- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Management of MIH to prevent early posteruptive enamel breakdown- A case report
Dr Simone Bagattoni and colleagues from the Department of Biomedical and Neuromotor Sciences, Unit of Dental Care for Special Needs Patients and Paediatric Dentistry, University of Bologna, Alma Mater Studiorum, Bologna, Italy recently reported an unusual case study where they found out a novel interim approach to prevent early posteruptive enamel breakdown of molar-incisor hypomineralization.
The research is published in the Journal of American Dental Association.
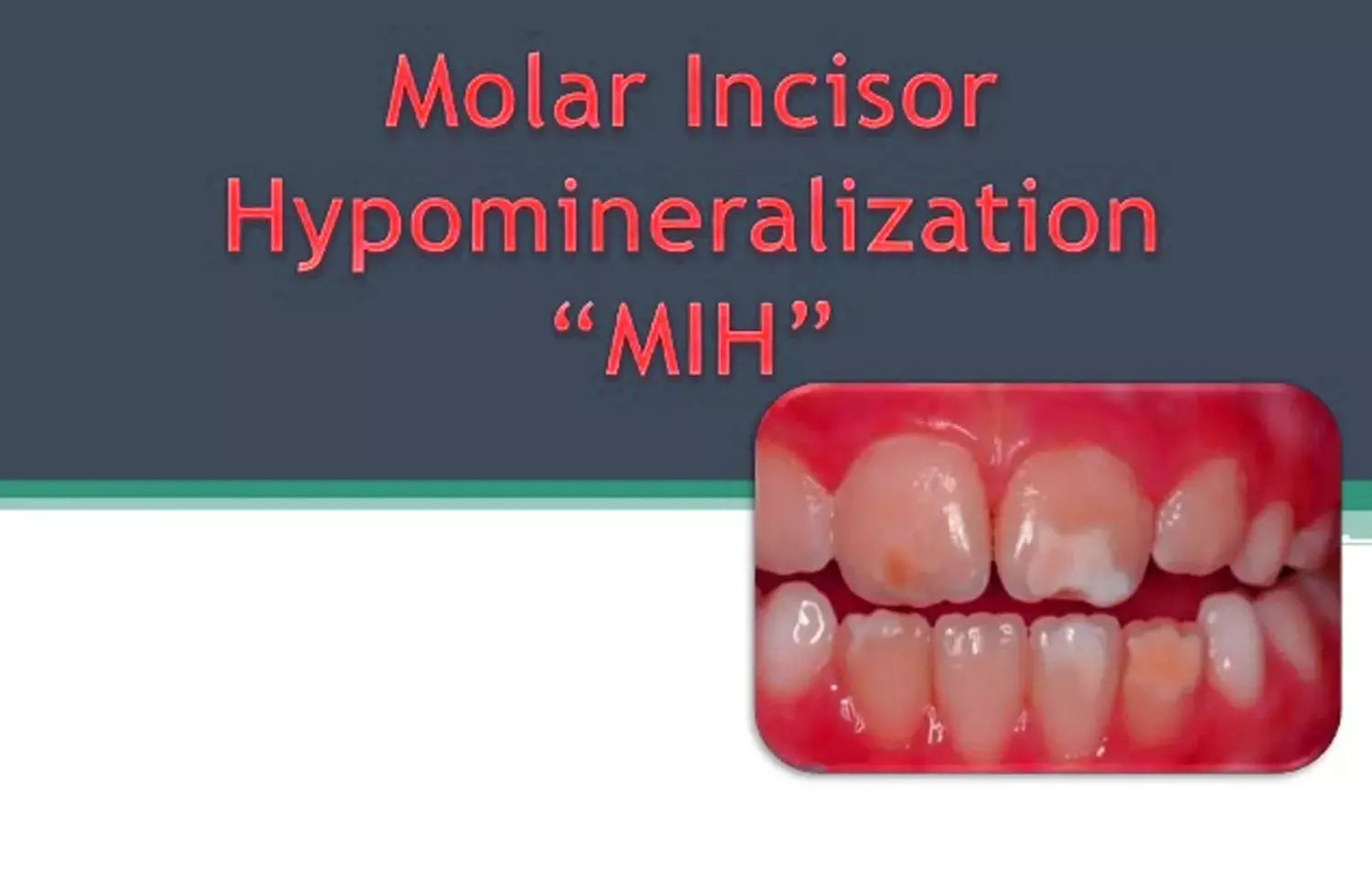
Molar incisor hypomineralization (MIH) is the hypomineralization of systemic origin of one to four permanent first molars, frequently associated with affected incisors. It is a qualitative defect of the enamel. It is also called as hypomineralized permanent first molars (PFMs), idiopathic enamel hypomineralization, nonfluoride hypomineralization, and dysmineralized PFMs.
Severely molar-incisor hypomineralization (MIH)–affected teeth are prone to develop early posteruptive enamel breakdown (PEB) and caries. The characteristic feature of MIH is the clear demarcation between the affected and sound enamel. There is asymmetry of defects present in the molars and incisors where one molar or incisor can be severely affected, while the contralateral tooth may be clinically sound or have only minor defects.
The authors studied the case history of a 6-year-old boy who presented with strong hypersensitivity and extensive brown opacities in the partially erupted mandibular permanent first molars (PFMs), which later was diagnosed with MIH.
Constant hygiene and dietary counseling were planned and followed by the application of luted orthodontic bands and glass ionomer sealants to protect PFMs from caries and PEB until the complete eruption of the teeth.
After 36 months, the PFMs were completely erupted, with no caries and PEB, and the cooperation of the child increased.
This led the authors to conclude that temporary strategies are useful to preserve MIH-affected PFMs.
They further added that with the methodology described, the hypersensitivity decreased in the patient and that the patient reached a good degree of cooperation, making possible definitive rehabilitative considerations for the management of molar incisor hypomineralization.
Dr. Nandita Mohan is a practicing pediatric dentist with more than 5 years of clinical work experience. Along with this, she is equally interested in keeping herself up to date about the latest developments in the field of medicine and dentistry which is the driving force for her to be in association with Medical Dialogues. She also has her name attached with many publications; both national and international. She has pursued her BDS from Rajiv Gandhi University of Health Sciences, Bangalore and later went to enter her dream specialty (MDS) in the Department of Pedodontics and Preventive Dentistry from Pt. B.D. Sharma University of Health Sciences. Through all the years of experience, her core interest in learning something new has never stopped. She can be contacted at editorial@medicaldialogues.in. Contact no. 011-43720751
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


