- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Management of Chronic Insomnia Disorder and Obstructive Sleep Apnea: VA/DoD guidelines
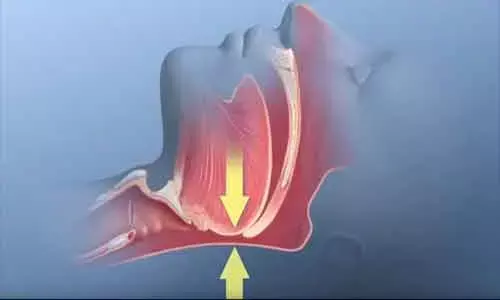
SAN ANTONIO - The U.S. Departments of Veterans Affairs and Defense (VA/DoD) jointly have issued new guidelines for assessment and treatment of insomnia and obstructive sleep apnea. The guidelines have been published in the Annals of Internal Medicine.
"This is a major step for these two organizations in recognizing the importance of appropriately diagnosing and treating sleep disorders in these unique populations," said Vincent Mysliwiec, M.D., a sleep medicine physician, researcher and retired U.S. Army colonel who helped author the guidelines.
Military service is an established risk factor for sleep disorders, which are considerably more prevalent in military personnel and veterans than in the general U.S. population. These populations also have high rates of traumatic brain injury, posttraumatic stress disorder (PTSD), and other mental health disorders, which combined with insomnia and/or sleep apnea complicate the treatment of affected military personnel and veterans.
Nearly half of U.S. military personnel have reported poor sleep quality, including insomnia symptoms. Insomnia is one of the most common sleep disorders and affects up to 41 per cent of active-duty military personnel deployed to combat zones, 25 per cent of noncombatants and 20 per cent of those preparing for deployment.
One study found a six-fold increase in sleep disorders among veterans between 2003 and 2010 when millions were deployed to Iraq and Afghanistan. In that study, 4.5 per cent of veterans were diagnosed with sleep-disordered breathing, including sleep apnea, a condition in which blockage of the airway interferes with breathing at night. Importantly, sleep apnea increases the risk of cardiovascular disease and motor vehicle crashes. The study also found that 2.5 per cent of veterans were diagnosed with insomnia.
Dr Mysliwiec's group concluded in the journal article that the actual prevalence of chronic insomnia among veterans likely is considerably higher because it often is not documented in the medical record. Insomnia can cause daytime sleepiness and cognitive impairment and can adversely affect mental and physical health.
In other research, veterans have reported insomnia rates as high as 50 per cent.
This synopsis summarizes the key recommendations of the guideline in 3 areas: diagnosis and assessment of OSA and chronic insomnia disorder, treatment and management of OSA, and treatment and management of chronic insomnia disorder. Three clinical practice algorithms are also included.
The "VA/DoD Clinical Practice Guideline for the Management of Chronic Insomnia Disorder and Obstructive Sleep Apnea" is based on evidence-based and effective therapies for military personnel and veterans with chronic insomnia disorder and sleep apnea, while including evidence from civilian studies. The VA/DoD work group's 41 recommendations in the clinical practice guideline (CPG) are relevant to all military, VA, and civilian providers who treat patients with sleep disorders.
Main recommendations in the CPG include:
1. Use of positive airway pressure therapy (commonly known as CPAP) for the entirety of a patient's sleep period.
2. Continued use of CPAP even with patients who do not use it for at least the common insurance provider standard of four hours per night, while addressing barriers to CPAP adherence.
3. Interventions to improve CPAP adherence in patients with sleep apnea and co-occurring PTSD, anxiety, and/or insomnia upon initial diagnosis because these patients have higher rates of non-adherence.
4. For chronic insomnia, notable recommendations include:
5. Cognitive-behavioural therapy for insomnia is the recommended treatment, but a shortened version called brief behavioural therapy for insomnia is also acceptable for some patients.
6. Sleep hygiene - habits that promote nighttime sleep quality, such as limiting the length of daytime naps and avoiding stimulants close to bedtime - while important, should not be used as a stand-alone therapy for chronic insomnia disorder.
7. Some medications may be used as a second-line treatment for chronic insomnia, but antipsychotic drugs and over-the-counter agents such as antihistamine and melatonin are not helpful for treating chronic insomnia.
"We expect the guidelines to be far-reaching and lead to necessary changes in clinical practice while helping to determine what clinical and research questions will need to be addressed in military personnel and veterans," Dr Mysliwiec said. "Whereas in the past, problems with sleep disorders have been discounted, there is growing recognition of the importance of sleep health and treating sleep disorders."
for further references log on to:
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


