- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Primary trabeculectomy bests primary medical treatment in advanced glaucoma: BMJ
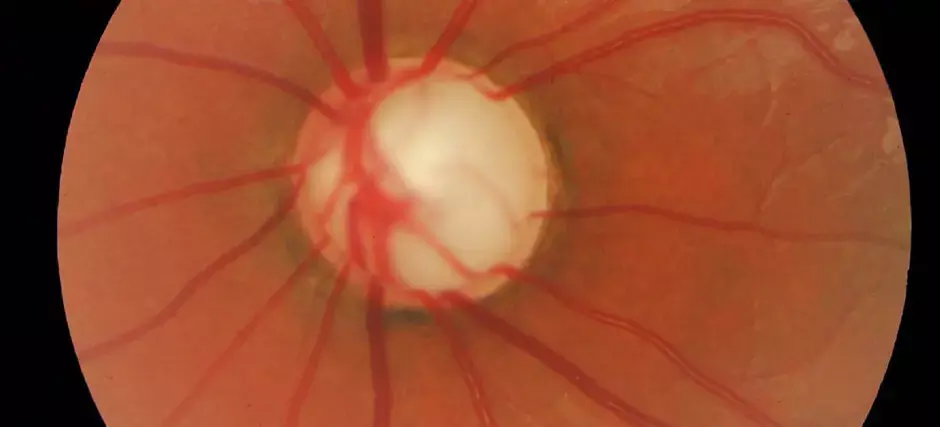
Glaucoma is a chronic progressive eye disease with substantial and detrimental effects on many aspects of daily living. The number of patients with glaucoma is predicted to increase substantially as the result of an ageing population.
Severe visual field loss occurs in people with advanced open angle glaucoma, which encroaches on central vision and eventually reduces visual acuity. People with advanced open angle glaucoma in both eyes, even with good visual acuity, may be eligible for certification as severely sight impaired.
The primary risk factor for blindness due to glaucoma is advanced vision loss at presentation. In the UK, guidelines from the National Institute for Health and Care Excellence (NICE) suggest that patients presenting with advanced disease should be offered trabeculectomy as a primary intervention but cite poor evidence to support this recommendation. Most patients are treated medically with escalating topical drug therapy, only undergoing trabeculectomy if medical management is not successful.
Effective treatment can control the disease, prevent further sight loss, and so prevent blindness. Reducing intraocular pressure is the only proven effective treatment for glaucoma. Better control of intraocular pressure at the initial stage following diagnosis reduces the risk of further progression.
A J King et al carried out a multicentre randomised controlled trial comparing primary medical management against primary trabeculectomy for people presenting with previously untreated advanced open angle glaucoma published in British Medical Journal.
The Treatment of Advanced Glaucoma Study (TAGS) was a pragmatic, multicentre, randomised unblinded controlled trial conducted in 27 centres in the UK. 453 adults presenting with newly diagnosed advanced open angle glaucoma in at least one eye (Hodapp classification) between 3 June 2014 and 31 May 2017 were included in this study. Intervention included Mitomycin C augmented trabeculectomy (n=227) and escalating medical management with intraocular pressure reducing drops (n=226).
The primary outcome was health related quality of life measured using the Visual Function Questionnaire-25 (VFQ-25) at 24 months. Secondary outcomes included patient reported outcomes: the EuroQol Group's 5 dimension 5-level health status questionnaire (EQ5D-5L), the Health Utility Index-mark 3 (HUI-3), the Glaucoma Utility Index (GUI) and the patient's experience.
Results:
- At 24 months, the mean VFQ-25 scores were 85.4 (13.8) and 84.5 (16.3) in the trabeculectomy and medical management arms, respectively. The mean difference was 1.06 (95% confidence interval −1.32 to 3.43; P=0.38) (table 2). The per protocol and complier average causal effect estimates for VFQ-25 were similar.
- No evidence was reported of any differences for EQ-5D-5L, HUI-3, and GUI at 24 months .
