- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Intrastromal injections effective adjunct to topical therapy in recalcitrant fungal keratitis
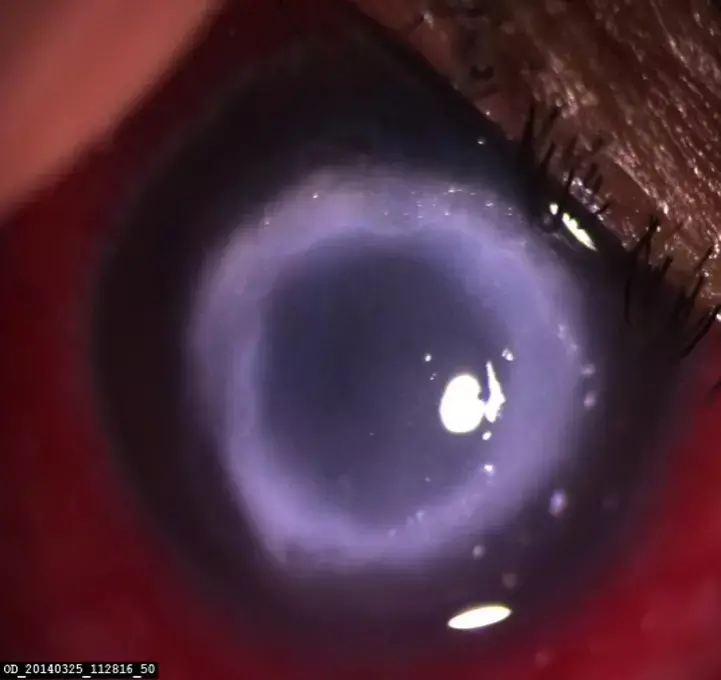
Fungal keratitis often presents with deep stromal abscess and endothelial plaque that needs to be managed timely and appropriately to prevent resultant ocular morbidity. Standard topical therapy with commonly used antifungal agents, namely, Natamycin (NTM) 5% and Voriconazole (VCZ) 1%, may not be sufficient for treating nonresponding fungal keratitis due to limited efficacy and the low capability of the medications to penetrate the deep layers of the cornea.
Various other interventions, such as penetrating keratoplasty (PKP), collagen crosslinking with photoactivated riboflavin (PACK-CXL), excisional keratectomy combined with focal cryotherapy and amniotic membrane inlay, have been proposed to deal with these cases. However, these have their own limitations and targeted delivery of antifungal agents at the ulcer site by means of intrastromal injections remains an effective alternative of bypassing these complex options. These injections are known to enhance the drug levels at the desired site of the cornea thereby allowing successful healing of the corneal ulcer.
Voriconazole is the most commonly used antifungal agent for intrastromal delivery (ISVCZ) and numerous studies have previously proven its efficacy in recalcitrant cases. Similarly, intrastromal Amphotericin-B (ISAMB) has also been employed successfully for targeted drug delivery.
Saluja et al conducted a randomized clinical trial to determine and compare the safety and efficacy of ISVCZ 50ug/ 0.1 mL, ISAMB 5ug/0.1 mL and ISNTM 10ug/0.1 mL as adjuncts to topical NTM 5% in cases of recalcitrant fungal keratitis.
The study was a prospective interventional study. Sixty eyes of 60 patients with microbiologically proven recalcitrant fungal keratitis (ulcer size >2 mm, depth >50% of stroma, and not responding to topical NTM therapy for two weeks) were recruited. Patients were randomized into three groups of 20 eyes, each receiving ISVCZ 50ug/ 0.1 mL, ISAMB, 5ug/0.1 mL and ISNTM 10ug/0.1 mL. The patients in all three groups continued topical NTM 5% every four hours until the ulcer healed. Primary outcome measure was time taken till complete clinical resolution of infection, and secondary outcome measure was best corrected visual acuity (BCVA) at six months.
All three groups had comparable baseline parameters. The mean duration of healing was significantly better (p=0.02) in the ISNTM group (34±5.2 days) as compared to the ISVCZ group (36.1±4.8 days) and the ISAMB group (39.2±7.2 days).
In the ISVCZ, ISAMB and ISNTM groups, 19/20 (95%), 18/20 (90%) and19/20 (95%) patients showed complete resolution of infection, respectively (p=0.8). Of these, 12/20 (60%), 11/20 (55%) and 13/20 (65%) patients healed with first injection; 6/20 (30%), 5/20 (25%) and 5/20 (25%) healed with second injection and 1/20 (5%), 2/20 (10%) and 1/20 (5%) healed with third injection in the ISVCZ, ISAMB and ISNTM groups, respectively. This implied that the maximum number of failures and patients needing repeat injections was seen in the ISAMB group (p=0.8). About 95%, 90% and 95% patients healed successfully in the ISVCZ, ISAMB and ISNTM groups, respectively.
In terms of healing, deep vascularization was significantly greater in the ISAMB group (55%, p=0.02) when compared to the ISVCZ and ISNTM groups (31% and 26%, respectively). While deep vascularization makes the cornea a high risk bed for corneal grafting in the future, the actual effect of these agents on graft survival needs to be ascertained with larger and longer studies.
The average time taken for re-epithelization and for disappearance of hypopyon was significantly higher in the ISAMB group compared to the ISVCZ and ISNTM groups. Mean time taken for complete resolution of stromal infiltrates and the mean scar size were comparable in all groups.
There were fewer repeat injections in the ISNTM group (7/20 vs 8/20 and 9/20 in the ISVCZ and ISNTM groups, respectively).
Intrastromal injections were administered at the residual host rim while performing penetrating keratoplasty; patients were also advised on topical and systemic antifungals.
Intracameral injections of antifungal drugs along with intrastromal injections have been found to be effective in the early resolution of endothelial plaque, but in this study, as natamycin was being given for the first time, intracameral injections were avoided. Also, to maintain uniformity in the management of reliable results, only intrastromal injections were administered in all patients.
The authors concluded, "Intrastromal antifungal agents can be a safe and useful adjunct to standard therapy for management of recalcitrant fungal keratitis, specifically caused by the filamentary fungi. However, regional differences in microbiological profile have to be considered before prescribing them. Based on our study results, ISVCZ seems to be the best first-line anti-stromal agent. However, novel composition of NTM holds promising results and its applicability for treating recalcitrant fungal keratitis can be explored in the future. However, larger long-term, randomized comparative trials are awaited to determine the most efficacious and safest intrastromal agent."
Source: Saluja et al; Clinical Ophthalmology 2021:15 2437–2446
Dr Ishan Kataria has done his MBBS from Medical College Bijapur and MS in Ophthalmology from Dr Vasant Rao Pawar Medical College, Nasik. Post completing MD, he pursuid Anterior Segment Fellowship from Sankara Eye Hospital and worked as a competent phaco and anterior segment consultant surgeon in a trust hospital in Bathinda for 2 years.He is currently pursuing Fellowship in Vitreo-Retina at Dr Sohan Singh Eye hospital Amritsar and is actively involved in various research activities under the guidance of the faculty.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


