- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
T-tube for biliary drainage does not prevent postoperative complications in Parkinson's patients, suggests study
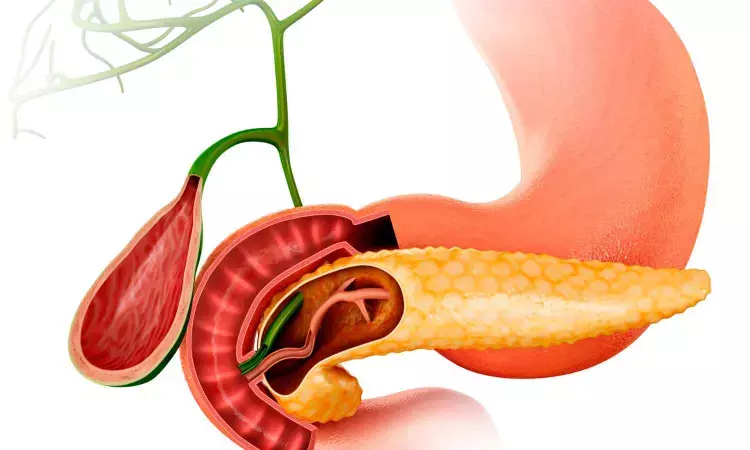
A new study published in the journal of BMC Surgery found that the use of a T-tube in pancreaticoduodenectomy (PD) is not a practical way to avoid postoperative problems. Pancreaticoduodenectomy is usually used to treat malignant tumors of the distal bile ducts, ampulla, and pancreatic head. A few instances of chronic pancreatitis, benign ampullary tumors, and injury to the pancreatic head duodenum can also be treated with PD. With a reported incidence rate of 3-5% in prior research, biliary anastomotic stricture (BAS) is an uncommon long-term complication that follows Parkinson's disease (PD) surgery.
Prior studies have indicated that the implementation of external T-tube biliary drainage may lower the incidence of postoperative problems related to Parkinson's disease (PD), particularly the incidence of clinically relevant postoperative pancreatic fistula (CR-POPF). Thus, this research was set out to assess whether T-tube biliary drainage after Parkinson's disease (PD) was necessary and practical as it's prophylactic impact on biliary anastomotic stricture has given special attention.
This research included patients who had pancreaticoduodenectomy performed at the facility between July 2016 and June 2020. The patients were separated into T-tube groupings and non-T-tube groups based on whether a T-tube was implanted during the procedure. the data gathered through an examination of the electronic health record system. Gender, age, BMI, length of stay after surgery (LOSAS), estimated blood loss (EBL), pathological diagnosis, size of mass, bile duct diameter, and postoperative complications (Bile leakage, postpancreatectomy hemorrhage (PPH), intra-abdominal infection (IAI), CR-POPF, and delayed gastric emptying) were the baseline data that were collected. Biliary anastomotic stricture (BAS) was the main goal of this study.
The findings of the study suggest that 330 individuals in all (Not-T-tube group = 226; T-tube group = 104) had PD. 222 participants were selected for further analysis using propensity score matching (Not-T-tube group =134, T-tube group = 88). The demographics of the patients in the matched groups were similar. The T-tube group had noticeably greater frequencies of clinically relevant postoperative pancreatic fistula (CR-POPF). Biliary anastomotic stricture (BAS) was observed in 3.15% of cases overall. Although the incidence of T-tube group was somewhat lower, there was no substantial difference. Overall, after PD, T-tube biliary drainage does not reduce the risk of developing BAS or postoperative sequelae.
Source:
Luo, X., Zhuo, X., Lin, X., Lin, R., Yang, Y., Wang, C., Fang, H., Huang, H., & Lu, F. (2024). Whether T-tube biliary drainage is necessary after pancreaticoduodenectomy: a single-center retrospective study. In BMC Surgery (Vol. 24, Issue 1). Springer Science and Business Media LLC. https://doi.org/10.1186/s12893-024-02570-5
Neuroscience Masters graduate
Jacinthlyn Sylvia, a Neuroscience Master's graduate from Chennai has worked extensively in deciphering the neurobiology of cognition and motor control in aging. She also has spread-out exposure to Neurosurgery from her Bachelor’s. She is currently involved in active Neuro-Oncology research. She is an upcoming neuroscientist with a fiery passion for writing. Her news cover at Medical Dialogues feature recent discoveries and updates from the healthcare and biomedical research fields. She can be reached at editorial@medicaldialogues.in
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