- The mean intraocular pressure at 24 months was 12.4 (SD 4.7) mm Hg for the trabeculectomy arm and 15.1 (4.8) mm Hg for the medical management arm (mean difference −2.75 (95% confidence interval −3.84 to −1.66) mm Hg; P<0.001)
- No evidence was found of a difference in visual field mean deviation at 24 months or other secondary outcomes
- The need for additional interventions was greater in the trabeculectomy arm. All glaucoma surgery related serious adverse events (flat anterior chamber, ocular perforation during anaesthesia, diplopia, and bleb related endophthalmitis) needed further surgical intervention.
- Of the adverse events reported, 27 patients needed further intervention to manage them, 24 in the trabeculectomy arm and three in the medical management arm.
At 24 months, the study found no difference between treatment arms in the primary outcome, VFQ-25 score, which is an established method of assessing glaucoma related quality of life.
Compared with baseline, surgery was more effective in lowering intraocular pressure at all time points measured where a reduction to 12.4 (SD 5.7) mm Hg was noted at four months, and it remained at around 12 mm Hg for the remainder of the study. A sustained reduction in intraocular pressure is recognised to be the most effective method of preventing further visual field loss in glaucoma. The trabeculectomy arm required far fewer topical medications for control of intraocular pressure. Adverse events were similar between arms.
For patients, maintaining their quality of life and independence is the most important outcome from their glaucoma management. Both eyes contribute to vision related quality of life, so this reflects the true visual experience of patients and reports the visual outcomes they achieve.
At 24 months, the modest deterioration in visual acuity is potentially due to the development of early cataract in the trabeculectomy arm. Quality of life and requirement for cataract surgery were very similar in both arms at 24 months. The study found no substantive difference between arms for the other main measure of visual function and disease progression, the visual field test.
A major concern for clinicians was the perceived "high risk" of complications associated with trabeculectomy. The overall frequency of adverse events was broadly similar between the treatment arms. Two specific concerns of clinicians related to trabeculectomy were risk of blindness from bleb related endophthalmitis and risk of unexplained visual loss ("wipe-out") immediately after surgery. No unexplained loss of vision occurred immediately after surgery, indicating no occurrence of wipe-out.
Strengths of this study was it adopted a pragmatic approach to replicate current clinical practice in the management of advanced glaucoma as closely as possible. The inclusion of multiple centres and multiple surgeons undertaking standard trabeculectomy, along with the use of available topical medications, ensured that this study was representative of the current standard of care. Both of the interventions used in TAGS are used routinely worldwide to lower intraocular pressure.
Limitations included the fact that treatments and patient reported outcome measures could not be masked from participants or clinicians. Although the design of the trial was pragmatic, completion of questionnaires would not be part of standard care. This may have affected participants' feeling of wellbeing either in a negative way owing to the burden of completion or in a positive way owing to the perception that they were being well cared for.
The researchers concluded, "TAGS showed no difference in quality of life between treatment arms. Surgery was safe and achieved a sustained greater reduction in intraocular pressure compared with primary medication. This study provides the first direct evidence of the outcomes of interventions for patients presenting with advanced glaucoma. These results will inform clinicians and patients in making treatment choices."
Source: Anthony J King, Jemma Hudson, Gordon Fernie et al, BMJ 2021;373:n1014
http://dx.doi.org/10.1136/bmj.n1014
Dr Ishan Kataria has done his MBBS from Medical College Bijapur and MS in Ophthalmology from Dr Vasant Rao Pawar Medical College, Nasik. Post completing MD, he pursuid Anterior Segment Fellowship from Sankara Eye Hospital and worked as a competent phaco and anterior segment consultant surgeon in a trust hospital in Bathinda for 2 years.He is currently pursuing Fellowship in Vitreo-Retina at Dr Sohan Singh Eye hospital Amritsar and is actively involved in various research activities under the guidance of the faculty.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


