- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Virtual 3D models facilitate personalized treatment of complex acetabular fractures: Study
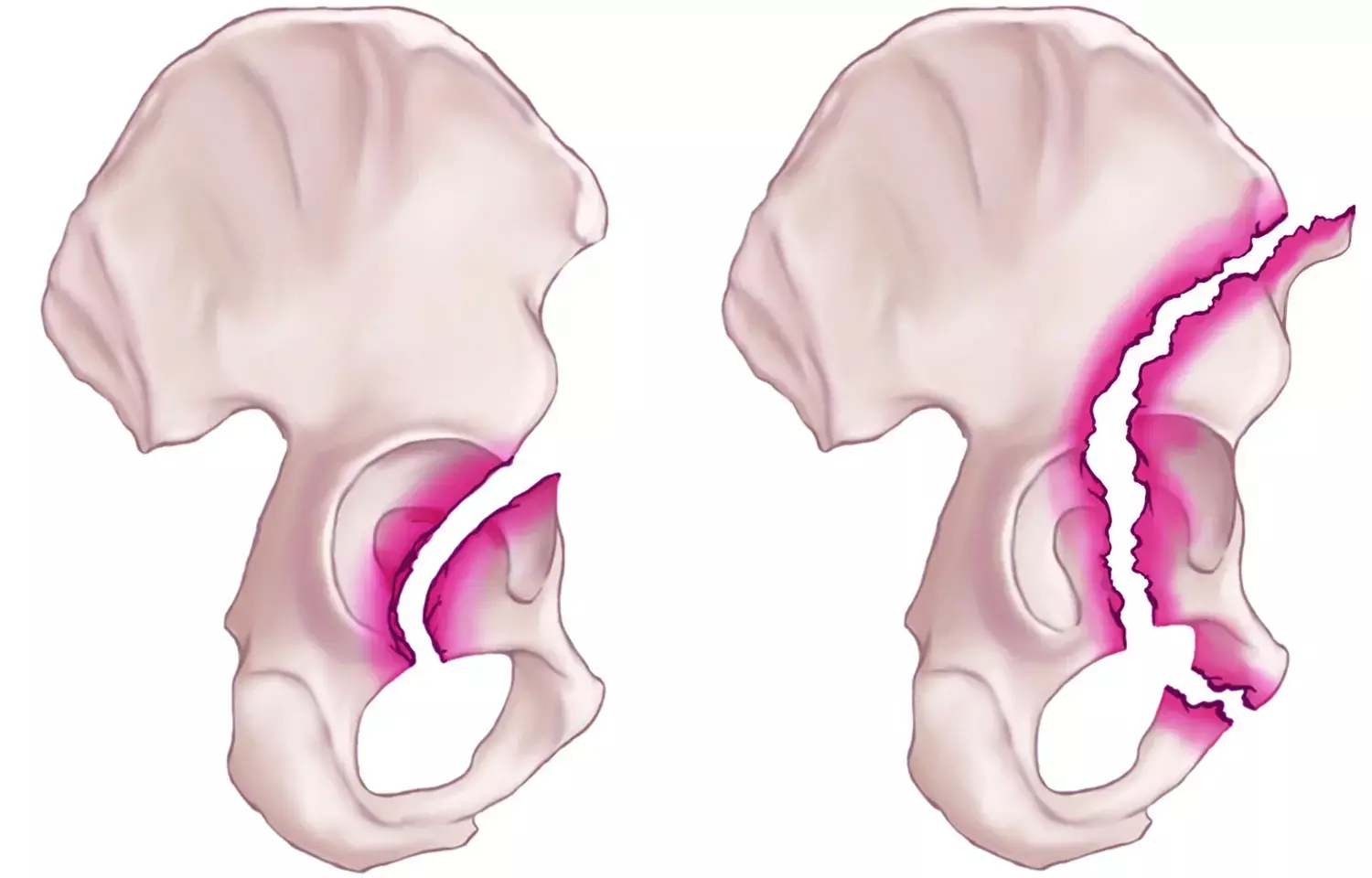
Netherlands: Virtual 3D models based on CT data can be used for providing patient-specific treatments and surgical planning for patients with complex acetabular fractures, finds a recent study in the journal JAMA Network Open.
According to the study, 3-D virtual surgical planning, manufacturing, and clinical application of patient-specific osteosynthesis plates and drilling guides was feasible and yielded good clinical outcomes.
Fast-track personalized surgical treatment could open a new era for complex injuries treatment, the authors noted.
Achieving an optimal reconstruction of the articular surface decreases osteoarthritis risk and the subsequent need for total hip arthroplasty in acetabular fracture surgery. However, owing to the differences in fracture patterns and variations in pelvic anatomy, no one-size-fits-all osteosynthesis plate is available. Currently, plates need to be manually contoured intraoperatively, that often results in inadequate reduction and fixation of the fractured segments.
Frank F. A. IJpma, University Medical Center Groningen, Groningen, the Netherlands, and colleagues, therefore, aimed to determine the feasibility and accuracy of a novel concept of fast-track 3-dimensional (3-D) virtual surgical planning and patient-specific osteosynthesis for complex acetabular fracture surgery.
For the purpose, the researchers performed a case series study that examined the use of patient-specific osteosynthesis plates for patients who required operative treatment for displaced associated-type acetabular fractures at a tertiary university-affiliated referral center and level 1 trauma center between January 1, 2017, and December 31, 2018.
The researchers created 3-D models based on computed tomography (CT) data, fractures were virtually reduced, and implant positions were discussed in a multidisciplinary team of clinicians and engineers. Patient-specific osteosynthesis plates with drilling guides were designed, produced, sterilized and clinically applied within 4 days. Data were analyzed at the 1-year follow-up.
The primary outcome was the quality of the reduction as determined by the postoperative CT scan. The secondary outcomes were accuracy of the screw placement and clinical outcome using patient-reported outcome measures.
The series included a total of 10 patients with an acetabular fracture.
Key findings of the study include:
- The median (interquartile range [IQR]) preoperative gap was 20 mm, and the median (IQR) step-off was 5 mm.
- Postoperatively, the median (IQR) gap was reduced to 3 mm, and the median (IQR) step-off was reduced to 0 mm, indicating good fracture reduction, indicating good fracture reduction.
- The mean difference between the preoperative and postoperative gap was 14.6 mm, and the mean difference in step-off was 5.7 mm.
- The median (IQR) difference in screw direction between the planning and actual surgery was only 7.1°.
- All patients retained their native hip and reported good physical functioning at follow-up.
"These findings suggest that 3-D virtual surgical planning, manufacturing, and clinical application of patient-specific osteosynthesis plates and drilling guides was feasible and yielded good clinical outcomes. Fast-track personalized surgical treatment could open a new era for the treatment of complex injuries," concluded the authors.
The study titled, "Feasibility of Imaging-Based 3-Dimensional Models to Design Patient-Specific Osteosynthesis Plates and Drilling Guides," is published in the journal JAMA Network Open.
DOI: https://jamanetwork.com/journals/jamanetworkopen/article-abstract/2776551
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


