- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Intracoronary hypothermia safe in primary PCI reveal early results of EURO-ICE trial
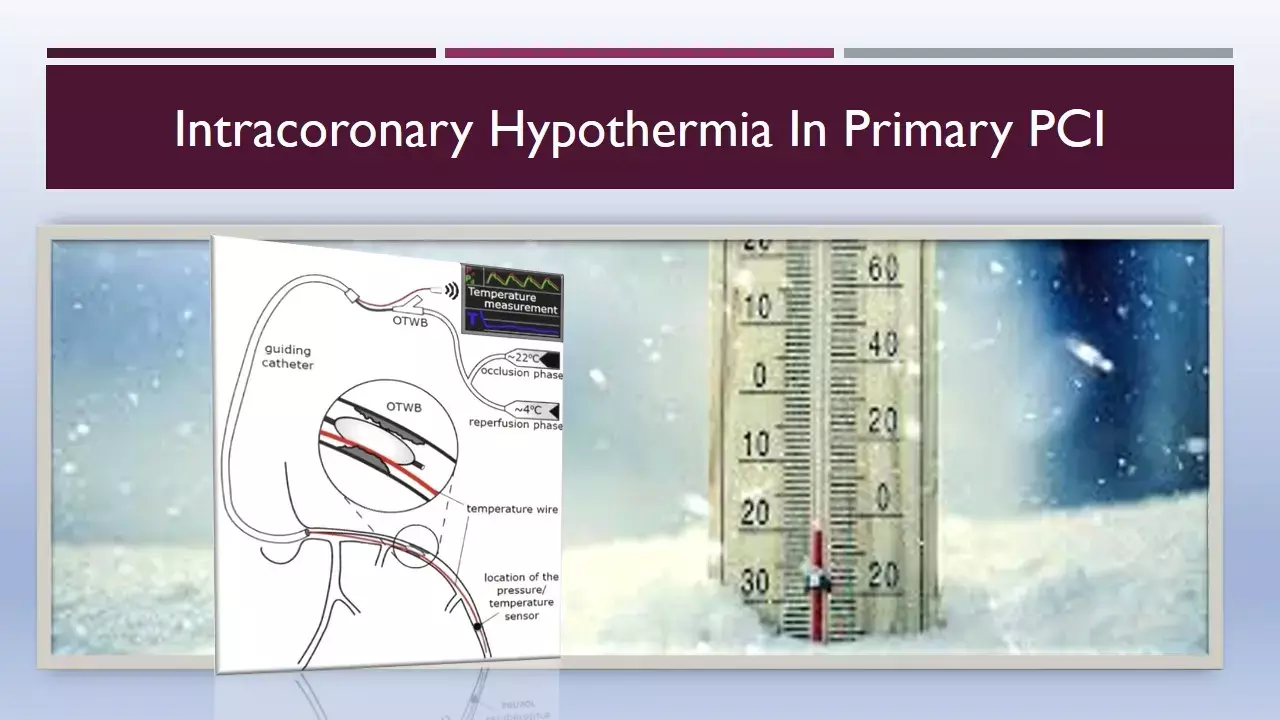
Reperfusion injury may undermine a considerable part of the recovery of the ischemic myocardium achieved by Primary PCI (percutaneous intervention). Selective intracoronary hypothermia is a novel therapy intended to reduce myocardial reperfusion injury and has shown beneficial effects in animal studies.
In the latest issue of JACC: Cardiovascular Interventions, El Farissi et al present preliminary safety results of the EURO-ICE randomized trial and report that selective intracoronary hypothermia during Primary PCI (PPCI) in patients with anterior STEMI can be implemented within the routine of PPCI and seems to be safe.
Experimental studies have consistently shown that hypothermia induced prior to reperfusion significantly reduces infarct size and is more effective if initiated soon after acute coronary occlusion.
Unfortunately, randomized clinical trials using different methods of systemic hypothermia, such as cold saline infusion, endovascular cooling catheters, surface cooling, and peritoneal lavage alone or in different combinations, have so far failed to show significant reduction in infarct size beyond salvage observed by PPCI.
Selective intracoronary hypothermia is a novel treatment designed to reduce myocardial reperfusion injury and is currently being investigated in the ongoing randomized controlled EURO-ICE trial. In the present analysis, 50 patients with anterior STEMI treated with selective intracoronary hypothermia during PPCI were compared for safety with the first 50 patients randomized to the control group undergoing standard PPCI.
In-hospital mortality, occurrence of rhythm or conduction disturbances, stent thrombosis, onset of heart failure during the procedure, and subsequent hospital admission were assessed.
In-hospital mortality was 0%. One patient in both groups developed cardiogenic shock. Atrial fibrillation occurred in 0 and 3 patients, and ventricular fibrillation occurred in 5 and 3 patients in the intracoronary hypothermia group and control group, respectively. Stent thrombosis occurred in 2 patients in the intracoronary hypothermia group; 1 instance was intraprocedural, and the other occurred following interruption of dual-antiplatelet therapy consequent to an intracranial hemorrhage 6 days after enrollment. No stent thrombosis was observed in the control group.
As cooling is limited to the infarcted area, without inducing systemic hypothermia, the method is much more comfortable for the patient and, importantly, obviates the need for complex antishivering protocols. Despite different mechanism of ischemic-area cooling without induction of systemic hypothermia, the decrease in blood temperature within affected myocardium before reperfusion (−6.44°C) appears to be much larger than with the currently most powerful endovascular cooling catheter (−3.0°C).
"Obviously, we are all eagerly awaiting final results in terms of efficacy with the hope that the presented safety profile of the study will be maintained. Selection of the primary effectiveness endpoint, infarct size expressed as a percentage of left ventricular mass assessed on cardiac magnetic resonance at 3 months, is very appropriate", noted Noc et al in an accompanying editorial.
This first report on the safety of selective intracoronary hypothermia during PPCI in patients with anterior STEMI suggests that the procedure can be implemented safely during PPCI without increased risk for complications. The ongoing randomized controlled EURO-ICE study will demonstrate whether selective intracoronary hypothermia will reduce infarct size and improve clinical outcomes.
Source: JACC Cardiovascular Interventions:
1. DOI: 10.1016/j.jcin.2021.06.009
2. DOI: 10.1016/j.jcin.2021.06.037
MBBS, MD , DM Cardiology
Dr Abhimanyu Uppal completed his M. B. B. S and M. D. in internal medicine from the SMS Medical College in Jaipur. He got selected for D. M. Cardiology course in the prestigious G. B. Pant Institute, New Delhi in 2017. After completing his D. M. Degree he continues to work as Post DM senior resident in G. B. pant hospital. He is actively involved in various research activities of the department and has assisted and performed a multitude of cardiac procedures under the guidance of esteemed faculty of this Institute. He can be contacted at editorial@medicaldialogues.in.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


