- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Dasiglucagon effective treatment for postprandial hypoglycemia after weight loss surgery: Study
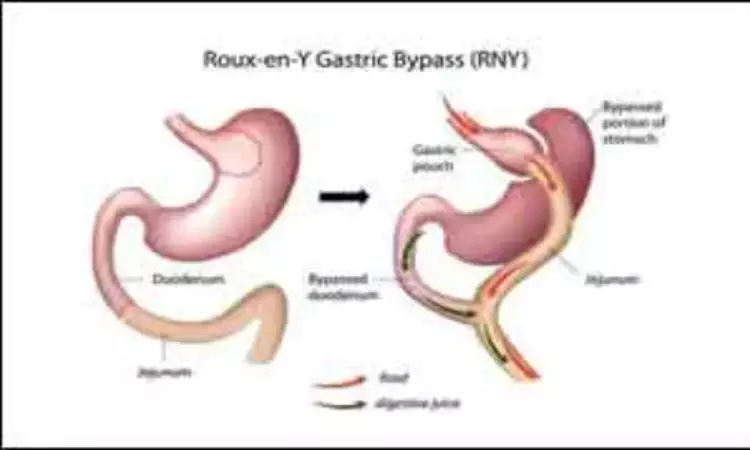
Denmark: Dasiglucagon could be a new therapeutic option for the management of postprandial hypoglycemia (low blood sugar) after weight loss surgery, suggests a recent study in the ADA journal Diabetes. The study found that the administration of dasiglucagon effectively improved postprandial hypoglycemia after Roux-en-Y gastric bypass (RYGB). Dasiglucagon is a novel, stable glucagon analog.
There is sufficient clinical and mechanistic evidence to support inclusion of metabolic surgery among antidiabetes interventions for controlling blood sugar and weight in people with T2D and obesity.
Reactive hypoglycemia (postprandial hypoglycemia) refers to low blood sugar that occurs after a meal — usually within four hours after eating. This is different from low blood sugar (hypoglycemia) that occurs while fasting.
Postprandial hypoglycemia or sudden and serious fall of blood sugar is a frequent and debilitating complication following RYGB without effective treatments. In a proof-of-concept study, Casper K. Nielsen from Denmark and colleagues investigated the effects of dasiglucagon on postprandial hypoglycemia after RYGB.
The randomized crossover study consisted of Ten RYGB-operated individuals with confirmed symptomatic postprandial hypoglycemia (plasma glucose concentration (PG) <3.5 mmol×L-1). The study involved three study days each including a standardized liquid mixed meal test (25 kJ per kg body mass; 50% carbohydrates, 35% fat and 15% protein). Subcutaneous injection of either placebo, 80 or 200 µg dasiglucagon (D80µg and D200µg) was administered after the postprandial PG peak, ten minutes before the projected time point where PG returned to fasting levels, using a subject-specific linear regression model. Blood sampling and assessment of hypoglycemic symptoms (Edinburgh Hypoglycemia Symptom Scale) were performed at fixed time intervals.
Key findings of the study include:
- Compared with placebo, treatment with both D80µg and D200µg significantly increased nadir PG (placebo: 3.0±0.2 mmol×L-1; D80µg: 3.9±0.3 mmol×L-1; D200µg: 4.5±0.2 mmol×L-1; P=0.002 and P=0.0002) and PG incremental area under the curve (iAUC70-240min) after drug administration (placebo: 752±19 mmol×L-1×min; D80µg: 917±22 mmol×L-1×min; D200µg: 992±28 mmol×L-1×min).
- Both doses reduced time spent in hypoglycemia (<3.9 mmol×L-1) (placebo: 62.0±8 min; D80µg: 27.5±12 min; D200µg: 14.0±9 min).
- There were no significant changes in hypoglycemic symptoms between the three study days.
"Administration of dasiglucagon effectively ameliorates postprandial hypoglycemia representing a promising new therapeutic option for management of postprandial hypoglycemia after RYGB," concluded the authors.
The study, "Dasiglucagon Ameliorates Postprandial Hypoglycemia after Roux-en-y Gastric Bypass," is published in the ADA journal Diabetes.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


