- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Thousands in India die at home from abdominal conditions
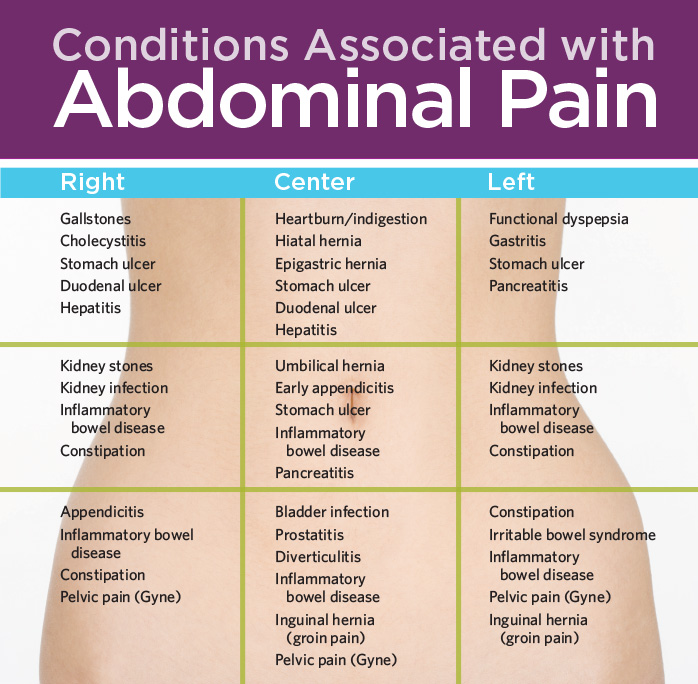
(Reuters Health) - Tens of thousands of people in India die at home each year of conditions such as peptic ulcer disease, appendicitis and hernias they might have survived with timely surgery, a study suggests.
Based on a survey of 1.1 million households in India, researchers estimated that 72,000 people died from acute abdominal conditions in 2010. Most of them died at home and in rural areas, the study found.
Because these conditions must be treated quickly, access to round-the-clock emergency surgical facilities is critical to reduce delays in care and deaths, the researchers note in The Lancet Global Health. But in 2010, just 43 percent of the Indian population lived within 50 kilometers (31 miles) of a well-resourced district hospital.
Many factors, including a lack of health literacy, limited financial resources, and significant geographic barriers to care can influence mortality, said study co-author Dr. Prabhat Jha, a professor of global health at the University of Toronto.
“These barriers typically affect the rural poor the most,” Jha said by email.
To see how much geography influenced deaths from acute abdominal conditions, Jha and colleagues reviewed deaths by postal codes and categorized regions of high and low mortality.
Then the researchers mapped out how far people lived from "well-resourced" district hospitals – that is, facilities with 24-hour surgical and anesthesia services, critical care beds, a blood bank and basic laboratory and radiology departments.
Areas with deaths from acute abdominal conditions were more likely to be poorer, have lower use of gas or other liquid fuels for cooking and slightly lower household density.
About four in five of these deaths were from peptic ulcer disease. Half of the dead were no more than 53 years old, and almost two thirds were men.
Only one in five deaths occurred in a hospital. More than four fifths happened in rural areas.
The hospital deaths suggest that at least some of the dying patients sought care but may have waited too long, lived too far from a hospital to get there quickly or reached a facility that wasn’t equipped to treat them, Jha said.
“This finding is very important for health services planning,” Jha added. “There can be a tendency in emerging economies to focus on building flagship tertiary hospitals in the cities, and in fact India delivers advanced, world class care in many of its large city hospitals. But to prevent deaths from common, treatable surgical conditions such as appendicitis, well-resourced community or district hospitals that are close to the population they serve are really what is needed.”
In an editorial, Drs. Nobhojit Roy and Monty U Khajanchi of BARC Hospital, Mumbai, note that the problem of patients showing up late, and critically ill to hospitals is common in low- and middle-income countries. As a result, surgery is associated in these countries with high mortality and generally poor outcomes.
