 days with uterine-artery embolization.
The 6-to-8-point benefit, on average, in health related quality-of-life scores in the myomectomy group, as compared with the uterine-artery embolization group, is consistent with a small to-moderate standardized treatment benefit at 2 years.
In conclusion, this multicenter trial showed the superiority of myomectomy over uterine artery embolization with respect to health-related quality of life. The overall incidence of perioperative and postoperative complications was similar in the two groups.
Source: I. Manyonda, A.-M. Belli, M.-A. Lumsden et al; N Engl J Med
DOI: 10.1056/NEJMoa1914735
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


