- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Novel oral, multi-kinase inhibitor therapy effective in exudative AMD: APEX trial
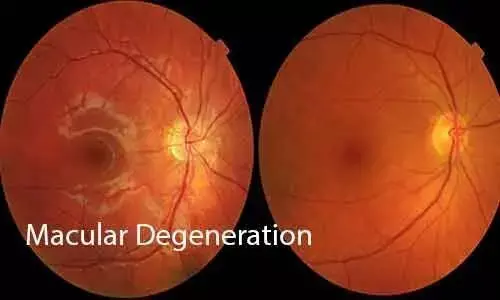
Age-related macular degeneration (AMD) is one of the most common causes of visual loss, projected to affect nearly 200 million people worldwide. Roughly two-thirds of the cases of late stage AMD involve CNV, manifest by the exudation of fluid and blood, often resulting in vision loss and a fibrotic scar if untreated.
Intravitreal injections of vascular endothelial growth factor (VEGF) inhibitors diminish the extent of exudation arising from CNV. Treatment with anti-VEGF agents may lead to an upregulation of platelet-derived growth factor (PDGF), which has been implicated in the recruitment, survival and subsequent maturation of pericytes—cells that are essential in the formation and maturation of neovascular complexes. These pericytes, fuelled by PDGF, may supply key growth factors, like VEGF, that promote the growth and stabilisation of CNV, which may result in a level of resistance to anti-VEGF therapy. If both VEGF and PDGF can be simultaneously targeted, then it might be possible to have a synergistic effect on inhibiting blood vessel formation.
X-82 is an oral, multi-kinase inhibitor of both VEGF and PDGF, which is structurally related to other multi-kinase inhibitors and is a potent inhibitor of angiogenesis. The most common adverse events (AEs) were diarrhoea (17%) nausea (14%) and fatigue (14%).
Based upon promising retreatment results, a phase II trial was conducted to evaluate the safety and efficacy of X-82 administered orally for the treatment of wet AMD by Cohen MN et al published in British Journal of Ophthalmology.
This phase II, randomised, double-masked, placebo-controlled trial enrolled subjects with a prior diagnosis of exudative AMD having received at least two intravitreal injections of anti-VEGF therapy. Subjects were randomised equally into four groups that received either daily 50mg, 100mg or 200mg dosages of X-82 or a placebo tablet. At each 4-week interval visit for 52 weeks, subjects were to be assessed to determine if rescue treatment was needed with anti-VEGF therapy.
The primary outcome was the change in the ETDRS visual acuity score from Day 1 to Week 52 after randomisation. A secondary outcome measure involved the number of anti-VEGF injections that were required in the treatment arm during the first 52 weeks after randomisation compared with the placebo group.
A total of 157 participants were enrolled at 39 sites across the USA. A total of 103 subjects completed the study up to and including the week 56 follow-up visit.
Overall, the ITT population started with a mean visual acuity of 71.0 and ended with a mean of 72.3 at week 52. Those in the 50 mg, 100 mg, 200 mg and placebo groups had a mean change from baseline in visual acuity of 0.2, −0.9, 1.7 and −0.3 letters at week 52, respectively.
Patients in the ITT population required an average of 6.4 intravitreal injections, with the 50 mg (n=40), 100 mg (n=39), 200 mg (n=39) and placebo (n=39) group requiring 6.7, 6.0, 4.7 and 8.1 injections, respectively. In the PP population (n=92), a similar trend was seen. Interestingly, there were several instances in which patients did not require another anti-VEGF injection after the final screening treatment was completed. This was more common in those receiving X-82 than those receiving placebo. X-82 treatment nearly doubled the time needed for retreatment with anti VEGF therapy.
This phase II clinical trial demonstrated statistically significant non-inferiority in visual acuity outcomes in those receiving the oral tyrosine kinase inhibitor X-82 plus PRN anti-VEGF injections when compared with those only receiving placebo and PRN anti VEGF treatments.
In addition to showing non-inferiority in BCVA outcomes, there was a trend towards fewer intravitreal anti-VEGF injections in those receiving X-82 when compared with placebo. This effect did appear to be dose-related, with those in the 200 mg X-82 group, on average, receiving fewer anti-VEGF injections. To further support this dose-related reduction in anti-VEGF injections, there were also several patients who did not require any antiVEGF injections after the initial treatment in the screening phase of the trial.
Those receiving treatment also demonstrated a dose dependent decrease in subretinal fluid on SD-OCT imaging upon completion of the 52-week trial, which is consistent with a decreased need for intravitreal anti-VEGF treatment. Moreover, when analysing the number of fellow eye conversions to exudative AMD, there appeared to be a protective effect of X-82. All of these effects of the study drug were clearly demonstrated despite limited adherence to self-administered dosing.
The study concluded, "Systemic tyrosine kinase activity remains promising yet elusive for the treatment of exudative AMD. Patients receiving X-82 demonstrated non-inferiority in visual acuity compared with those receiving placebo. They also demonstrated a decreased intravitreal anti-VEGF injection burden and several patients were able to stop intravitreal therapy all together while on X-82 therapy. However, the systemic toxicity of this medication continues to limit its use."
Source: Cohen MN, et al. Br J Ophthalmol 2020;0:1–7.
doi:10.1136/bjophthalmol-2020-316511
Dr Ishan Kataria has done his MBBS from Medical College Bijapur and MS in Ophthalmology from Dr Vasant Rao Pawar Medical College, Nasik. Post completing MD, he pursuid Anterior Segment Fellowship from Sankara Eye Hospital and worked as a competent phaco and anterior segment consultant surgeon in a trust hospital in Bathinda for 2 years.He is currently pursuing Fellowship in Vitreo-Retina at Dr Sohan Singh Eye hospital Amritsar and is actively involved in various research activities under the guidance of the faculty.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


