- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Is Hysteroscopy Safe for diagnosing Type 2 Endometrial Cancer?
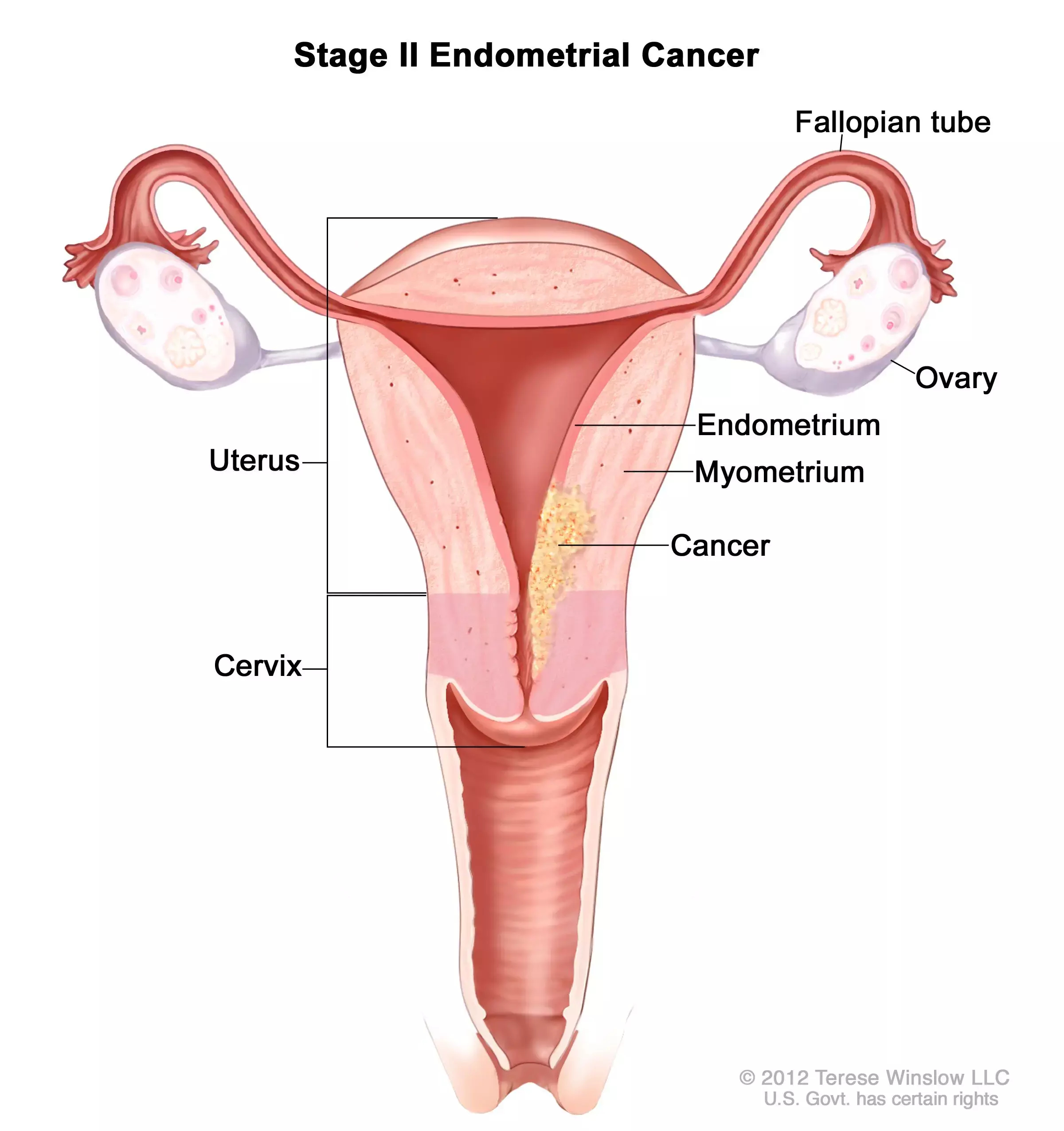
Endometrial cancer accounts for approximately 4% of all cancers in women and occurs predominantly after menopause. A recent study suggests diagnostic hysteroscopy may not be associated with increased odds of positive peritoneal cytology at the time of surgical staging or with decreased survival. The study findings are published in the Journal of Minimally Invasive Gynecology on October 19, 2020.
Hysteroscopy is a highly accurate method and is useful in diagnosing, rather than excluding endometrial cancer in women with abnormal uterine bleeding. This technique, however, flushes fluid and endometrial cells into the abdomen via the fallopian tubes, thus potentially spreading malignant cells. Several studies have associated hysteroscopy with an increased risk of positive peritoneal cytology in women with endometrial cancer, while certain studies have raised the possibility of an adverse impact of hysteroscopy on prognosis in women with endometrial cancer. Endometrial cells may shed during hysteroscopy and be passively transported with fluid into the peritoneal cavity. Moreover, it is important to assess this hypothesis into type 2 endometrial cancer, a more aggressive phenotype that usually presents with endometrial atrophy and worse prognosis. Therefore, researchers conducted a study to assess the prevalence of positive peritoneal cytology in type II endometrial cancer in women undergoing hysteroscopy as a diagnostic tool and determine their prognosis.
It was a randomized retrospective cohort study in 127 women with type II endometrial cancer at Tertiary centre, academic hospital. A total of 127 patients were randomly assigned to either diagnostic hysteroscopy (HSC)(n=43) or dilation/curettage (D&C)(n=84). Researchers evaluated the clinical and pathologic characteristics, including peritoneal cytology results. They used the Kaplan-Meier method to project survival curves and compared it with the log-rank test. They used Cox-regression analysis to assess factors related to disease-free survival (DFS).
Key findings of the study were:
♦ Upon analysis, they found no difference with regard to age between the groups.
♦ They observed that D&C group had a higher frequency of advanced staging and greater vascular invasion.
♦ They also found positive cytology in 2/43 (4.6%) women following HSC and in 9/84 (10.7%) patients following D&C.
♦ However, they found no statistically significant difference in the survival curve between groups.
♦ Upon Multivariate analysis for DFS, they found that advanced staging (III and IV) (HR=3.89), advanced age (HR=1.073) and vascular invasion (OR=3.01) increases the risk of recurrence.
The authors concluded, "Diagnostic HSC did not increase the rate of positive peritoneal cytology at the time of surgical staging in this cohort of women with type II endometrial cancer and presented equal safety when compared to D&C".
For further information:
Medical Dialogues Bureau consists of a team of passionate medical/scientific writers, led by doctors and healthcare researchers. Our team efforts to bring you updated and timely news about the important happenings of the medical and healthcare sector. Our editorial team can be reached at editorial@medicaldialogues.in.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


