- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Giant retinal tear in child with Marfan's syndrome: a rare ocular emergency reported in BMJ
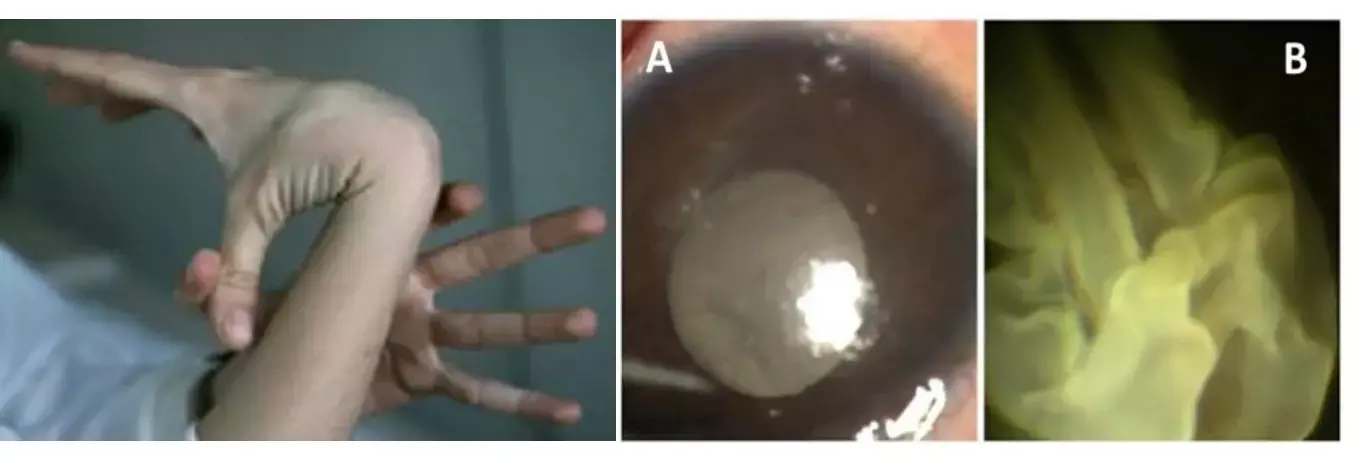
Giant retinal tears (GRTs) are reported in 16%–18% of paediatric retinal detachments. The risk factors for GRTs include trauma, high myopia, and systemic diseases like Marfan's syndrome, sticklers syndrome, atopic dermatitis and other disorders.
Parrina et al from Government Hospital, Chandigarh reported an interesting case of rhegmatogenous retinal detachment with giant retinal tear in a child with marfanoid features.
A 7-year-old male child with Marfanoid habitus presented with sudden and painless decrease in the vision of the right eye . He denied any past history of similar complaints. Upon general examination, patient was tall for his age, the extremities showed abnormalities like long, thin, slender digits and genu valgum suggesting Marfanoid habitus and pectus deformities of chest and hyperflexibility of the joints in the extremities.
On ocular examination, the child had best-corrected visual acuity (BCVA) of perception of light with accurate projection of rays in right eye and 20/80 with −11.00 D spherical lens in left eye. Slip-lamp biomicroscopy revealed a clear anterior segment and no evidence of subluxation of lens. Upon fundocscopy of right eye, there was tobacco dusting in the anterior vitreous with crumpled retina obscuring the view of optic disc and leaving the large area of bare choroid .In the left eye they noted an area of lattice degeneration from 10'o clock to 3'o clock hours with few small retinal breaks .
Paediatric consultation was taken which later confirmed the provisional diagnosis of Marfan's syndrome after going through complete systemic workup. Echocardiography done to rule cardiac and valvular abnormalities was reported as normal. Facilities for genetic workup were not available at the center and parents also refused to get genetic testing done for the child from outside.
The patient underwent a combined procedure comprising scleral bucking and pars plana vitrectomy (PPV) with silicone oil tamponade with 360° endolaser in right eye. Focal laser treatment for the breaks within lattice degeneration was done in left eye.
At 4 weeks follow-up visit, the patient came with decreased vision in OS after a trivial trauma. Examination of left eye showed crumbled retina with bare choroid similar to right eye presentation in past. Hence he underwent pars plana vitrectomy (PPV) with silicone oil tamponade with 360° endolaser in the left eye.
At 6 months after parsplana vitrectomy of the right eye, the patient developed cataract for which phacoaspiration with posterior chamber intraocular lens implantation was done.
On the last follow-up examination at 9 months, child had gained the best corrected visual acuity of 20/200 in right eye and 20/80 in left eye with attached retina showing no signs of any recurrence of RRD or new breaks or silicone oil emulsification.
Marfan's syndrome is one of the rare genetic disorders with an autosomal dominant inheritance which can result in various systemic abnormalities in major organs like the skeleton, heart, aorta, eyes and lungs. Ocular complications like ectopia lentis (50%–80%) are commonly seen as compared with retinal detachment (5%–11%) in this disease. In recent times, the prognosis of paediatric retinal detachments with GRTs has improved with the advancements in vitreoretinal surgical techniques.
Authors conclude: "we would like to highlight the need for early aggressive ocular screening in children who are diagnosed with Marfan's syndrome and the need for prophylactic treatment in the unaffected eye."
Source: Sehgal P, Narang S, Chandra D. Rhegmatogenous retinal detachment with giant retinal tear in a child with Marfan's syndrome: a rare ocular emergency. BMJ Case Rep. 2021 Jun 2;14(6):e241354. doi: 10.1136/bcr-2020-241354.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