Building more hospitals doesn’t necessarily mean people will come, said Dr. Adam Kushner, founder and director of Surgeons OverSeas who has researched access to care in developing countries.
“We found that even in the most removed villages, people understood the need for surgery and surgical care, but that mistrust with the health care system or the high cost of care or travel would preclude their seeking assistance,” Kushner said by email.
One limitation of the study, the researchers acknowledge, is the use of postal codes, which may not always provide an accurate way to measure the distance people live from the hospital.
However, the authors also suggest that the findings for acute abdominal conditions would hold true for other health problems requiring emergency surgery where the same level of hospital care would be necessary to increase patients’ survival odds.
SOURCE: bit.ly/1MeZWGO and bit.ly/1M0ickw The Lancet Global Health, online August 13, 2015.
Based on a survey of 1.1 million households in India, researchers estimated that 72,000 people died from acute abdominal conditions in 2010. Most of them died at home and in rural areas, the study found.
Because these conditions must be treated quickly, access to round-the-clock emergency surgical facilities is critical to reduce delays in care and deaths, the researchers note in The Lancet Global Health. But in 2010, just 43 percent of the Indian population lived within 50 kilometers (31 miles) of a well-resourced district hospital.
Many factors, including a lack of health literacy, limited financial resources, and significant geographic barriers to care can influence mortality, said study co-author Dr. Prabhat Jha, a professor of global health at the University of Toronto.
“These barriers typically affect the rural poor the most,” Jha said by email.
To see how much geography influenced deaths from acute abdominal conditions, Jha and colleagues reviewed deaths by postal codes and categorized regions of high and low mortality.
Then the researchers mapped out how far people lived from "well-resourced" district hospitals – that is, facilities with 24-hour surgical and anesthesia services, critical care beds, a blood bank and basic laboratory and radiology departments.
Areas with deaths from acute abdominal conditions were more likely to be poorer, have lower use of gas or other liquid fuels for cooking and slightly lower household density.
About four in five of these deaths were from peptic ulcer disease. Half of the dead were no more than 53 years old, and almost two thirds were men.
Only one in five deaths occurred in a hospital. More than four fifths happened in rural areas.
The hospital deaths suggest that at least some of the dying patients sought care but may have waited too long, lived too far from a hospital to get there quickly or reached a facility that wasn’t equipped to treat them, Jha said.
“This finding is very important for health services planning,” Jha added. “There can be a tendency in emerging economies to focus on building flagship tertiary hospitals in the cities, and in fact India delivers advanced, world class care in many of its large city hospitals. But to prevent deaths from common, treatable surgical conditions such as appendicitis, well-resourced community or district hospitals that are close to the population they serve are really what is needed.”
In an editorial, Drs. Nobhojit Roy and Monty U Khajanchi of BARC Hospital, Mumbai, note that the problem of patients showing up late, and critically ill to hospitals is common in low- and middle-income countries. As a result, surgery is associated in these countries with high mortality and generally poor outcomes.
Building more hospitals doesn’t necessarily mean people will come, said Dr. Adam Kushner, founder and director of Surgeons OverSeas who has researched access to care in developing countries.
“We found that even in the most removed villages, people understood the need for surgery and surgical care, but that mistrust with the health care system or the high cost of care or travel would preclude their seeking assistance,” Kushner said by email.
One limitation of the study, the researchers acknowledge, is the use of postal codes, which may not always provide an accurate way to measure the distance people live from the hospital.
However, the authors also suggest that the findings for acute abdominal conditions would hold true for other health problems requiring emergency surgery where the same level of hospital care would be necessary to increase patients’ survival odds.
SOURCE: bit.ly/1MeZWGO and bit.ly/1M0ickw The Lancet Global Health, online August 13, 2015.
Meghna A Singhania is the founder and Editor-in-Chief at Medical Dialogues. An Economics graduate from Delhi University and a post graduate from London School of Economics and Political Science, her key research interest lies in health economics, and policy making in health and medical sector in the country. She is a member of the Association of Healthcare Journalists. She can be contacted at meghna@medicaldialogues.in. Contact no. 011-43720751
Next Story


