- Home
- Medical news & Guidelines
- Anesthesiology
- Cardiology and CTVS
- Critical Care
- Dentistry
- Dermatology
- Diabetes and Endocrinology
- ENT
- Gastroenterology
- Medicine
- Nephrology
- Neurology
- Obstretics-Gynaecology
- Oncology
- Ophthalmology
- Orthopaedics
- Pediatrics-Neonatology
- Psychiatry
- Pulmonology
- Radiology
- Surgery
- Urology
- Laboratory Medicine
- Diet
- Nursing
- Paramedical
- Physiotherapy
- Health news
- Fact Check
- Bone Health Fact Check
- Brain Health Fact Check
- Cancer Related Fact Check
- Child Care Fact Check
- Dental and oral health fact check
- Diabetes and metabolic health fact check
- Diet and Nutrition Fact Check
- Eye and ENT Care Fact Check
- Fitness fact check
- Gut health fact check
- Heart health fact check
- Kidney health fact check
- Medical education fact check
- Men's health fact check
- Respiratory fact check
- Skin and hair care fact check
- Vaccine and Immunization fact check
- Women's health fact check
- AYUSH
- State News
- Andaman and Nicobar Islands
- Andhra Pradesh
- Arunachal Pradesh
- Assam
- Bihar
- Chandigarh
- Chattisgarh
- Dadra and Nagar Haveli
- Daman and Diu
- Delhi
- Goa
- Gujarat
- Haryana
- Himachal Pradesh
- Jammu & Kashmir
- Jharkhand
- Karnataka
- Kerala
- Ladakh
- Lakshadweep
- Madhya Pradesh
- Maharashtra
- Manipur
- Meghalaya
- Mizoram
- Nagaland
- Odisha
- Puducherry
- Punjab
- Rajasthan
- Sikkim
- Tamil Nadu
- Telangana
- Tripura
- Uttar Pradesh
- Uttrakhand
- West Bengal
- Medical Education
- Industry
Vesicoureteral reflux severity after ureteroneocystostomy may not increase catheterization need or hospital stay
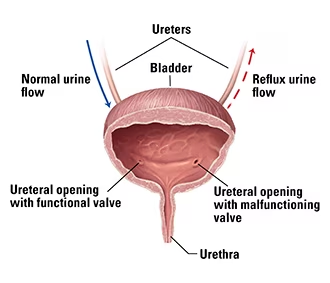
Severity of Vesicoureteral reflux after ureteroneocystostomy not tied to increased need for catheterization or prolonged hospital stay suggests a new study published in the Journal of Pediatric Urology.
Vesicoureteral reflux (VUR) is a common urologic condition affecting approximately 1% of all children. Surgical success often depends on the grade of VUR, as patients with grades 4 or 5 have been have a greater risk for postoperative complications. Unplanned urinary catheter placement (UCP) postoperatively and prolonged length of hospital stay (LOS) are indicative of unexpected complications. The association between VUR severity and such metrics remain unclear.
The study's objective is to determine if the severity of VUR is associated with higher rates of UCP or prolonged LOS after ureteroneocystostomy (UNC).
The 2020 National Surgical Quality Improvement Program Pediatric database was analyzed for patients with VUR. A total of 1742 patients were initially evaluated with 1373 meeting exclusion criteria. The patients were divided into 3 groups of varying voiding cystourethrogram (VCUG) or radionuclide cystogram (RNC) severity: VCUG Grade 1 or RNC Grade 1 (Group A), VCUG Grade 2 or 3 or RNC Grade 2 (Group B), and VCUG Grade 4 or 5 or RNC Grade 3 (Group C). Basic statistical analysis was performed, and logistic regression was performed with both UCP and LOS as dependent variables.
Results
Among the 1373 patients, 2.9% were included in Group A, 32.5% were in Group B, and 64.6% were in Group C. Significant differences were found among the groups for mean age, gender, inpatient status, rate of congenital malformation, ureteral stents, and ASA classification. Regarding surgical treatment, differences were also found comparing mean operative time, LOS, laterality and type of procedure, urine culture results, rates of UTI, surgical site infections, postoperative returns to the emergency department, and unplanned procedures and catheterization. Multivariate analysis demonstrated no significant association between the rate of UCP and VUR severity, while postoperative UTI and unplanned procedure were both independent factors associated with UCP postoperatively. Additionally, postoperative UTI, ASA classification, mean operation time, ureteral stent placement, unplanned procedure, and UCP were independent factors found to contribute to LOS.
Greater VUR severity does not appear to increase the need for catheterization or prolong hospital stay, while the development of a UTI postoperatively or having an additional unplanned procedure are associated with an increased likelihood of both. The postoperative course after UNC also appears to be influenced more so by other factors such as the operative approach and whether complications arise
Keywords:
Reference:
Mark E. Quiring, Young Son, Ranel Thaker, Noah Davidson, Edward Wu, Benjamin A. Fink, Brian Thomas, Nathaniel B. Gentry, Angie Yossef, Virgil K. DeMario, Lance Earnshaw, Blen Weldekidan, Gregory Dean. Vesicoureteral reflux severity is not associated with unplanned urinary catheterization or length of hospital stay after ureteroneocystostomy,
Journal of Pediatric Urology,
2023, ISSN 1477-5131. https://doi.org/10.1016/j.jpurol.2023.08.034.
(https://www.sciencedirect.com/science/article/pii/S1477513123003935)
Keywords:
Severity, of, Vesicoureteral, reflux, after, ureteroneocystostomy, not, tied, increased, need, catheterization, prolong, hospital, stay, Journal of Pediatric Urology, Ureteral reimplantation; Ureteroneocystostomy; Vesicoureteral reflux; Length of stay; Unplanned catheterization, Mark E. Quiring, Young Son, Ranel Thaker, Noah Davidson, Edward Wu, Benjamin A. Fink, Brian Thomas, Nathaniel B. Gentry, Angie Yossef, Virgil K. DeMario, Lance Earnshaw, Blen Weldekidan, Gregory Dean
Dr. Shravani Dali has completed her BDS from Pravara institute of medical sciences, loni. Following which she extensively worked in the healthcare sector for 2+ years. She has been actively involved in writing blogs in field of health and wellness. Currently she is pursuing her Masters of public health-health administration from Tata institute of social sciences. She can be contacted at editorial@medicaldialogues.in.
Dr Kamal Kant Kohli-MBBS, DTCD- a chest specialist with more than 30 years of practice and a flair for writing clinical articles, Dr Kamal Kant Kohli joined Medical Dialogues as a Chief Editor of Medical News. Besides writing articles, as an editor, he proofreads and verifies all the medical content published on Medical Dialogues including those coming from journals, studies,medical conferences,guidelines etc. Email: drkohli@medicaldialogues.in. Contact no. 011-43720751


