- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
COVID-19 Pneumonia Patient significantly Improves with Laser: Case report
Cutting Edge Laser Technologies
LOWELL, Mass - Dr. Scott Sigman, principal investigator and lead author, reported today positive results from the first-ever use of laser therapy to treat a COVID-19 pneumonia patient.
The case has been published in the American Journal of Case Reports.
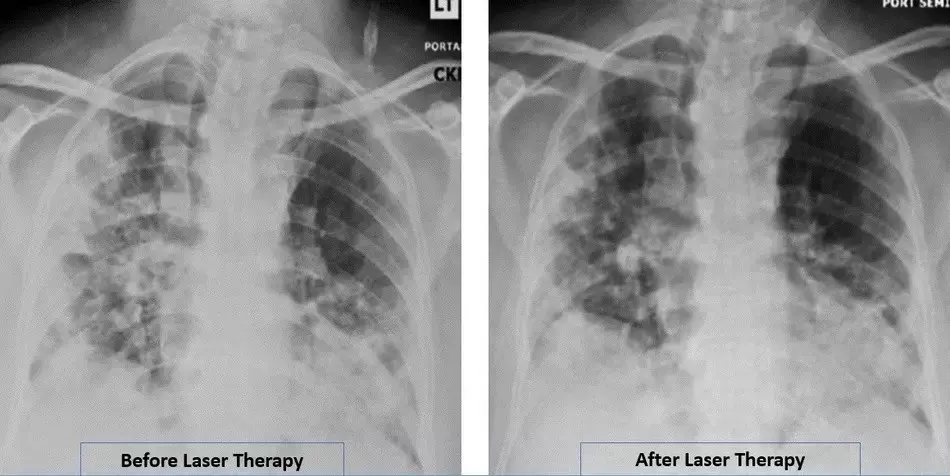
According to the history of case, after supportive treatment with Photobiomodulation Therapy (PBMT) the patient's respiratory indices, radiological findings, oxygen requirements and outcomes improved over several days and without the need for a ventilator.1 The patient in this report is part of a randomized clinical pilot trial involving 10 patients with confirmed COVID-19.
The patient, a 57-year-old African American man diagnosed with SARS-CoV-2, was admitted to the ICU for respiratory distress and in need of oxygenation. He was treated with once-daily, 28-minute PBMT sessions for four days using an FDA-cleared Multiwave Locked System (MLS) Therapy Laser (ASA Laser, Italy). The MLS Therapy Laser used in this study is distributed exclusively in North America by Cutting Edge Laser Technologies based in Rochester, N.Y. The patient's response to PBMT was evaluated by comparing different scoring tools before and after laser therapy, all of which improved following therapy. Results showed:
- Oxygen saturation (SpO2) increased from 93–94% to 97–100%
- Oxygen requirement decreased from 2–4 L/min to 1 L/min
- RALE Chest X-ray score improved from 8 to 5
- Pneumonia Severity Index improved from Class V (142) to Class II (67)
- Pulmonary indices, Brescia-COVID and SMART-COP, both decreased from 4 to 0
- C-Reactive Protein normalized from 15.1 to 1.23
- Community-Acquired Pneumonia assessment tool reported substantial improvement
Prior to treatment, the patient was bedridden with a severe cough and inability to ambulate. Upon completion of treatment, the patient's cough resolved, and he was able to ambulate with physical therapy. On the following day, he was discharged to an acute rehabilitation facility on minimum supportive oxygen. Just one day later, the patient was able to complete two trials of stair climbing with physical therapy and was in the process of weaning to room air. On follow-up, his clinical recovery in total was three weeks, whereas the median time is typically six to eight weeks.
"Adjunct Photobiomodulation Therapy effectively treated respiratory symptoms in a severe case of COVID-19 pneumonia. We consider this therapeutic option to be a feasible supportive treatment modality," said Dr. Sigman. "There is continued medical need for more safe and effective COVID-19 treatment options. We are hopeful that this report and subsequent study will encourage others to consider additional clinical trials with the use of adjunct PBMT for COVID-19 pneumonia."
In PBMT, light is applied over damaged tissues, and light energy is absorbed by cells starting a cascade of molecular reactions that improve cell function and enhance the body's healing process. PBMT has demonstrated anti-inflammatory effects and is emerging as an alternative modality in pain management, lymphedema treatment, wound healing and musculoskeletal injuries. The utilization of supportive PBMT for COVID-19 is based on the theory that the laser light reaches the lung tissue to relieve inflammation and promote healing. Additionally, PBMT is non-invasive, cost-effective, and has no known adverse effects.
The MLS laser uses a mobile scanner with 2 synchronized laser diodes, one in pulse mode (adjustable to 1–2000 Hz), emitting at 905 nm, and another in pulsed mode emitting at 808 nm. The two laser wavelengths work simultaneously and are synchronized. The laser is placed 20 cm above the patient across the lung fields while in the prone position. The laser is painless, and patients typically are unaware that the laser treatment is occurring. This laser is routinely used for deeper tissues like hips and pelvic joints that are surrounded by thick muscles. The therapeutic dose used to reach the deep targets of the pelvis is 4.5 J/cm2. Based on calculations by Dr. Soheila Mokmeli, co-author of the study, 7.2 J/cm2 was used over the skin, delivering a therapeutic dose just over 0.01 J/cm2 of laser energy to the lung. This dosage is able to penetrate the chest wall and reach the lung tissue creating an anti-inflammatory effect that in theory blocks the effects of the cytokine storm seen in COVID-19 pneumonia.
For further reference log on to:
Am J Case Rep 2020; 21:e926779 ::
Hina Zahid Joined Medical Dialogue in 2017 with a passion to work as a Reporter. She coordinates with various national and international journals and association and covers all the stories related to Medical guidelines, Medical Journals, rare medical surgeries as well as all the updates in the medical field. Email: editorial@medicaldialogues.in. Contact no. 011-43720751
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


