- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Resurgery or Reopening of first failed macular hole: Which is better?
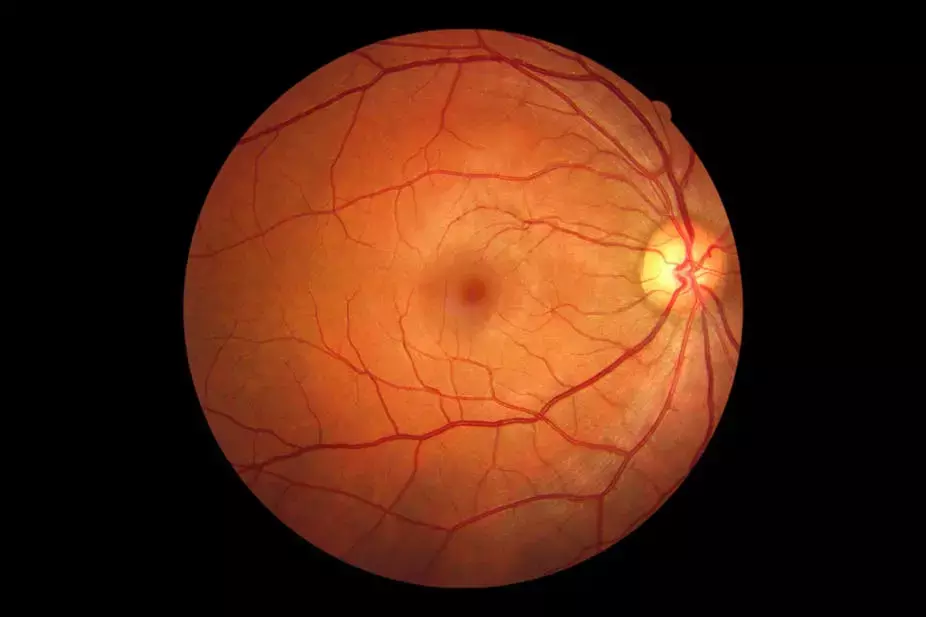
An idiopathic full-thickness macular hole (iFTMH) represents a defect of all neurosensory retinal layers involving the fovea and can result in metamorphopsia and reduced central vision.
Idiopathic full-thickness macular holes result from changes at the vitreomacular interface, which, in turn, lead to perifoveal cortical vitreous traction. If untreated, most iFTMHs will progress in size and grade with increasing central visual loss.
A Systematic review and meta-analysis Pubmed.gov and Cochrane Library were searched by Gerard et al for studies in presenting outcomes of idiopathic full-thickness macular hole that FTC or RO to evaluate repeated surgery for idiopathic full-thickness macular hole that failed to close (FTC) after first surgery or reopened (RO) once originally closed.
Anatomical closure, postoperative best-corrected visual acuity, intraoperative/postoperative complications, and patient-reported outcomes were noted. Meta-analysis was performed on aggregate and available individual participant data sets.
Twenty-eight eligible studies were identified. After reoperation, pooled estimates for anatomical closure were 78% (95% confidence interval 71–84%) and 80% (95% confidence interval 66–89%) for FTC and RO groups, respectively. On average, best-corrected visual acuity improved in both groups. However, only 15% (28 of 189 eyes) of FTC eyes achieved best-corrected visual acuity of ≥6/12. The pooled estimated probability of ≥2-line best-corrected visual acuity improvement was 58% in the FTC group (95% confidence interval 45–71%); meta-analysis was not possible in the RO group. The most common complication was cataract.
The study concluded "Reoperation for FTC or RO idiopathic full-thickness macular hole achieved a clinically meaningful visual acuity improvement in more than half of patients; high levels of vision (≥6/12), however, were uncommon."
This review and meta-analysis indicated , "Just more than half of the patients undergoing a second surgery for FTC iFTMH are likely to experience visual acuity improvement of ≥2 Snellen lines after a second surgery, with a small risk of complications. Only a small proportion of these (15%), however, may achieve very good vision (≥6/12). There was weak evidence that visual success may be higher in the RO group. Repeated surgery is likely to lead to anatomical closure of the iFTMH in a high proportion of patients with FTC and RO iFTMHs (estimated at 78 and 80%, respectively). This information is useful for the counseling of patients before surgery."
doi: 10.1097/IAE.0000000000002564
Dr Ishan Kataria has done his MBBS from Medical College Bijapur and MS in Ophthalmology from Dr Vasant Rao Pawar Medical College, Nasik. Post completing MD, he pursuid Anterior Segment Fellowship from Sankara Eye Hospital and worked as a competent phaco and anterior segment consultant surgeon in a trust hospital in Bathinda for 2 years.He is currently pursuing Fellowship in Vitreo-Retina at Dr Sohan Singh Eye hospital Amritsar and is actively involved in various research activities under the guidance of the faculty.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


