- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Radiosurgery for Postoperative Metastatic Surgical Cavities: ISRS Practice Guidelines
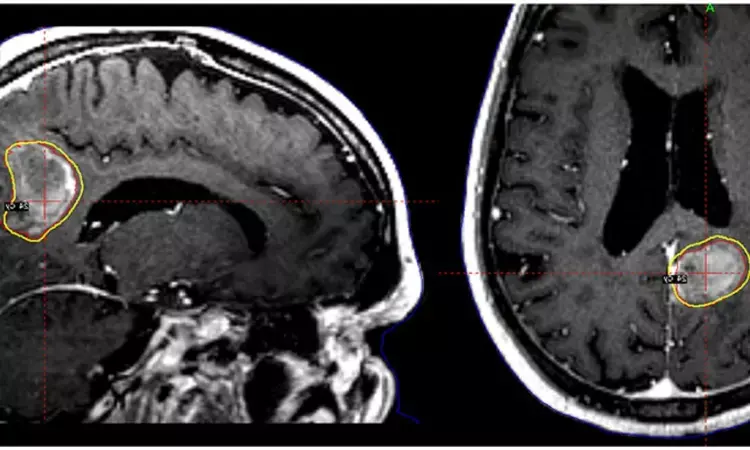
Delhi: The International Stereotactic Radiosurgery Society (ISRS) has released clinical guidance on the delivery of postoperative radiosurgery for brain metastatic surgical cavities.
The purpose of the guideline, published in the International Journal of Radiation Oncology, Biology, Physics, is to summarize the literature specific to single-fraction stereotactic radiosurgery (SRS) and multiple-fraction stereotactic radiation therapy (SRT) for postoperative brain metastases resection cavities and to present practice recommendations on behalf of the ISRS.
Key recommendations include:
- After surgery for a brain metastasis, postoperative SRS is preferred over observation due to superior local control.
- For patients with 1 resected brain metastasis, ECOG performance status of 0-2, and a resection cavity measuring <5 cm, postoperative SRS to the resection cavity is recommended to minimize cognitive toxicity compared with whole-brain radiation therapy.
- Target volume should include the resection cavity and entire surgical tract with consideration to expand the clinical target volume to include a 5-10 mm expansion beyond the preoperative tumor location along bone flap in those tumors contacting the dura preoperatively, while respecting anatomic barriers, and a 1-5 mm expansion along sinuses for tumors contacting a sinus preoperatively. In addition, a 2-3 mm radial expansion to PTV should be considered.
- Prescription doses of approximately 30-50 Gy EQD210, 50-70 EQD25, and 70-90 EQD22, have been associated with reasonable local control, but formal comparative studies are warranted. Emerging data suggest single-fraction treatment without dose de-escalation is appropriate in cavities <2 cm in size and that fractionated regimens may provide superior local control compared with single-fraction SRS in patients with large metastases greater than 2.5-3 cm.
- The consent process for brain metastases surgery should include a discussion of the risk of surgical dissemination of tumor manifesting as leptomeningeal disease.
"Although randomized data raise concern for poorer local control after resection cavity SRS than WBRT, these findings may be driven by factors such as conservative prescription doses used in the SRS arm," wrote the authors. "Retrospective studies suggest high rates of local control after single-fraction SRS and hypofractionated SRT for postoperative brain metastases. With a superior neurocognitive profile and no survival disadvantage to withholding WBRT, the ISRS recommends SRS as first-line treatment for eligible postoperative patients."
"Emerging data suggest that fractionated SRT may provide superior local control compared with single-fraction SRS, in particular, for large tumor cavity volumes/diameters and potentially for patients with a preoperative diameter greater than 2.5 cm," they concluded.
Reference:
"Stereotactic Radiosurgery for Postoperative Metastatic Surgical Cavities: A Critical Review and International Stereotactic Radiosurgery Society (ISRS) Practice Guidelines," is published in the International Journal of Radiation Oncology, Biology, Physics.
MSc. Biotechnology
Medha Baranwal holds a Bachelor’s degree in Biomedical Sciences from the University of Delhi and a Master’s degree in Biotechnology from Amity University. Since May 2018, she has been contributing to Medical Dialogues, writing and editing medical news articles that translate complex research into clear, accessible information for healthcare professionals.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


