- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Appropriate use of high-flow nasal oxygen in acute respiratory failure: ACP updates recommendations
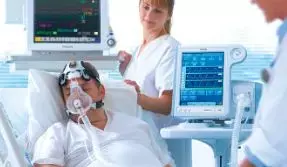
The American College of Physicians (ACP) has released updated guidelines to provide clinical recommendations on the appropriate use of high-flow nasal oxygen (HFNO) in hospitalized patients for initial or postextubation management of acute respiratory failure. The current recommendations are based on the best available evidence on the benefits and harms of HFNO, taken in the context of costs and patient values and preferences. They have been put forth in Annals of Internal Medicine.
High -flow nasal oxygen involves the delivery of warm and humidified oxygen via a small nasal cannula at a flow higher than the patient's inspiratory flow (up to 60 L/min). The purported benefits of HFNO versus conventional oxygen therapy (COT) (low-flow systems [nasal cannulae or masks] and high-flow systems [masks]) and noninvasive ventilation (NIV) (continuous or bilevel positive airway pressure ventilation) include improved patient comfort and physiologic advantages, such as improved oxygenation and ventilation, better pulmonary compliance, reduced anatomical dead space, modest positive end-expiratory pressure, more efficient respiratory effort, reduced work of breathing, and secretion clearance.
The ACP Clinical Guidelines Committee based these recommendations on a systematic review on the efficacy and safety of HFNO. The patient-centered health outcomes evaluated included all-cause mortality, hospital length of stay, 30-day hospital readmissions, hospital-acquired pneumonia, days of intubation or reintubation, intensive care unit (ICU) admission and ICU transfers, patient comfort, dyspnea, delirium, barotrauma, compromised nutrition, gastric dysfunction, functional independence at discharge, discharge disposition, and skin breakdown. This guideline was developed using the GRADE (Grading of Recommendations Assessment, Development and Evaluation) method.
The target audience was all clinicians, and the target patient population is adult patients with acute respiratory failure treated in a hospital setting (including emergency departments, hospital wards, intermediate or step-down units, and ICUs).
The key highlights have been summerised below.
- Recommendation 1a:ACP suggests that clinicians use high-flow nasal oxygen rather than noninvasive ventilation in hospitalized adults for the management of acute hypoxemic respiratory failure (conditional recommendation; low-certainty evidence). The evidence showed demonstrable improvement in clinically meaningful outcomes, including a large reduction in mortality, modest reduction in intubations and in hospital-acquired pneumonia as well as an improvement in patient comfort. Additionally, the CGC considered that most patients can use HFNO and there are usually no contraindications unless related to issues with fitting the nasal cannula.
- Recommendation 1b:ACP suggests that clinicians use high-flow nasal oxygen rather than conventional oxygen therapy for hospitalized adults with postextubation acute hypoxemic respiratory failure (conditional recommendation; low-certainty evidence). In this population, evidence showed HFNO may reduce re-intubation slightly and may improve patient comfort compared to COT, and that HFNO may not perform worse than COT with regard to all-cause mortality, hospital-acquired pneumonia, and length of ICU stay.
Keeping in mind the current pandemic scenario, the team opined that High-flow nasal oxygen is an aerosol-generating procedure and requires higher grades of personal protective equipment (respiratory protective devices) than routine procedures that do not involve aerosol generation.
"More research is needed to identify which patients (for example, high-risk patients) are most likely to benefit from HFNO, particularly by type of acute respiratory failure. Current evidence is insufficient on the use of HFNO in patients with hypercapnic respiratory failure because included studies typically did not specify whether patients with hypercapnic acute respiratory failure were excluded, or when included, the studies did not report findings by type of acute respiratory failure."the team concluded.
For full article follow the link: https://doi.org/10.7326/M20-7533
Primary source: Annals of Internal Medicine
Dr Satabdi Saha (BDS, MDS) is a practicing pediatric dentist with a keen interest in new medical researches and updates. She has completed her BDS from North Bengal Dental College ,Darjeeling. Then she went on to secure an ALL INDIA NEET PG rank and completed her MDS from the first dental college in the country – Dr R. Ahmed Dental College and Hospital. She is currently attached to The Marwari Relief Society Hospital as a consultant along with private practice of 2 years. She has published scientific papers in national and international journals. Her strong passion of sharing knowledge with the medical fraternity has motivated her to be a part of Medical Dialogues.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


