- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Rare case of Colon Cancer Metastases in Surgical Scar reported in NEJM
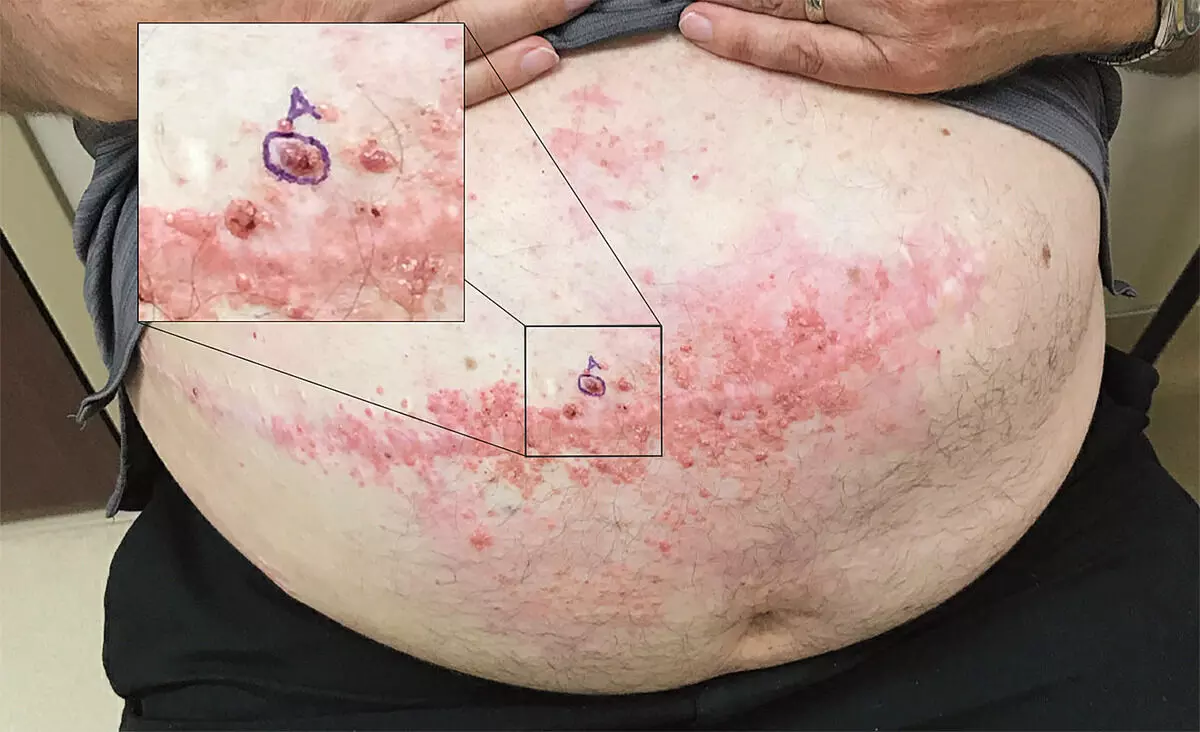 Courtesy New England journal of Medicine
Courtesy New England journal of MedicineDr. Grant Randall and colleagues at the University of Nebraska Medical Center, Omaha, NE have reported a rare case of Colon Cancer Metastases in a Surgical Scar that has been published in the New England Journal of Medicine.
Metastases represent one of the most outstanding characteristics of malignant neoplasms and are relatively rare in the skin, in spite of the great extension of the cutaneous organs.
Skin metastases from colon cancer are rare and usually develop after the primary tumor has manifested. This usually occurs to the scar of incisions used for resection of the colonic tumor itself.
Cutaneous metastases from asymptomatic colonic carcinoma have been documented rarely in the literature. But cutaneous metastasis to an already present operative scar as the mode of presentation of otherwise asymptomatic colon cancer is an extremely rare phenomenon.
Cutaneous metastases when present, indicate a poor prognosis, since more than two thirds of patients die within six months after diagnosis.2
According to history, a 59-year-old man with metastatic colon cancer was referred to the dermatology clinic for a possible case of shingles. He had a 10-week history of painless and nonpruritic skin lesions coalescing around a large abdominal scar from a hemicolectomy performed 3 years earlier. Subsequent liver resection and cholecystectomy had also been performed through this incision. On examination, the lesions were firm, pink to violaceous in color, and vesicular-appearing; the presence of ascites was also evident. In this clinical context, cutaneous metastases were considered most likely, and a skin biopsy confirmed the diagnosis of metastatic colon adenocarcinoma. The most common site of cutaneous metastases in colon adenocarcinoma is the abdominal skin, sometimes in or around surgical scars, as was seen in this case. The patient ultimately received hospice care and died 5 months after this presentation.
For further reference log on to:
New Engl J Med 2020; 382:e90
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


