- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Study Suggests: Accessory Renal Arteries May Be Innocent Bystanders in Prenatal Hydronephrosis
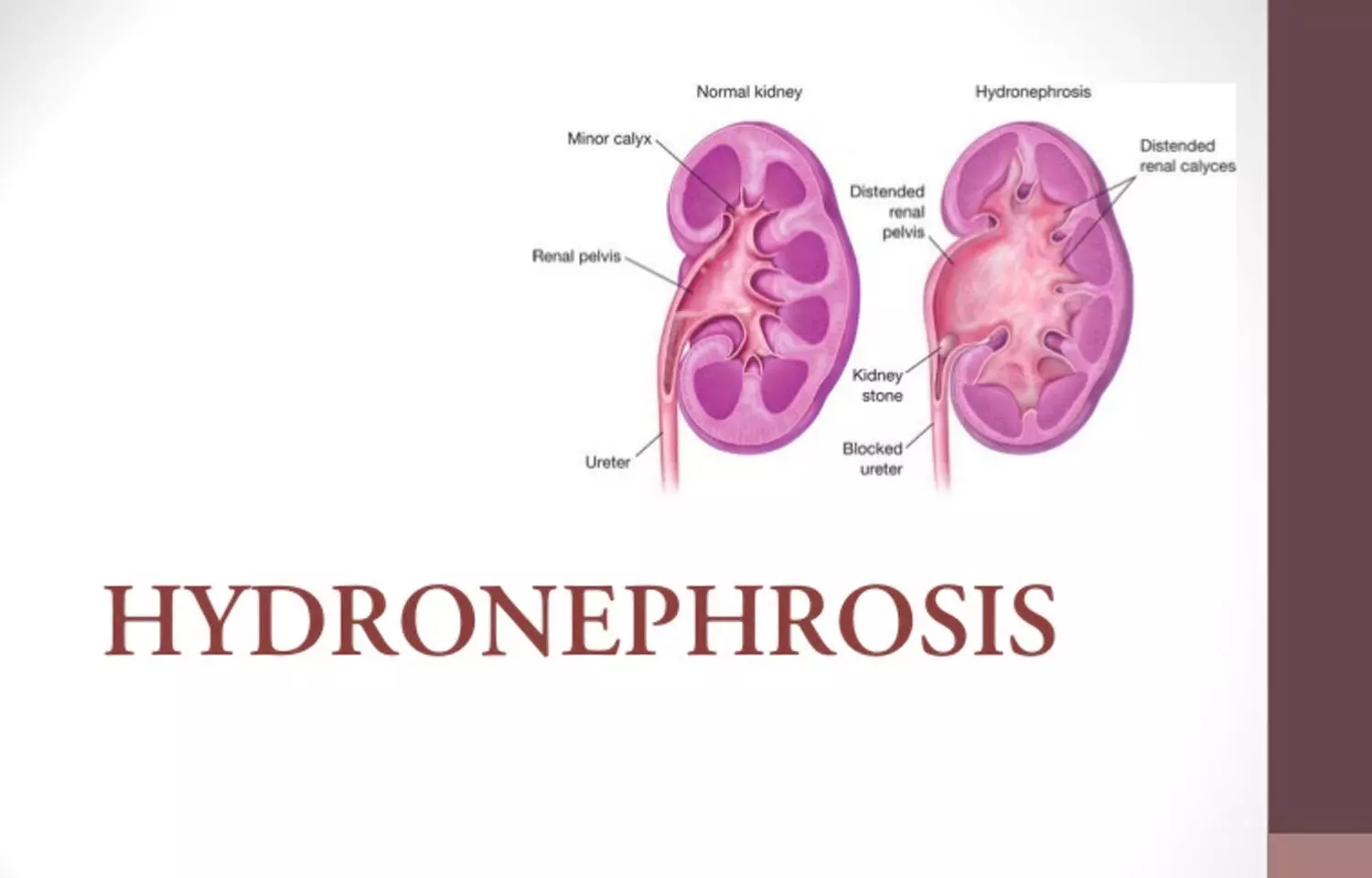
Going Beyond the Surface: What Causes Prenatal Hydronephrosis?
Prenatal hydronephrosis, or swelling of the fetal kidney, is a common finding on routine pregnancy ultrasounds. While many cases are harmless, some indicate underlying urinary tract issues. One possible cause? Accessory renal arteries (ARAs)—extra blood vessels supplying the kidneys, which are known to sometimes compress the urinary tract after birth. But are they really to blame before birth?
The Study: Peeking Into Fetal Kidneys
A team of researchers in Turkey set out to answer this mystery. In their prospective observational study, they recruited 123 pregnant women between 18 and 36 weeks’ gestation. Of these, 67 had fetuses with hydronephrosis and 56 had healthy controls. Each fetus underwent detailed ultrasound and Doppler imaging to detect ARAs and measure kidney size, volume, and blood flow.
What Did They Find?
ARAs were more common in fetuses with hydronephrosis (10.4%) than in controls (3.6%), but this difference wasn’t statistically significant.
No differences in kidney measurements: Whether or not ARAs were present, kidney size, kidney swelling, and blood flow in the main artery remained similar.
Most cases of hydronephrosis resolved after birth—including in those with ARAs.
No major postnatal complications tied directly to ARAs were observed in this small sample.
What Does This Mean for Families and Clinicians?
The results suggest that while ARAs are a little more common in fetuses with hydronephrosis, they’re likely just a normal anatomical variation—not a cause for alarm, nor a reliable predictor of future kidney trouble in most cases. Most babies—even those with both hydronephrosis and ARAs—will see the swelling go away naturally after birth.
However, as the study was limited in size, larger research is needed to confirm that ARAs don’t play a more significant role in select cases.
Key Takeaways
Accessory renal arteries are more often seen in fetuses with kidney swelling, but not by a significant margin.
No evidence was found that ARAs affect fetal kidney size, swelling, or blood flow before birth.
Most prenatal hydronephrosis, even with ARAs, resolves naturally after birth.
ARAs appear to be a normal variant rather than a culprit in prenatal hydronephrosis.
Larger studies are needed, but families can be reassured that extra arteries rarely mean trouble before birth.
Citation:
Avcı EA, Bülbül GA, Tsakır B, Sayal HB, Yavuz A. Accessory renal arteries in prenatal hydronephrosis: pathophysiologic contributor or incidental vascular finding? A prospective observational study. BMC Pregnancy and Childbirth. 2026. https://doi.org/10.1186/s12884-026-09169-z


